On this page
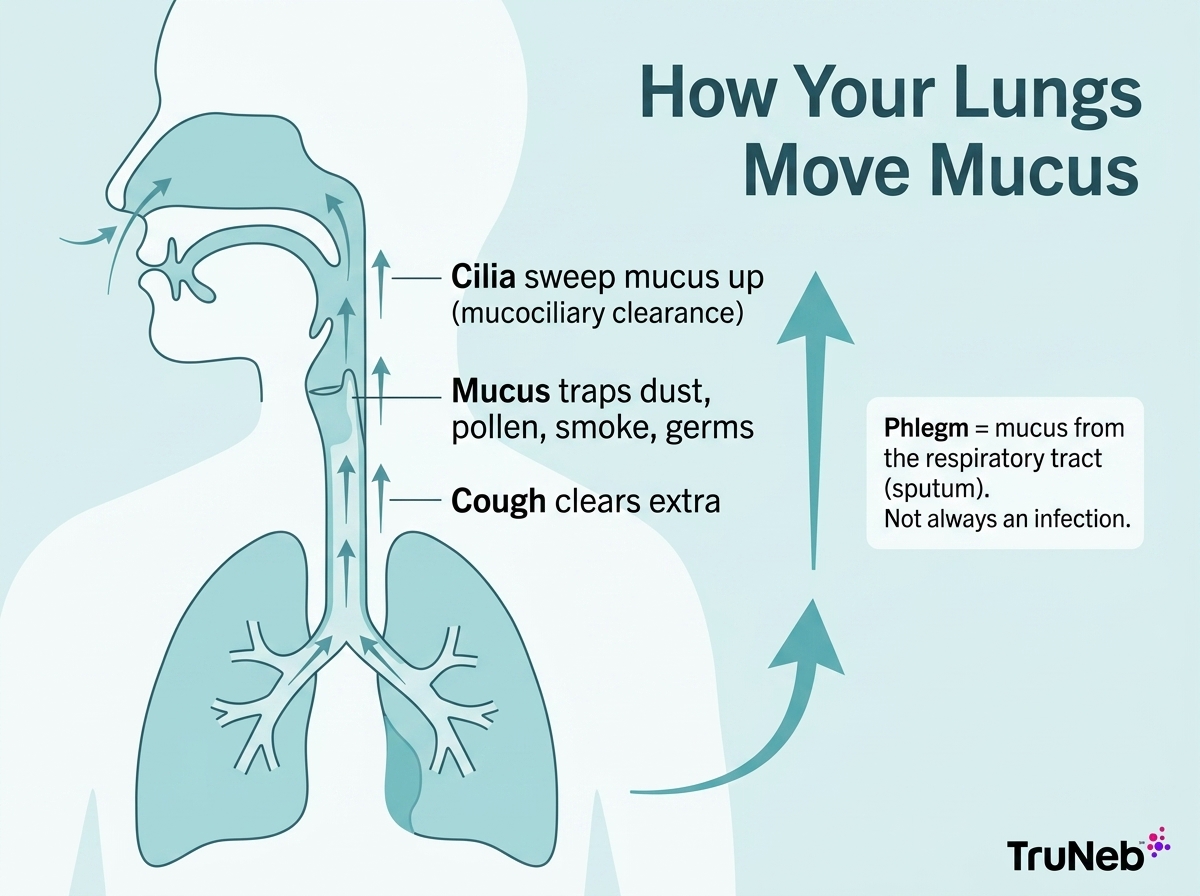
Coughing up phlegm even when you don’t feel sick can happen. Your airways make mucus every day to trap dust, pollen, smoke, and germs. Tiny hair-like cilia sweep that mucus upward (mucociliary clearance) so you can swallow it quietly or cough it out.
Phlegm is mucus from the respiratory tract. When it comes from the lower airways, doctors often call it sputum. A productive cough simply means you’re bringing up mucus, which can be protective.
Feeling well lowers the chance of a cold or flu, but it doesn’t rule out allergies, reflux, asthma, smoke irritation, or chronic airway conditions. What matters most is the pattern: how long it lasts, how much there is, what it looks like, and which symptoms show up with it.
Normal mucus is thin and usually clear. It shifts with seasons, indoor dryness, and irritants. It’s more concerning when it hangs around, increases, turns bloody, or comes with wheezing, shortness of breath, chest pain, fever, weight loss, or voice changes.
Quick distinction: throat mucus usually feels like drainage, frequent throat clearing, or a lump sensation, while lung phlegm tends to come up with a deeper chest cough, chest congestion, wheeze, or breathlessness.
Key point: Feeling “not sick” lowers the chance of an acute infection, but persistent or changing phlegm still deserves attention.
Common Reasons You May Cough Up Phlegm Without Feeling Sick
Coughing up phlegm without feeling sick usually points to irritation, inflammation, or drainage rather than a sudden infection.
Allergies and Postnasal Drip
Allergic rhinitis and sinus irritation can ramp up mucus in your nose and sinuses. That extra mucus can drip down the back of your throat and trigger a cough, especially at night. You might notice sneezing, itchy eyes, congestion, and a drainage feeling. Mucus is often clear or white. Some people use a saline nasal rinse for nasal symptoms; ask your doctor if it’s a good fit and how to use it safely.
Asthma and Airway Inflammation
Asthma can cause cough, chest tightness, wheeze, and mucus. Some people have cough-variant asthma where cough is the main sign. Sticky, thick phlegm can show up when airway inflammation isn’t well controlled. Nighttime or early-morning cough is common.
GERD and Silent Reflux
Acid irritation from GERD or laryngopharyngeal reflux (LPR) can lead to throat mucus and chronic cough. You might not feel heartburn. Clues include hoarseness, a lump sensation in the throat, throat clearing, sour taste, or cough after meals or when lying down.
Smoking, Vaping, and Irritants
Cigarette smoke, vaping aerosols, dust, fumes, wildfire smoke, and air pollution irritate the airways. Your body can make more mucus to trap these particles. A daily morning cough with phlegm is common in smokers and shouldn’t be brushed off.
Dry Air and Dehydration
Dry indoor air and low fluid intake thicken mucus. Thick mucus moves slowly and can feel stuck, even when you’re otherwise fine. Using humidified air and staying hydrated can make mucus easier to clear for some people. If dryness is a major factor, understanding the difference between a nebulizer vs humidifier may help you discuss options with your clinician.
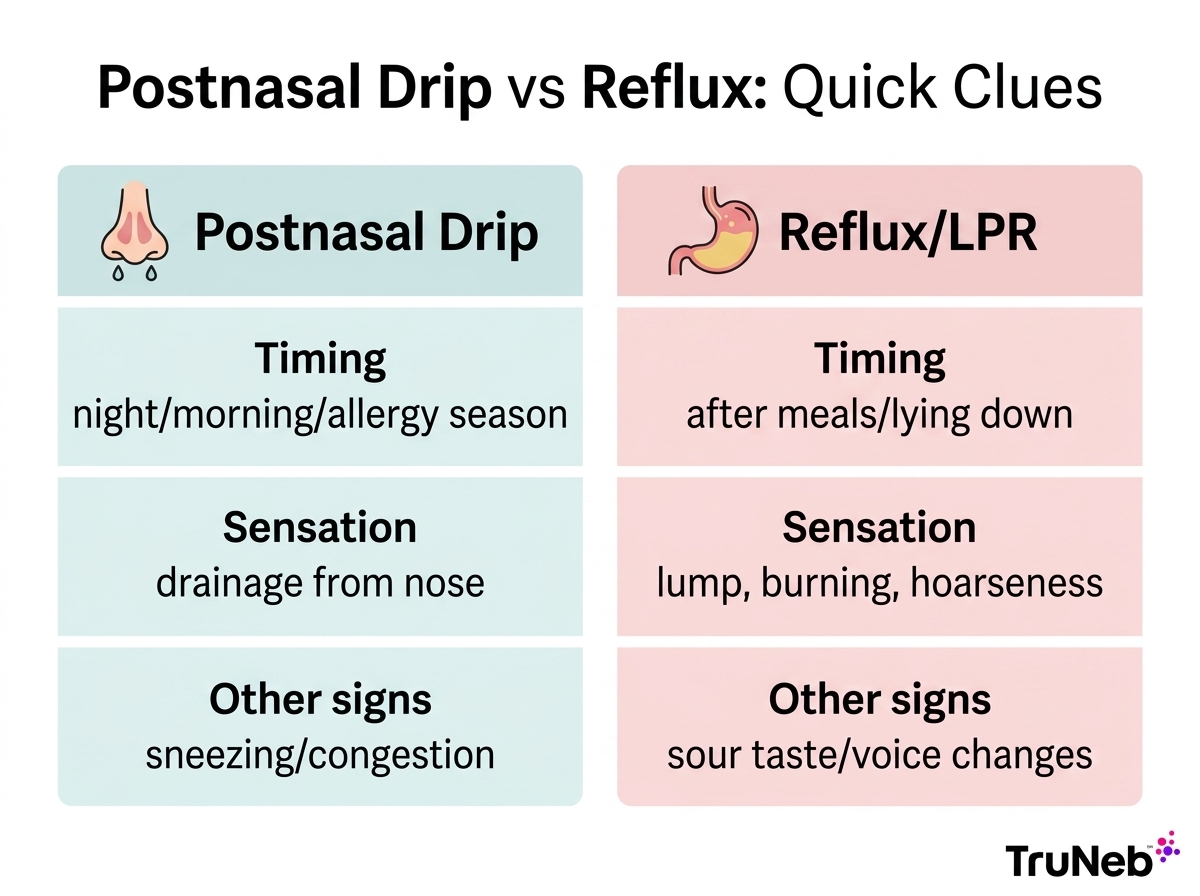
Postnasal drip usually feels like drainage from the nose, while reflux mucus is more likely to flare after meals or when lying down.
| Clue | Points to Postnasal Drip | Points to Reflux/LPR |
|---|---|---|
| Timing | Night or on waking; allergy season | After meals; when lying down or overnight |
| Sensation | Drainage from nose to throat, need to clear throat | Lump-in-throat, burning, sour taste, hoarseness |
| Other clues | Sneezing, itchy eyes, nasal stuffiness | Voice changes, cough after eating or at bedtime |
These can overlap. If you’re not sure, a doctor can look at your nose, throat, and reflux pattern to figure out the main driver.
When Ongoing Phlegm Points to a Chronic Airway Problem
Phlegm that lasts for weeks or keeps coming back can be a sign of asthma, COPD, bronchiectasis, reflux, or another ongoing condition.
Coughing Up Phlegm for Weeks or Months
A cough with phlegm that lasts several weeks is worth getting checked. A chronic productive cough can come from upper airway cough syndrome (postnasal drip), GERD, asthma, COPD, bronchiectasis, or repeated infections. Duration matters even if the mucus is clear. Note how long it’s lasted and whether it’s daily.
What COPD Mucus Can Look Like
People with COPD often notice clear, white, frothy, cloudy, yellow, or green sputum at baseline. COPD includes chronic bronchitis and emphysema; daily phlegm is especially common in chronic bronchitis. A change in amount, thickness, or color can signal a flare-up or infection, especially with more breathlessness, wheeze, or chest tightness. You can compare symptom patterns in this guide to asthma vs COPD differences.
Bronchiectasis and Daily Phlegm
Bronchiectasis damages airway walls and traps mucus. Daily cough with a lot of phlegm, frequent chest infections, breathlessness, or coughing blood are common signs. Airway clearance is often part of care. Doctors often confirm bronchiectasis with a chest CT and sometimes sputum tests.
If phlegm is a daily pattern for months, schedule a visit. Simple tests like spirometry or a chest X-ray can help show what’s going on. Early care can reduce flare-ups and protect your lungs.
What Phlegm Color, Texture, and Amount Can Tell You
Phlegm color can offer clues, but the bigger warning signs are persistence, increasing amount, blood, and breathing symptoms.
Clear or White Phlegm
Usually linked to allergies, irritation, reflux, asthma, or your personal baseline. If it builds up, lasts, or comes with wheeze or breathlessness, it still matters.
Yellow or Green Phlegm
Can show up with infection or inflammation. Color alone can’t diagnose the cause or tell if you need antibiotics. Fever, chest pain, shortness of breath, and worsening patterns add context.
Brown, Black, Pink, Red, or Bloody Phlegm
Brown or rust-colored can point to old blood or certain infections. Black can reflect smoke or dust exposure. Pink or new frothy white sputum with shortness of breath can be linked to heart failure and needs urgent care. Red or bloody phlegm (more than small streaks) needs prompt medical advice; less often, blood in mucus is tied to pulmonary embolism, tuberculosis, or lung cancer. For related color patterns, see guides on brown phlegm causes, black mucus from throat, and pink frothy sputum emergency signs.
Thick, Sticky, or Jelly-Like Mucus
Thick mucus can follow dehydration, dry air, asthma, COPD, or chronic lung disease. Texture matters alongside volume and symptoms.
When to Monitor, Book a Visit, or Seek Urgent Care
Think about timing: several days and improving, beyond 2 to 3 weeks, or recurring for months or daily.
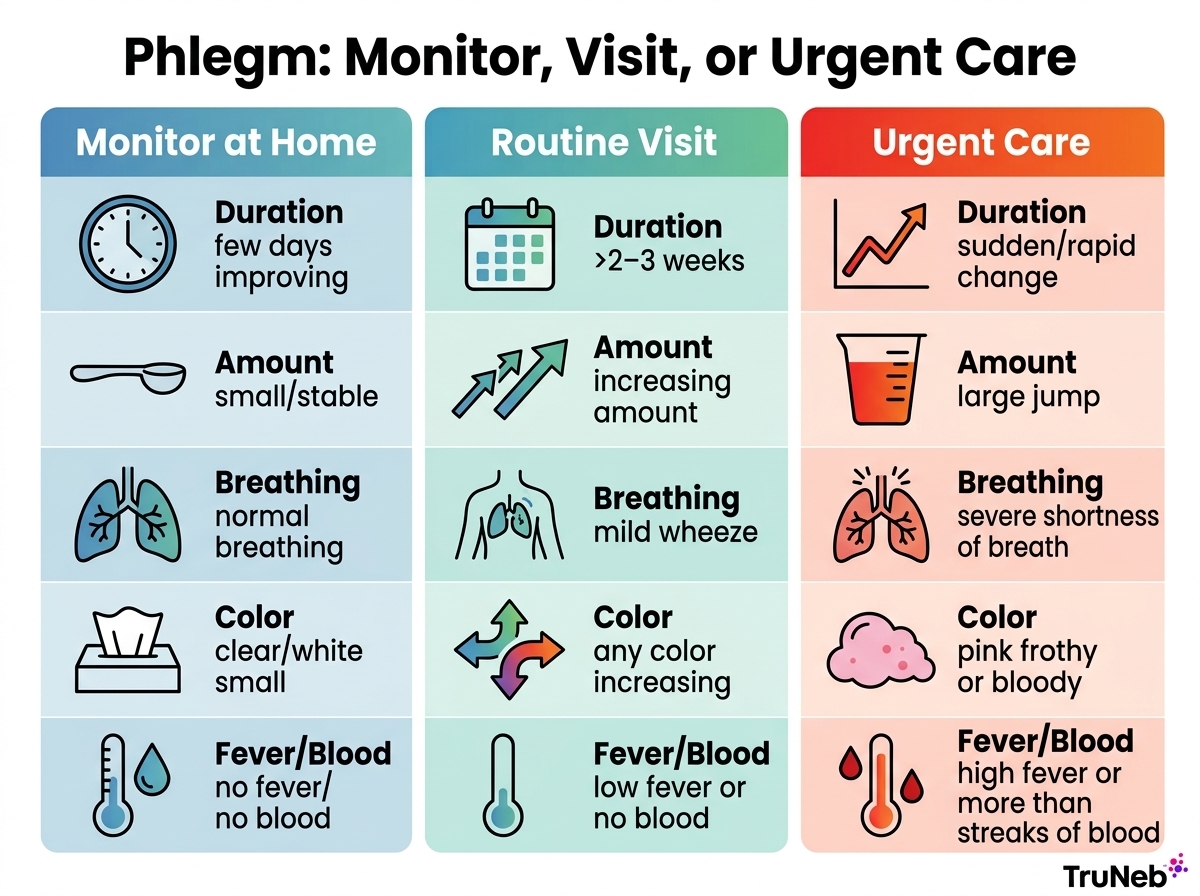
Monitor at Home if Symptoms Are Mild and Improving
Small amounts of clear or white phlegm, no fever, no chest pain, no shortness of breath, and no blood. If symptoms fit known triggers like allergies, dry air, or a recent irritant and are improving over several days, continue fluids and gentle airway care.
Book a Routine Medical Visit if Phlegm Persists or Keeps Returning
A cough or phlegm that lasts beyond 2 to 3 weeks, new daily morning phlegm, or recurring episodes should be checked. Also book a visit for increases in amount or thickness, wheeze or mild breathlessness, persistent hoarseness or reflux symptoms, difficulty swallowing, or a history of asthma, COPD, smoking, vaping, bronchiectasis, or heart disease. Your doctor might order spirometry or a chest X-ray to help decide next steps.
Seek Urgent Care for Red Flags
Blood beyond small streaks, severe shortness of breath, chest pain, blue lips, confusion, high or persistent fever, pink frothy sputum with breathing trouble, fainting, rapid worsening, or marked weight loss or night sweats with persistent cough. Don’t delay if your breathing feels unsafe.
Key point: Judge phlegm by the pattern, not color alone.
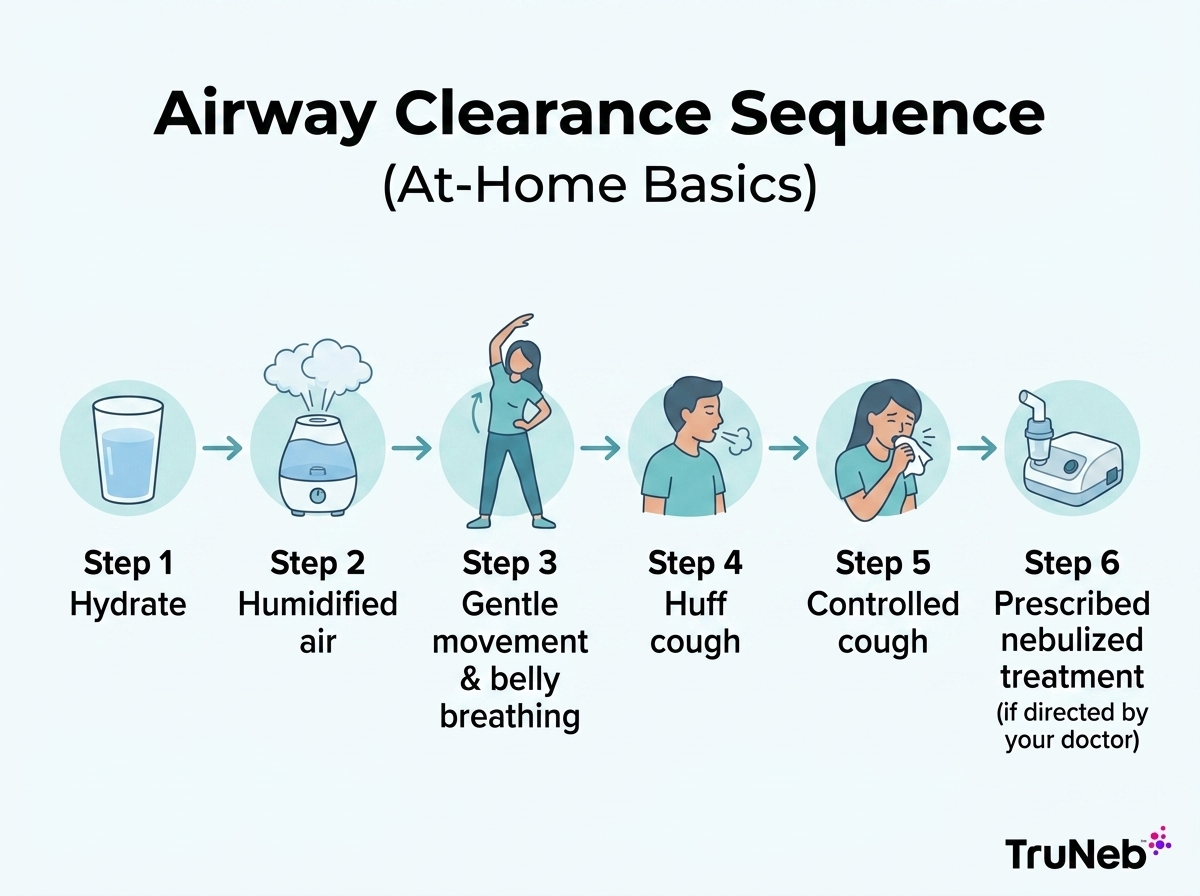
How to Clear Mucus From the Lungs at Home
Home care can help loosen mucus, but it shouldn’t replace medical evaluation when phlegm keeps returning or comes with red flags.
Hydration, Humidified Air, and Warm Fluids
Staying hydrated can make mucus easier to clear for some people. A cool-mist humidifier can ease dryness. Warm tea or broth might soothe your throat. Avoid smoke, strong fumes, and dusty rooms when you can.
Gentle Movement and Positioning
Easy walking and belly breathing invite deeper breaths that help move mucus. Elevating your head at night can reduce reflux or postnasal drip. Postural drainage uses gravity to shift mucus, but if you have reflux, severe breathlessness, heart problems, or are pregnant, ask your doctor before trying positions.
Controlled Coughing and Huff Coughing
Some people are taught breathing and cough techniques to help move mucus. If your doctor has recommended airway clearance, common examples include controlled coughing and huff coughing. Sit upright. Take a slow, deep breath. Hold 2 to 3 seconds. Cough two or three short coughs using your belly muscles, then rest. For a huff cough, take a medium breath in, then exhale with a gentle “ha” to move mucus without squeezing your throat. Stop if you feel dizzy, have chest pain, or severe shortness of breath.
For some chronic lung conditions, a respiratory therapist teaches chest percussion or device-based airway clearance. Ask your care team what’s right for you.
If your doctor suggests it, an over-the-counter expectorant like guaifenesin can sometimes help thin mucus. Avoid starting mucolytics or any nebulized solutions on your own.
What Not to Do
Don’t ignore persistent symptoms. Don’t use someone else’s inhaler, antibiotics, or nebulized medication. Don’t try to fully suppress a productive cough unless your doctor advises it. Don’t assume colored mucus means you need antibiotics—context matters.
⚠️ If you have severe shortness of breath, chest pain, blue lips, confusion, or blood in your mucus, seek urgent medical care instead of trying to manage it at home.
Safety note: Talk to your doctor before trying a new medication or any nebulized solution.
Where Nebulized Saline May Fit Into a Provider-Guided Plan
Nebulized saline is usually reserved for selected patients as part of a doctor-guided mucus-clearing plan.
How Nebulized Saline Can Help Thin Stubborn Mucus
Some people with chronic mucus conditions use nebulized saline under a doctor’s guidance. Isotonic saline (0.9%) is similar to body fluids, while hypertonic saline (such as 3% or 7%) draws water into airway mucus so it can move more easily. It’s commonly discussed in bronchiectasis and cystic fibrosis care and can be part of a COPD plan for selected patients. It can trigger coughing or bronchospasm in some people, so it should be used only if your doctor recommends it. Not everyone with mucus needs a nebulizer. This is usually considered for specific chronic diagnoses, not routine undiagnosed phlegm.
How TruNeb Fits Into Airway Clearance
A portable mesh nebulizer like the TruNeb™ Portable Mesh Nebulizer can be used to deliver prescribed saline or other nebulized treatments as part of your airway clearance routine. It belongs alongside hydration, trigger control, gentle clearance techniques, any prescribed inhalers, and follow-up care. A nebulizer doesn’t tell you why you’re coughing up phlegm. It only fits in when a doctor has already recommended nebulized treatment.
Don’t start nebulized saline on your own just because you have mucus. Ask your doctor whether it makes sense for your symptoms and diagnosis before making any changes. If prescribed, compare options in this overview of hypertonic saline nebulizers.
What a Clinician May Check if Phlegm Persists
A doctor usually looks at timing, triggers, mucus changes, and breathing symptoms before deciding which tests are worth doing.
Questions Your Doctor May Ask
How long has this been happening? What time of day is it worse? What color and how much? What makes it better or worse (meals, lying down, allergens, exercise, cold air)? Do you smoke or vape? Do you have asthma, COPD, reflux, or allergies? Any fever, weight loss, breathlessness, chest pain, or blood? What have you already tried?
What to track and bring:
- How long it’s been going on and whether it’s daily
- Color, thickness, and amount
- Time of day or season
- Triggers (allergens, meals, lying down, cold air, exercise, smoke)
- Breathing symptoms (wheeze, shortness of breath, chest tightness)
- Red flags (blood, fever, chest pain)
Tests That May Be Considered
A lung and ENT exam, oxygen saturation (pulse oximetry), and possibly a chest X-ray. Spirometry can check for asthma or COPD. A sputum culture might look for infection. If bronchiectasis or another chronic lung issue is suspected, a chest CT can help. Allergy testing, nasal endoscopy, or reflux testing (endoscopy or pH probe) are used when clues point to those sources.
You don’t need to diagnose yourself. Bring a simple symptom diary and review it with your doctor. That teamwork can speed up the right next step.
Quick Glossary of Phlegm Terms
Mucus: A slippery fluid that lines and protects your airways and traps dust, pollen, and germs.
Phlegm: Mucus from the respiratory tract. When coughed up, it’s often called sputum.
Sputum: Mucus that’s brought up from the lower airways by a productive cough.
Productive cough: A cough that brings up mucus or sputum.
Postnasal drip: Excess mucus from the nose and sinuses that drains down the back of the throat and can cause cough.
GERD: Gastroesophageal reflux disease, where stomach acid flows back into the esophagus and can irritate the throat.
LPR: Laryngopharyngeal reflux, a form of reflux that often causes throat symptoms without classic heartburn.
COPD: Chronic obstructive pulmonary disease, which includes chronic bronchitis and emphysema.
Bronchiectasis: A chronic condition where damaged airways trap mucus and cause daily phlegm and repeated chest infections.
Hypertonic saline: A salty nebulized solution (for example, 3% or 7%) that some doctors prescribe to help thin thick airway mucus.
Airway clearance: Breathing, positioning, and cough techniques, sometimes with prescribed devices or solutions, used to move mucus out of the lungs.
Key Takeaways
- Coughing up phlegm but not feeling sick is usually tied to allergies, postnasal drip, reflux, asthma, irritants, dry air, or chronic airway conditions.
- Clear or white phlegm is often less concerning, but persistence or a bigger amount still matters.
- Throat mucus (drainage, throat clearing) is different from lung phlegm (deep chest cough, congestion, wheeze).
- See a doctor if phlegm lasts more than 2 to 3 weeks, keeps coming back, or comes with wheeze, breathlessness, chest pain, fever, or blood.
- Helpful home steps include fluids, humidified air, trigger control, gentle movement, and controlled or huff coughing—stop and seek care for red flags.
- A portable nebulizer like TruNeb™ can be used to deliver doctor-prescribed saline as part of a provider-guided plan for stubborn mucus; it doesn’t replace an evaluation.
Frequently Asked Questions
Tap or click a question below to see the answer:
Irritation, allergies with postnasal drip, reflux, asthma, smoke or vaping, dry air, and dehydration can all raise mucus even when you feel fine. If it lasts beyond 2–3 weeks or keeps coming back, book a visit.
It happens. Your airways make mucus daily. Get checked sooner if there’s blood, pink frothy mucus, chest pain, fever, severe shortness of breath, or rapid worsening.
More than 2–3 weeks, daily for months, or repeat episodes are reasons to see a doctor. Go sooner for red flags like blood or breathing trouble.
Go now for blood beyond small streaks, severe shortness of breath, chest pain, blue lips, confusion, high or persistent fever, fainting, or new pink/frothy sputum with breathing trouble.
Stay hydrated, use humidified air, avoid smoke and strong fumes, and practice doctor-taught techniques like huff or controlled coughing. Don’t assume colored mucus means you need antibiotics, and don’t use someone else’s inhaler or nebulizer medicine.
Drainage feeling, sneezing, and congestion lean toward postnasal drip. Hoarseness, sour taste, and worse after meals or when lying down lean toward reflux. They can overlap—your doctor can help sort it out.
Yes. Laryngopharyngeal reflux (silent reflux) can cause throat mucus, hoarseness, a lump sensation, and throat clearing without classic heartburn.
It can be clear, white, frothy, cloudy, yellow, or green. A change from your usual—plus more breathlessness or wheeze—can signal a flare-up.
TruNeb™ is a portable mesh nebulizer that can be used to deliver doctor-prescribed saline or other treatments for selected patients. It should be part of a doctor-guided plan and doesn’t replace an evaluation.
Dry air, low fluids, irritation, asthma, or chronic lung disease can thicken mucus. If it doesn’t improve or you have breathing symptoms, see your doctor.
Disclaimer: This article is for informational purposes only and isn’t a substitute for medical advice, diagnosis, or treatment. Talk to your doctor about your symptoms and treatments.