On this page
What Atelectasis Means
Atelectasis is partial lung collapse at the air sac level.
Atelectasis means part of the lung hasn’t fully expanded because the tiny air sacs (alveoli) lost air, couldn’t refill, or were compressed. It’s a radiology finding, not a final diagnosis—the key question is why the lung didn’t stay open. How serious it is depends on the size of the area, the cause, your symptoms, and whether it keeps coming back.
Atelectasis is different from a fully collapsed lung caused by air around the lung (pneumothorax). But air or fluid around the lung can press on it and lead to atelectasis.
Report decoder: you might see words like subsegmental, bibasilar, linear, plate-like/discoid, dependent, or atelectatic changes. These usually describe size or location more than severity.
Small areas might cause no symptoms. Larger areas can cause shortness of breath or low oxygen. Your doctor looks at the size and likely cause to guide next steps.
Takeaway: Atelectasis means part of the lung has not fully expanded because the tiny air sacs lost air, couldn’t refill, or were compressed.
The Main Causes of Atelectasis in the Lungs
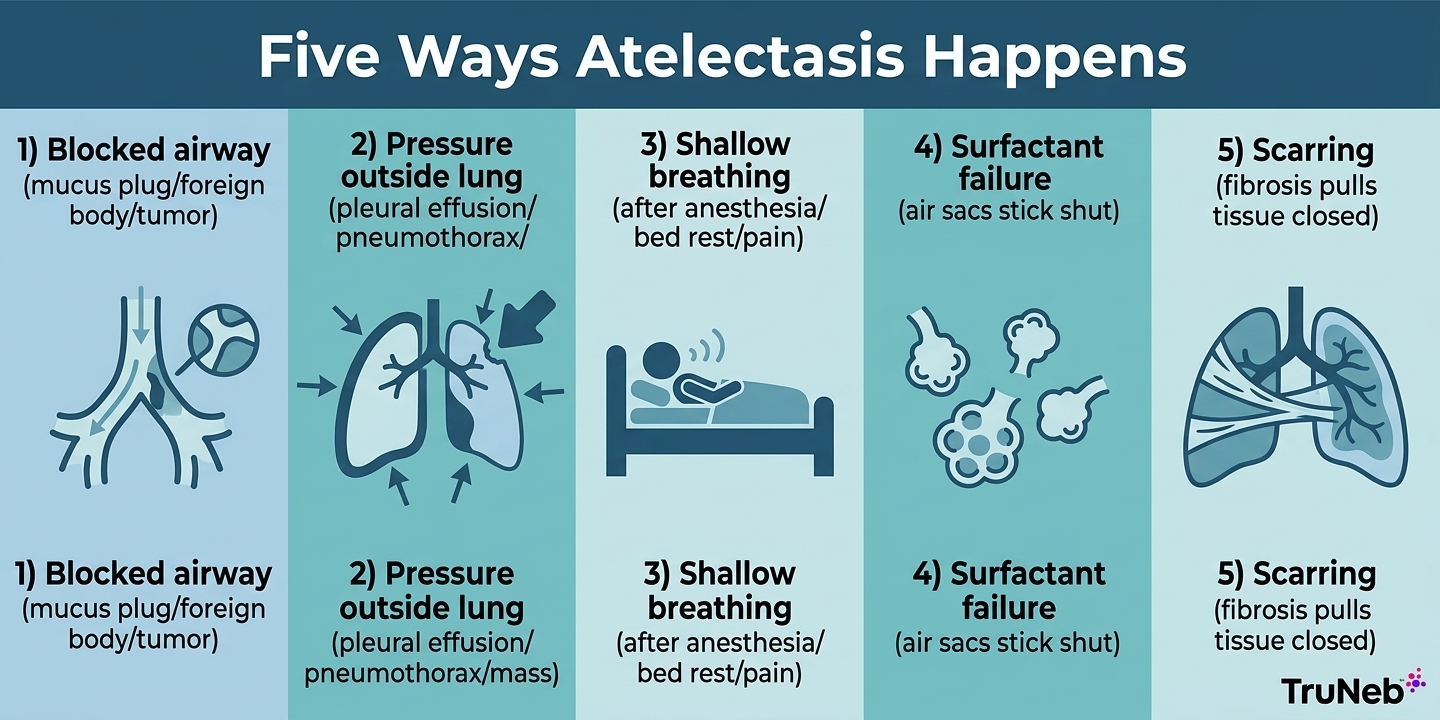
Most causes fall into five groups. In plain English, the lung can’t stay open because air can’t get in, the lung is being squeezed, or the air sacs won’t stay open.
Blocked airway (inside the tube)
A mucus plug, thick sputum/phlegm, food aspiration, a foreign body, or an endobronchial tumor (including lung cancer) can block airflow. Air beyond the blockage is absorbed into the blood and the air sacs collapse.
Pressure from outside the lung
Pleural effusion, pneumothorax, or a mass can compress the lung. Abdominal distension can also push the diaphragm upward and squeeze the lower lungs, leading to dependent or bibasilar atelectasis.
Low lung expansion (shallow breathing)
After anesthesia, with pain, or during bed rest, breaths are shallow. The lower lungs don’t fill well and small, plate-like (discoid) areas close down.
Surfactant problems
When surfactant is low or impaired, air sacs stick shut (for example in acute lung injury/ARDS).
Scarring/fibrosis
Fibrosis or old injury tugs airways and air sacs into a closed shape (cicatrization atelectasis).
Surgery with general anesthesia is a common setting for atelectasis in adults, especially in the first few days. People with asthma, COPD, bronchiectasis, or cystic fibrosis have a higher chance of mucus plugs.
Takeaway: The main causes of atelectasis are airway blockage, pressure from outside the lung, shallow breathing after surgery or pain, surfactant problems, and scarring.
Obstructive vs Nonobstructive Atelectasis
Obstructive (resorptive)
An airway blockage prevents fresh air from reaching the alveoli. Trapped air is absorbed, and the air sacs collapse. Triggers include a mucus plug, thick secretions, food aspiration, a foreign body, or an endobronchial tumor.
Nonobstructive
There’s no internal plug. The lung collapses from outside pressure, under-expansion, scarring, or surfactant problems (for example, pleural effusion, pneumothorax, fibrosis, or adhesive/surfactant issues).
| Type | What happens | Typical triggers | Common settings |
|---|---|---|---|
| Obstructive (resorptive) | Air can’t reach alveoli; trapped air is absorbed | Mucus plug, thick sputum/phlegm, food aspiration, foreign body, endobronchial tumor | Post-op, asthma/COPD/CF, children |
| Compressive (nonobstructive) | Lung is squeezed from outside | Pleural effusion, pneumothorax, mass, abdominal distension | Hospital, trauma, cancer |
| Adhesive (nonobstructive) | Air sacs won’t stay open | Surfactant impairment | ARDS, newborns |
| Cicatrization (nonobstructive) | Scar tissue pulls lung closed | Fibrosis, prior TB, radiation | Chronic lung disease |
| Postoperative mixed | Shallow breaths plus secretions | Anesthesia, pain, immobility | First few days after surgery |
Examples only. Your doctor will match imaging findings with your symptoms and history.
Takeaway: Obstructive atelectasis comes from an airway blockage, while nonobstructive atelectasis happens from pressure, under-expansion, scarring, or surfactant problems.
Atelectasis Causes and Risk Factors by Setting
Hospital and surgery
General anesthesia reduces deep breaths and cough. Muscle relaxants, a breathing tube, opioids, pain, lying flat, and immobility all raise risk. Chest, abdominal, and heart surgeries carry higher risk, and atelectasis tends to show up in the first few days after an operation.
Chronic lung disease
Asthma, COPD, bronchiectasis, and cystic fibrosis are linked to thick mucus and mucus plugs. Pneumonia or acute lung injury (ARDS) can also trigger small areas of collapse.
Lifestyle and physical factors
Smoking, obesity, pregnancy, rib fractures, chest trauma, neuromuscular weakness (for example muscular dystrophy), spinal cord injury, poor cough strength, swallowing problems with aspiration, and abdominal distension can contribute. These factors guide prevention and follow-up, but don’t always mean the finding is serious.
Takeaway: Risk factors help explain why atelectasis happened, but they don’t always mean the finding is serious.
Mucus Plug Atelectasis
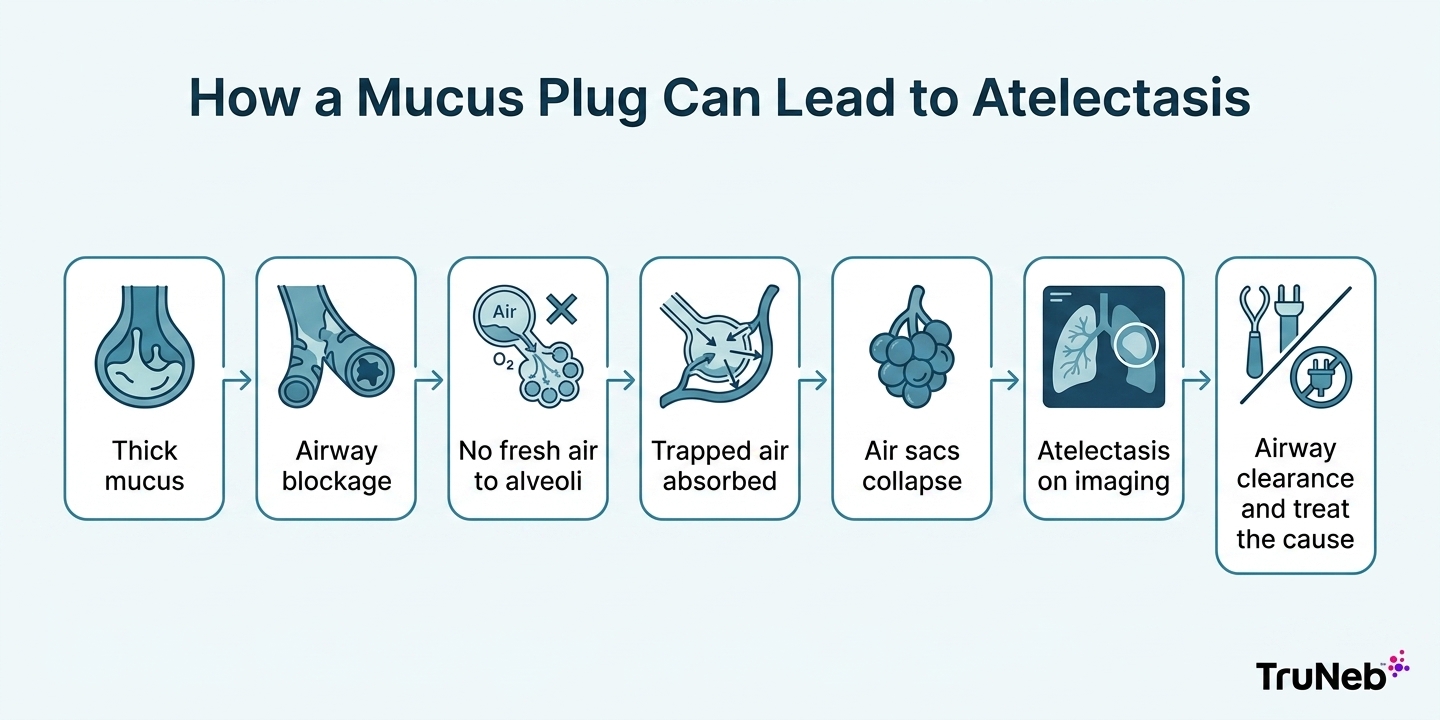
Mechanism
A mucus plug can block an airway; the air beyond it is absorbed and the air sacs deflate, so the closed area shows up on imaging. People often call these secretions mucus, sputum, or phlegm.
Who is at higher risk
After surgery; during severe asthma flares; with cystic fibrosis or bronchiectasis; in COPD with thick secretions; in children; with dehydration or dry air; on a ventilator; and when cough strength is low.
How doctors manage it
Deep breathing and coughing, incentive spirometry, chest physiotherapy, good hydration when allowed, suctioning when needed, and bronchodilators if prescribed. Selected patients use mucus-thinning therapies, such as prescribed hypertonic saline nebulizers, when a doctor recommends them. If obstruction doesn’t clear, bronchoscopy can remove a plug or foreign body and check for other causes.
When a doctor prescribes nebulized medication or hypertonic saline to thin and move mucus, TruNeb portable mesh nebulizer can help you complete scheduled treatments at home or during recovery. Nebulized therapy doesn’t replace deep breathing, coughing, positioning, movement, or follow-up care.
Takeaway: Mucus plug atelectasis happens when thick mucus blocks an airway and air sacs beyond the blockage deflate.
Postoperative Atelectasis Prevention
Why it happens after surgery
Anesthesia lowers deep breaths and cough. Pain leads to splinting and shallow breathing. Lying down reduces lung expansion. Secretions can pool, so early steps matter, especially in the first few days after surgery.
Prevention checklist
Patients are usually advised to sit upright, reposition regularly, and get moving as soon as the team clears it. Your team might ask you to use an incentive spirometer correctly as directed, then cough to clear loosened mucus. Some people are shown how to splint the incision with a pillow when coughing. Use prescribed inhalers or nebulized treatments when ordered.
When nebulized therapy is added
Doctors add nebulized therapies for thick secretions, chronic mucus conditions, or trouble clearing mucus. If prescribed, a portable mesh device can make it easier to stay on schedule.
Takeaway: After surgery, deep breathing, coughing, movement, positioning, and pain control help keep the lungs open.
Incentive Spirometer and Breathing Exercises for Atelectasis
Incentive spirometer
An incentive spirometer coaches slow, deep breaths that can reopen air sacs and reduce shallow-breathing collapse. Your doctor or therapist will tell you how often to use it.
Deep breathing and coughing
As an example of how therapists sometimes teach it: take a slow breath in through your nose so your belly rises, pause briefly if instructed, then breathe out slowly and cough to clear loosened mucus. Stop and rest if you feel dizzy or unwell, and tell your doctor if symptoms persist.
Pursed-lip and diaphragmatic (belly) breathing
Pursed-lip breathing slows the breath out and helps keep airways open a bit longer. Diaphragmatic breathing trains your main breathing muscle to work better. These methods support many people with chronic lung disease and are adapted after surgery.
Takeaway: An incentive spirometer helps you take slow, deep breaths that can reopen air sacs and reduce shallow-breathing collapse.
Atelectasis vs Pneumonia on Chest X Ray
Why they can look similar
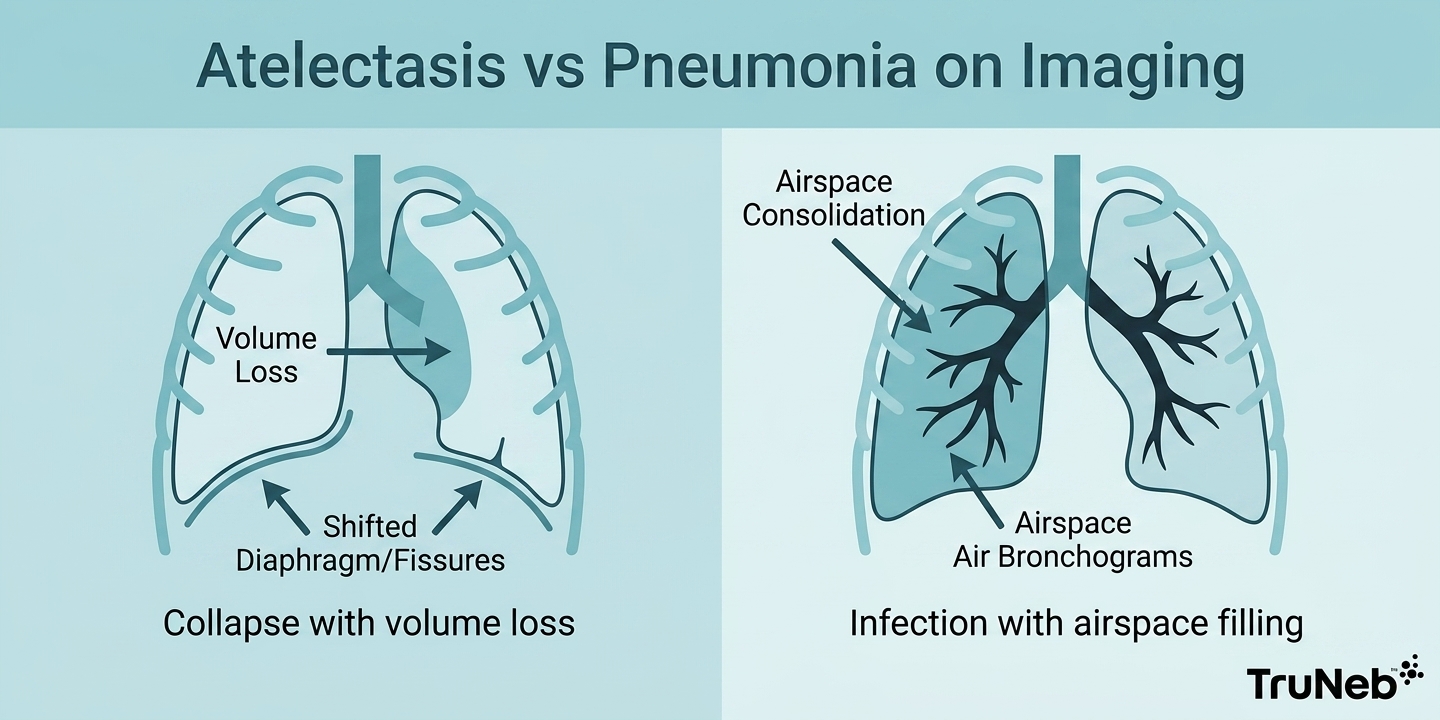
Both can show a white area (an opacity) on X-ray. Atelectasis is collapse with volume loss. Pneumonia is infection that fills air spaces with fluid or pus (consolidation). They can also occur together.
Clues favoring atelectasis
Signs of volume loss like shifted fissures, an elevated diaphragm, or structures pulled toward the white area; bandlike or wedge-shaped opacity; sometimes fewer clear air bronchograms; and in larger collapse, a mediastinal or hilar shift toward the affected side.
Clues favoring pneumonia
Consolidation without obvious volume loss; air bronchograms are common; fever, cough, and labs often support infection.
Takeaway: On imaging, atelectasis usually shows volume loss, while pneumonia usually shows infection-related airspace filling. For a broader comparison, see bronchitis vs pneumonia differences.
Is Subsegmental Atelectasis Serious
Mild cases
Subsegmental atelectasis is the mildest form and involves less than one bronchopulmonary segment. Reports might call it linear, plate‑like/discoid, bandlike, bibasilar, or dependent. It often shows up after shallow breathing, pain, immobility, or soon after surgery. Many small areas improve as you breathe deeper and move more.
When to pay more attention
See a doctor promptly if you have shortness of breath, low oxygen, chest pain, fever, or a cough that worsens, or if the finding keeps coming back. It also matters more with a smoking history, lung cancer risk, unexplained weight loss, coughing blood, or when a blockage is possible.
Takeaway: Subsegmental atelectasis is usually a small, mild finding, but symptoms or repeated findings need medical follow‑up.
How Atelectasis Is Diagnosed
Imaging
A chest X‑ray is usually first. A CT scan can show the type, size, and cause more clearly and can reveal a hidden blockage or fluid. Images are read together with your symptoms and history.
Oxygen checks and ultrasound
Pulse oximetry checks oxygen level on your finger. Arterial blood gas can be used when illness is more serious. Chest ultrasound can identify pleural effusion or pneumothorax.
Bronchoscopy
A thin camera test looks inside the airways when a blockage is suspected. It’s both diagnostic and therapeutic in some cases: it can remove a mucus plug or foreign body and take samples if a tumor (including an endobronchial tumor) is possible.
Takeaway: Doctors diagnose atelectasis by matching imaging findings with symptoms, oxygen levels, and the suspected cause.
How Atelectasis Is Treated
Treat the cause
Mild cases can improve as you breathe deeper, move more, and clear mucus. Larger, persistent, or symptomatic areas need a plan from your doctor. Treating the underlying cause—such as pneumonia, pleural effusion, or a tumor—helps prevent recurrence.
Airway clearance and support
Deep breathing, incentive spirometry, coughing, chest physiotherapy, postural drainage, and gentle percussion can help. Early activity and upright positioning support lung inflation. Some people need supportive care such as supplemental oxygen, assisted cough techniques for weak cough, or noninvasive positive pressure (for example, CPAP in selected patients as advised by a doctor).
Removing a blockage
Suctioning can remove secretions. Bronchoscopy can remove a mucus plug or foreign body and evaluate or sample a suspected tumor when needed.
Medications and nebulized treatments
Bronchodilators can help when airway narrowing plays a role. Selected patients use mucus‑thinning therapies—including prescribed hypertonic saline—under doctor guidance. A portable mesh nebulizer can make prescribed treatments easier to complete on schedule. TruNeb™ is not a substitute for diagnosis or emergency care, but it can support a prescribed airway‑clearance plan when a doctor recommends nebulized medication or hypertonic saline for thick mucus.
Safety: Talk to your doctor before starting any new medication or device. Don’t start, stop, or change prescriptions on your own.
Takeaway: Treatment for atelectasis focuses on reopening the lung and fixing the reason it collapsed.
When to Call a Healthcare Provider
⚠️ Seek emergency care right away for severe or sudden shortness of breath, blue lips or face, chest pain, confusion, or coughing blood.
Urgent help
Go to urgent or emergency care for rapidly worsening breathing, very low oxygen readings if you monitor, severe wheezing, chest pain, confusion, blue lips or face, or coughing blood.
Follow‑up concerns
Call your doctor for fever, a persistent or worsening cough, thick mucus you can’t clear, new or recurrent atelectasis on imaging, known lung disease with new symptoms, or questions about prescribed inhaled or nebulized therapy.
Takeaway: Sudden breathing trouble, blue lips, chest pain, confusion, or coughing blood need urgent medical care.
Disclaimer: This article is for informational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Always talk to your doctor about your symptoms, test results, and treatment options.
Key Terms to Know
These common report terms can help you understand what your imaging results are describing.
Atelectasis: partial collapse of lung tissue when air sacs don’t stay open.
Atelectatic changes: wording radiology reports use for areas that look partially collapsed.
Alveoli: tiny air sacs where oxygen enters your blood.
Obstructive (resorptive) atelectasis: collapse caused by an airway blockage; trapped air is absorbed.
Nonobstructive atelectasis: collapse from pressure, under‑expansion, scarring, or surfactant issues.
Compressive atelectasis: outside pressure squeezes the lung (for example, pleural effusion or pneumothorax).
Adhesive atelectasis: low or impaired surfactant lets air sacs stick shut.
Cicatrization atelectasis: scar tissue pulls lung closed.
Subsegmental atelectasis: the mildest, very small area of collapse.
Linear, plate‑like, or discoid atelectasis: thin bandlike areas, often from shallow breathing.
Bibasilar atelectasis: small areas at both lung bases.
Dependent atelectasis: small areas in the lowest parts of the lungs when lying down.
Pleural effusion: fluid around the lung that can compress it. See also pleural effusion vs pneumothorax.
Pneumothorax: air around the lung that can compress it.
Opacity: a white area on an X‑ray that can represent collapse or other processes.
Consolidation: infection‑related airspace filling often seen in pneumonia.
Bronchoscopy: a camera test to look inside and sometimes treat the airways.
Endobronchial tumor: a growth inside an airway that can narrow or block it.
Aspiration: when food, liquid, or stomach contents go into the airway or lungs instead of the stomach.
Incentive spirometer: a device to coach slow, deep breaths.
Hypertonic saline: sterile salty solution sometimes prescribed to thin mucus. Some patients may use 3% hypertonic saline solution when prescribed.
Frequently Asked Questions
Tap or click a question below to see the answer:
In adults, the most common setting is the first few days after surgery with general anesthesia. Mucus plugs and shallow breathing are typical drivers.
It’s usually small and mild. Get medical care if you have symptoms, low oxygen, or if the finding keeps coming back.
Atelectasis shows collapse with volume loss; pneumonia shows infection‑related airspace filling (consolidation). Doctors read images with your symptoms and labs.
Follow your surgical team’s plan: sit up, reposition, walk when cleared, use the incentive spirometer as instructed, cough, manage pain, and use prescribed inhalers or nebulized therapy.
It helps you take slow, deep breaths that can reopen air sacs. It’s one part of a bigger plan that also includes movement and coughing.
Yes. A mucus plug can block an airway so the air sacs beyond it deflate until the blockage clears.
Only when a doctor prescribes medication or saline to thin mucus or open airways. A nebulizer doesn’t replace breathing exercises or medical care.
Small areas can improve with deeper breathing, coughing, and movement. Bigger or persistent areas need medical evaluation.
Seek urgent care for sudden or severe breathing trouble, blue lips, chest pain, confusion, or coughing blood. Call your doctor for fever, a worsening cough, thick mucus you can’t clear, or repeated findings on imaging.
Atelectasis is partial collapse at the air‑sac level. A full collapse from air around the lung is pneumothorax; it can also compress the lung and cause atelectasis.