On this page
What Are the Two Readings on a Pulse Oximeter
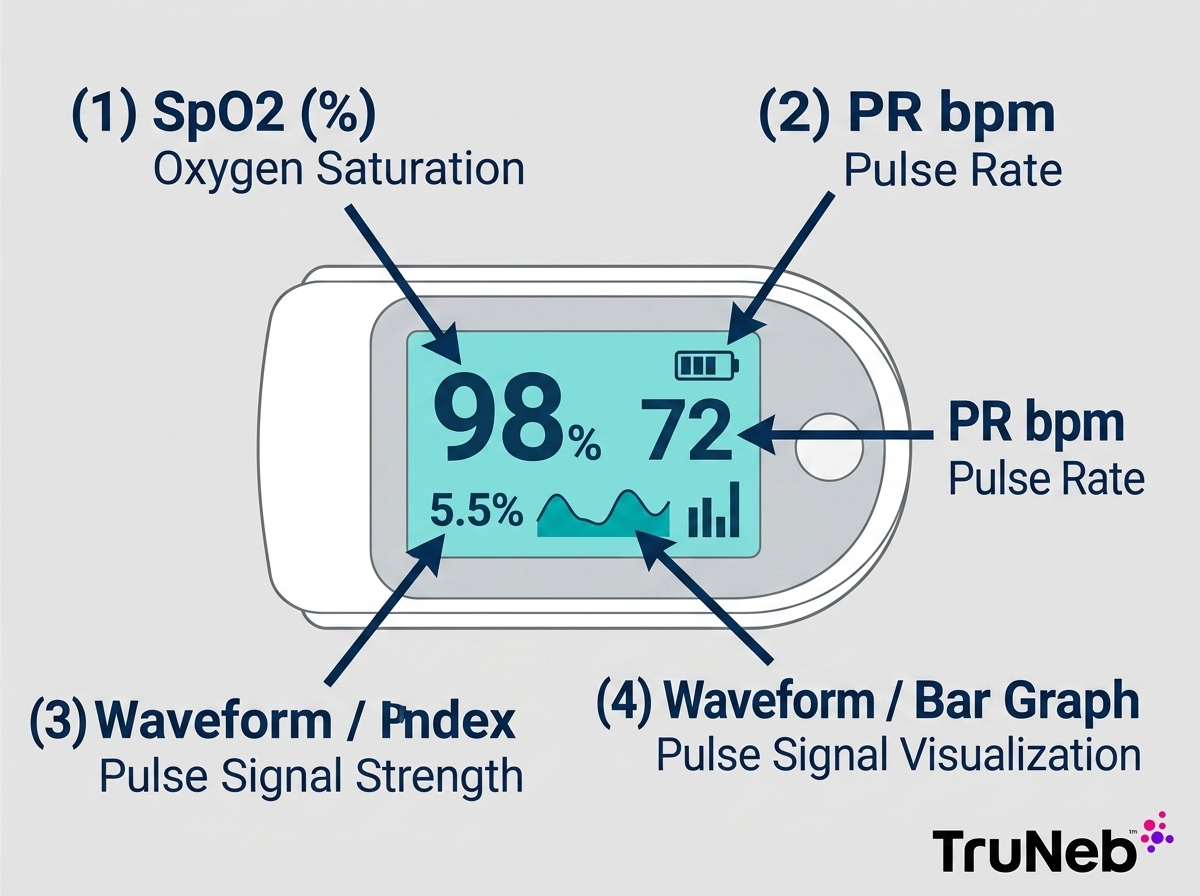
The two main readings on a pulse oximeter are SpO2 and PR bpm. SpO2 is the estimated oxygen saturation of hemoglobin (how full the oxygen seats are), shown as a percentage. PR bpm is your pulse rate, shown as beats per minute. Some models also show extras like a waveform (sometimes called a pleth), a bar graph, a battery or Bluetooth icon, or a perfusion index (PI), but SpO2 and PR bpm are the core numbers you read first.
Pulse oximeters estimate oxygen saturation and do not directly measure oxygen in your blood. They are less direct than an arterial blood gas (ABG) test. For a quick reference, see a pulse oximeter readings chart to understand common ranges at a glance.
SpO2 Shows Blood Oxygen Saturation
SpO2 estimates the percentage of hemoglobin carrying oxygen. It’s displayed as a percentage, usually the larger number on screen.
PR bpm Shows Pulse Rate
PR bpm is your pulse rate. It’s based on blood flow changes detected by the device and usually tracks your heart rate.
Some Devices Show Extra Numbers
If you see PI, that’s a signal-strength clue (how strong the pulse signal looks to the device). Waveforms and bar graphs also show signal quality. These help you get a steadier reading but are not the main results.
Quick takeaway: The two pulse oximeter readings are SpO2 (estimated oxygen saturation) and PR bpm (pulse rate).
What SpO2 and PR bpm Mean
SpO2 Shows How Much Oxygen Your Blood Is Carrying
SpO2 stands for peripheral oxygen saturation. It estimates what percent of your hemoglobin has oxygen on it. You’ll see it as a percentage labeled SpO2. For most healthy adults, typical values are about 95% to 100%. Targets can differ if you have lung or heart disease or live at higher altitude. Low SpO2 can point to hypoxemia, or low blood oxygen.
PR bpm Shows How Fast Your Heart Is Beating
PR means pulse rate, and bpm means beats per minute. This number estimates how many times your pulse beats each minute, based on blood flow changes in your finger. A common adult resting range is about 60 to 100 bpm. Fitness level, medicines, fever, stress, dehydration, and illness can shift this up or down. It usually tracks heart rate, but they are not exactly the same measurement.
Why You Should Read the Two Numbers Together
Reading SpO2 and PR bpm together gives a clearer picture. A low SpO2 with a high PR can mean your body is working harder. A normal SpO2 with a high PR can happen with anxiety, fever, pain, or recent activity. A low SpO2 with a normal PR can still be concerning. The device helps you track trends, but it does not diagnose problems by itself. SpO2 is not the same thing as your pulse or heart rate.
Quick takeaway: SpO2 estimates how full the oxygen seats are on hemoglobin; PR bpm tells you how fast the pulse is beating.
How to Read a Pulse Oximeter Screen
Find the Number Marked SpO2
This is your oxygen saturation. It’s shown as a percent (%). On many devices it’s the biggest number, but screen layouts can rotate or swap positions by brand, so read the labels.
Find the Number Marked PR bpm or HR
This is your pulse rate in beats per minute. It may sit near a heart icon or be labeled PR, PR bpm, or HR. This is not the oxygen number.
Understand Extra Labels Like PI, RR, and Waveform
PI often means perfusion index, a clue about signal strength at your finger. Some devices show RR for respiratory rate. A waveform (sometimes called a pleth) or bar graph shows that the device is detecting your pulse and how steady the signal is. Battery and Bluetooth symbols are device status, not health readings.
Not every number or icon on the screen is a health reading. Battery icons, Bluetooth symbols, and signal graphics are device info, not oxygen results.
Quick takeaway: Look for SpO2 for oxygen percent and PR bpm for pulse rate; everything else is extra context or device status.
Normal Pulse Oximeter Range in Adults
Typical SpO2 Range
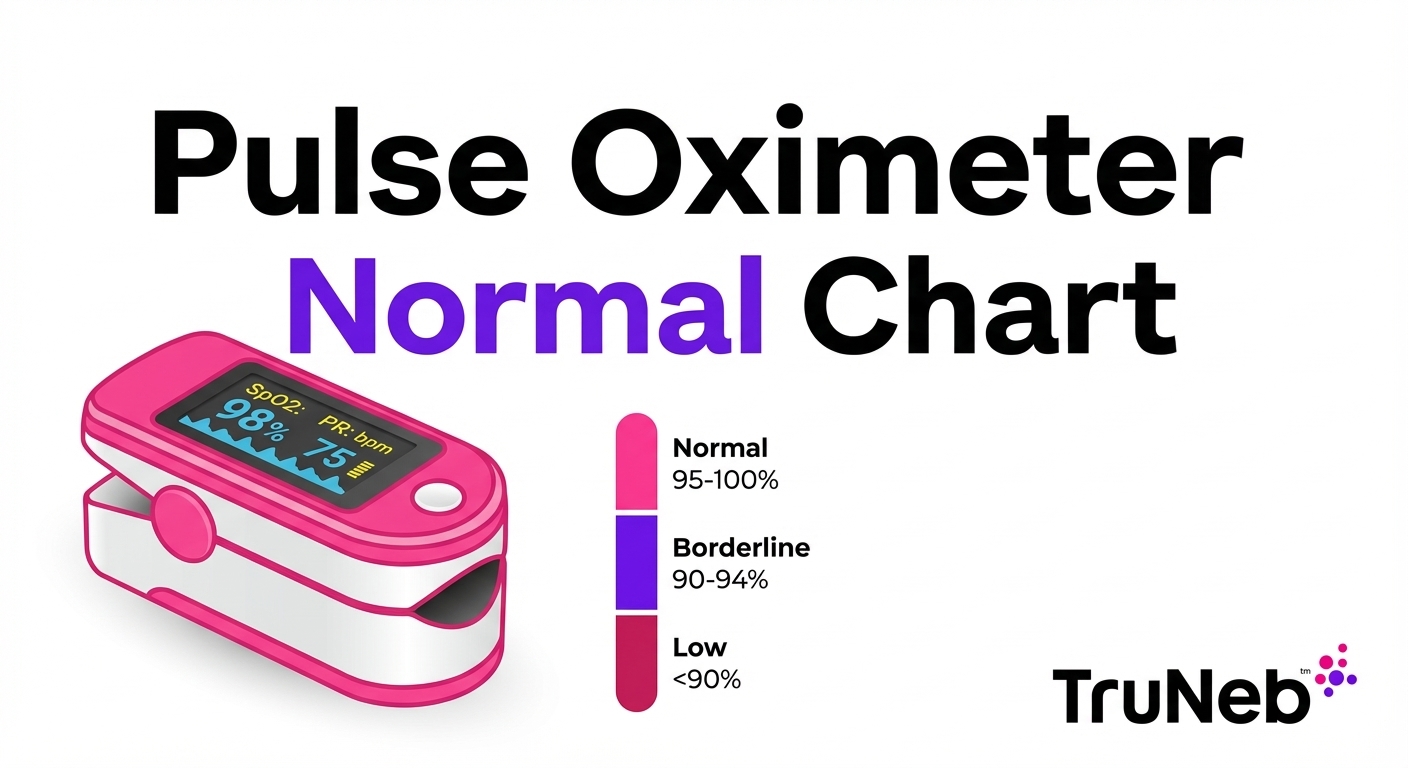
For most healthy adults at sea level, SpO2 is usually 95% to 100%. Values under 90% are generally considered low. Some people with chronic lung or heart conditions or those at higher altitude may have different targets set by their doctor. Home pulse oximeters are estimates, so numbers near a cutoff should be interpreted carefully. For a fuller view, see a normal oxygen levels during sleep guide.
Typical Resting Pulse Rate
A common adult resting pulse rate is about 60 to 100 bpm. Athletes can be lower. Fever, anxiety, pain, dehydration, infection, and some medicines can raise it.
When a Low Reading Becomes Concerning
Tap to view a simple adult SpO2 guide
| SpO2 (at sea level) | What it usually means | What to do |
|---|---|---|
| 95%–100% | Typical for most healthy adults | Log it if you’re monitoring |
| 93%–94% | Borderline for many people | Repeat with good technique; if it persists or is below your baseline, call your doctor |
| 90%–92% | Low for many adults | Call your doctor, especially if you have symptoms |
| ≤89% | Low | Seek medical advice promptly |
| ≤88% | Very low | Urgent evaluation is recommended |
Notes: Targets can differ for COPD, other chronic lung diseases, or higher altitude. Use trends and symptoms, not a single number.
Quick takeaway: For most healthy adults, SpO2 is usually 95% to 100% and resting pulse is 60 to 100 bpm, but your doctor may give you different targets.
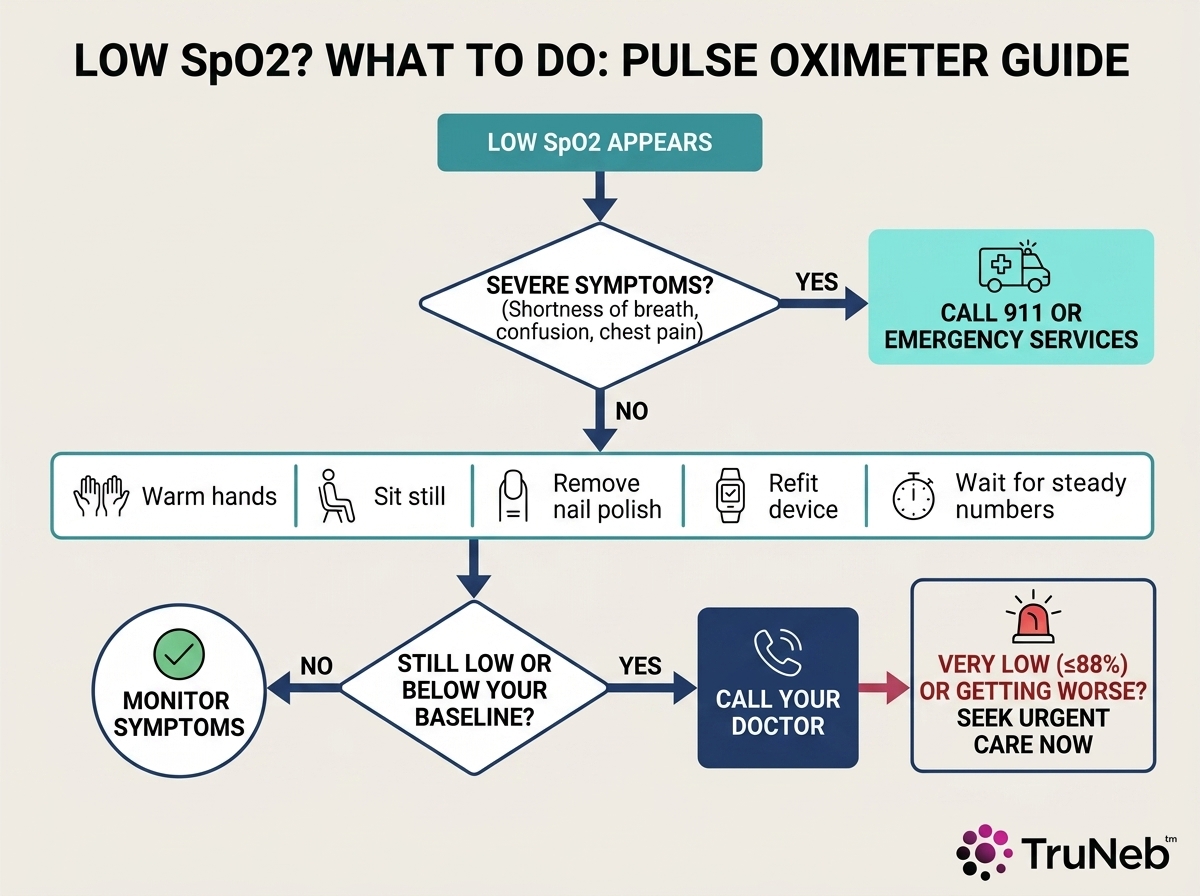
When Low Oxygen May Be an Emergency
⚠️ If you have severe shortness of breath, chest pain, confusion, blue lips or nails, fainting, or rapidly worsening symptoms, call 911 or seek emergency care right away.
Symptoms That Need Urgent Help
- Severe or sudden shortness of breath
- Chest pain or tightness
- Blue or gray lips, face, or nails (cyanosis)
- Confusion or trouble thinking clearly
- Fainting, collapse, or inability to speak full sentences
- Quickly worsening breathing or severe weakness
What to Do With a Very Low Reading
A normal-looking pulse ox does not rule out an emergency. If you feel very unwell, act on symptoms. If you can do so safely, repeat the reading after warming hands, sitting still, and refitting the device. Repeated SpO2 of 88% or lower deserves urgent medical attention.
Why Symptoms Matter More Than One Number
Pulse oximeters can be off by several points, and readings tend to be less reliable at lower oxygen levels. Do not wait on the device if symptoms are serious—seek help.
Quick takeaway: Severe shortness of breath, chest pain, confusion, blue lips, or very low repeated readings need urgent medical attention.
How to Get a More Accurate Reading at Home
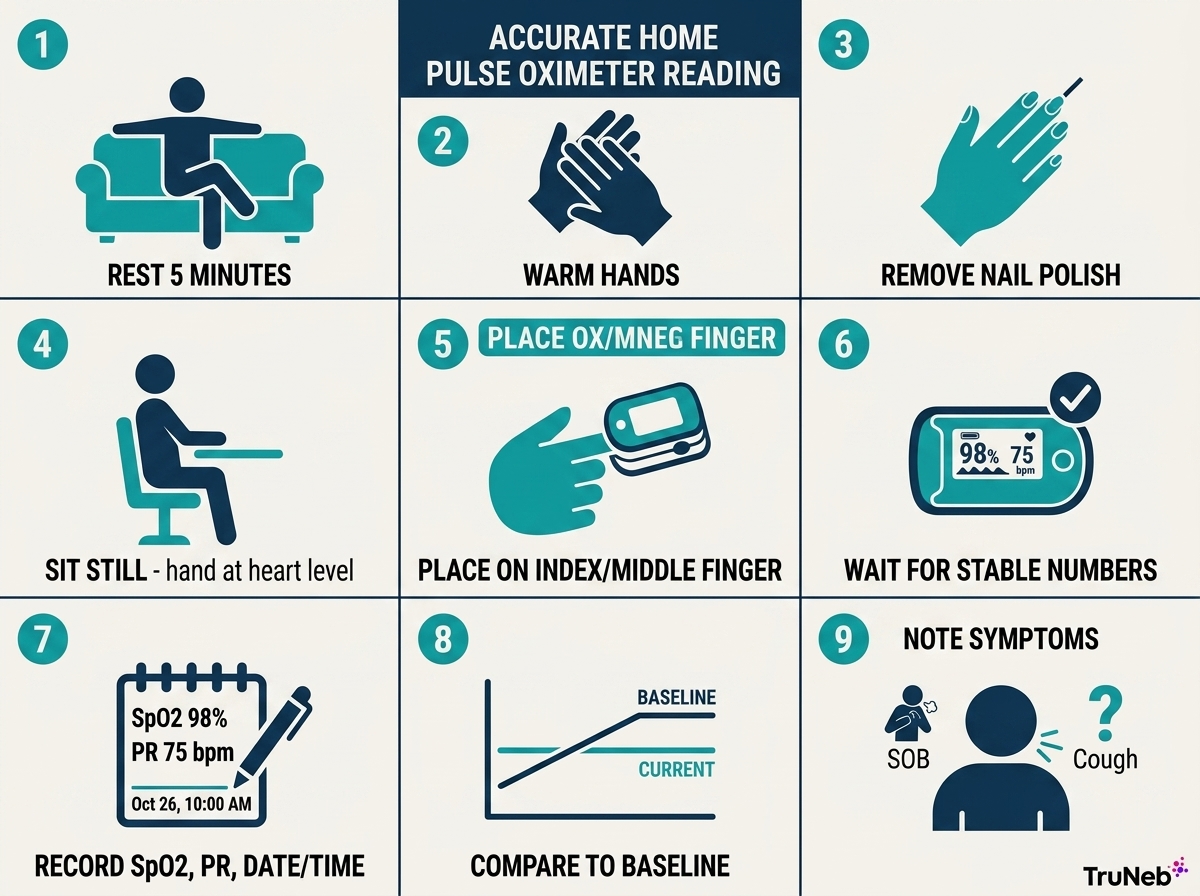
Step by Step Setup
- Read your device instructions.
- Rest for a few minutes before checking.
- Warm your hand (rub hands together or use warm water and dry well).
- Remove nail polish or artificial nails on the testing finger.
- Sit still with your hand relaxed at heart level.
- Place the oximeter snugly on the finger.
- Wait until the numbers stop changing and look steady.
- Record SpO2, PR bpm, symptoms, date, and time if you’re monitoring.
- Compare with your usual baseline and your doctor’s target.
Best Finger Placement for an Oximeter
The index or middle finger is commonly used. Use the same finger each time when tracking trends. The dominant-hand middle finger may read slightly higher in some people, but consistency matters more. Avoid very cold fingers or any with polish.
What Can Make a Reading Less Accurate
- Your body or environment: movement, cold hands, poor circulation, bright light, darker skin pigmentation effects, thicker skin, tobacco use, carbon monoxide exposure, fever, or anxiety.
- Device or setup: low battery, poor device fit, using an over-the-counter (OTC) general wellness device to make medical decisions, or reading before the display stabilizes.
FDA-cleared prescription or medical-purpose pulse oximeters undergo testing for accuracy claims, while many inexpensive OTC models are marketed as general wellness devices. Consumer fingertip devices provide estimates and should not be the only basis for medical decisions. Readings can be off by several points and are less reliable at lower oxygen levels.
Quick takeaway: Warm hands, stillness, good finger placement, and a stable display help you get the most reliable home estimate.
Why Pulse Oximeter Numbers Fluctuate
Small Changes Can Be Normal
A one to two point wiggle can happen with normal breathing, posture, activity, sleep, anxiety, altitude, or circulation shifts. The trend over time matters more than a single blink.
Big Jumps Usually Mean Signal Problems
If your reading jumps from very low to normal in seconds, think technique: movement, cold fingers, loose fit, low battery, bright light, or weak perfusion. If you do not have severe symptoms, fix these issues and retake the reading.
Repeated Low Readings Need Attention
If values stay low after careful setup and are below your usual baseline or doctor target, call your doctor. If your symptoms are severe, seek urgent help.
Troubleshooting quick list:
- Jumps every second → movement or weak signal; sit still until the display steadies
- Low with cold hands → warm hands, switch fingers, and retry
- No reading or dashes → refit the device, check battery, and try another finger
- Repeated low after proper technique → call your doctor; if you feel worse, seek urgent care
Quick takeaway: Rapid swings usually point to a weak signal; repeated lows after good technique deserve a call to your doctor.
What Perfusion Index Means on a Pulse Oximeter
PI Is a Signal Strength Clue
Perfusion index (PI) reflects how strong the pulse signal is at the sensor site. It compares pulsatile blood flow to non-pulsatile flow at your fingertip. In plain language, PI tells you how strong the pulse signal looks at your fingertip. A stronger signal usually helps the device hold a steadier reading.
How PI Helps Troubleshoot Readings
Low PI can show up with cold hands, poor circulation, or a loose device. If PI looks low and your numbers jump around, warm your hand, switch fingers, or reposition the oximeter until the signal steadies.
PI Is Not a Diagnosis
PI varies by person, device, finger, temperature, and health status. There isn’t a single “normal” PI number for everyone or every device. Use it to improve technique, not to diagnose a condition.
Quick takeaway: Perfusion index is best used as a signal-strength hint to steady your reading, not as a health score.
Special Notes for Asthma, COPD, and Chronic Lung Conditions
Know Your Personal Baseline
If you live with asthma, COPD, bronchiectasis, cystic fibrosis, heart failure, sleep apnea, or pulmonary hypertension, ask your doctor for your target ranges and when to call, adjust therapy, or seek urgent care. Track your usual numbers so you can spot changes.
Follow Your Respiratory Action Plan
Use your prescribed inhalers, nebulizers, oxygen, and airway clearance exactly as directed. Some people are prescribed nebulized medications or saline, including hypertonic saline, as part of a doctor-directed plan. Keep a simple log of SpO2, PR bpm, symptoms, and treatments if your doctor asks you to monitor. Do not change your medicines or oxygen on your own based on a single reading.
Where TruNeb Fits in Home Respiratory Care
For people prescribed nebulized therapy, a TruNeb portable mesh nebulizer can help deliver doctor-ordered medications or saline at home or on the go. It supports your broader care plan but does not replace a pulse oximeter, oxygen therapy, medical evaluation, or emergency care for low oxygen. TruNeb™ is not a treatment for low oxygen itself.
Quick takeaway: If you have a chronic lung condition, follow your doctor’s target range and action plan instead of a generic chart.
Pulse Oximeter Reading Examples
Example 1: SpO2 98 and PR bpm 72
This looks like a common adult resting reading. If you’re monitoring at home, record it as your baseline or daily check.
Example 2: SpO2 93 and PR bpm 105
Borderline oxygen with a fast pulse can be concerning if it keeps happening or is below your baseline. Repeat with careful technique and call your doctor if it persists or you have symptoms.
Example 3: SpO2 Jumps From 86 to 99
Big swings usually point to a weak signal from movement, cold fingers, or poor fit. If you do not have severe symptoms, fix technique and retest. If you feel very unwell, seek urgent care now.
Example 4: SpO2 88 or Lower
This may be urgent. Repeat only if it’s safe and you have no severe symptoms. If still 88 or lower, get medical help right away.
Quick takeaway: Treat steadiness and symptoms as your guide—recheck calmly, then escalate care if lows persist or you feel worse.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice. Always talk to your doctor about symptoms, oxygen readings, medications, and treatment decisions. If you think you’re having a medical emergency, call 911 right away.
Frequently Asked Questions
Tap or click a question below to see the answer:
SpO2 is your estimated oxygen saturation (%), and PR bpm is your pulse rate (beats per minute).
The oxygen number is labeled SpO2 and shown as a percentage.
SpO2 estimates oxygen on hemoglobin; PR bpm is your pulse rate. They are different numbers and mean different things.
Most healthy adults at sea level read about 95%–100% SpO2. Resting pulse is commonly 60–100 bpm. Your doctor may set different targets.
Severe shortness of breath, chest pain, confusion, blue lips or nails, fainting, or very low repeated readings (about 88% or lower) need urgent care—call 911.
Movement, cold hands, loose fit, bright light, low battery, or normal breathing changes can make numbers move. Let the display stabilize, then read.
The index or middle finger works well. Use the same warm, unpolished finger for tracking.
PI is a signal-strength hint showing pulse strength at the sensor site. It helps steady your reading but is not a diagnosis.
They provide estimates. Accuracy varies by device and can be off by several points, especially at lower oxygen levels. Many OTC models are general wellness devices; FDA-cleared medical devices have tested accuracy claims.
Some screens include PI (perfusion index) or RR (respiratory rate). Read the labels—SpO2 is oxygen %, PR bpm is pulse rate. Displays can rotate or swap positions by brand.
Use a nebulizer only as prescribed. It does not treat low oxygen itself or replace emergency care. A TruNeb™ portable mesh nebulizer helps deliver medicines within a doctor-directed plan.