On this page
Why Stairs and Hills Make You Short of Breath So Quickly
Stairs are a hidden stress test
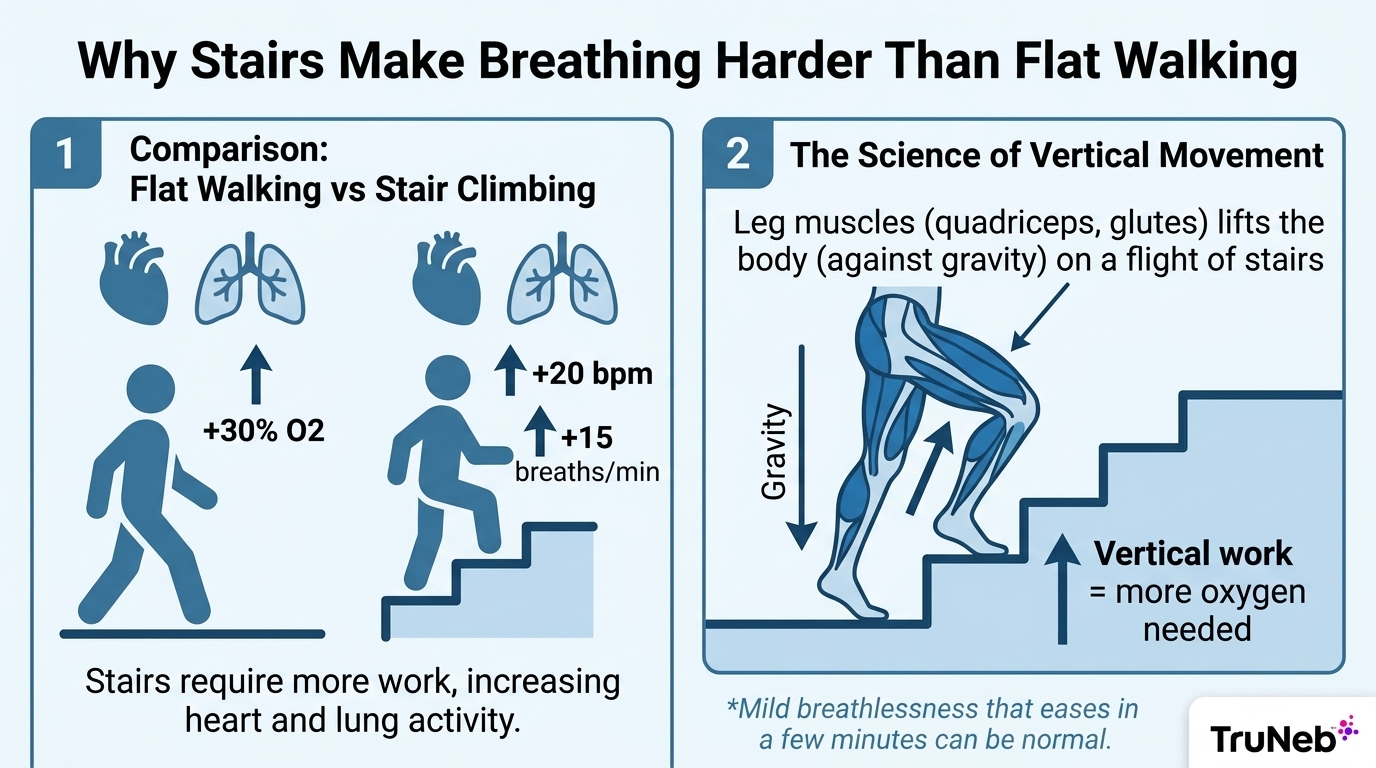
Shortness of breath climbing stairs is common because stairs act like a mini stress test. You move your body weight up against gravity. Your leg muscles ask for oxygen fast. Your heart rate and breathing rate jump within seconds. That sudden spike can leave you winded even if flat walking feels easy.
Hills and extra load
Climbing pulls in more muscle fibers in your quads and calves than strolling on level ground. Those muscles need oxygen-rich blood right away. Your lungs move more air to bring in oxygen and clear carbon dioxide. Your heart pumps harder to deliver it. If you start from sitting or standing still, the jump in demand feels sharper. Hills work the same way. Walking uphill or on an incline raises the mechanical load on your legs. The steeper the grade, the higher the oxygen demand. Cold air, air pollution, extreme heat or cold, heavy bags, or rushing can add even more effort to the task.
What feels normal
Mild breathlessness that settles within a few minutes of rest can be normal. It is also common to feel more winded after sickness, time off from exercise, travel, or at higher altitude. As your conditioning improves, stairs usually feel easier. Breathlessness is a symptom, not a diagnosis. The cause ranges from fitness and recovery to heart or lung conditions.
Takeaway: Stairs raise oxygen demand fast, so brief breathlessness that eases with rest can be normal; a new or worsening pattern deserves a closer look.
Medical disclaimer: This article is for general information only and is not a substitute for medical advice. Talk to your doctor about your symptoms and seek urgent care for red-flag signs.
When Shortness of Breath on Stairs Is Normal and When It Is Not
Normal patterns
Breathlessness shows up with clear effort (climbing, rushing, carrying bags), eases within a few minutes, and stays stable week to week. You can keep going after a short pause. There is no chest pain, fainting, blue lips, or severe wheezing. This usually reflects fitness level, quick starts from rest, or recovery after illness or travel.
Concerning patterns
Breathlessness is new, getting worse, or appears after just one flight. You now need to stop during simple tasks that used to be easy. You get short of breath with mild activity, while talking, or even at rest. Recovery takes longer. You also have chest pressure, dizziness, palpitations, wheeze, swelling, fever, or cough. These changes should be checked by a doctor.
Track your threshold
Note how many stairs trigger symptoms, how long you need to recover, and what else you feel (like chest tightness or wheeze). A drop in your usual threshold over days or weeks is a clear sign to see your doctor. Exercise intolerance is the term for getting unusually winded or fatigued with activity.
Shortness of breath on stairs: what is usually normal vs more concerning
| Feature | Usually normal | More concerning |
|---|---|---|
| Trigger | Clear effort (climbing fast, carrying loads, rushing, cold air) | Shows up with milder activity, talking, or at rest |
| Recovery time | Settles within a few minutes of rest | Takes longer to recover or lingers |
| Other symptoms | No chest pain, fainting, blue lips, or severe wheeze | Chest pressure, fainting/near-fainting, blue lips, severe wheeze, coughing blood |
| Trend over time | Stable week to week or improving with training | New or worsening over days to weeks |
| Context | After illness, deconditioning, pregnancy, altitude, extreme temperatures, or air pollution exposure | Unexplained drop in activity tolerance (exercise intolerance) or new swelling, fever, palpitations |
| What to do | Slow down, pace, rebuild fitness if already cleared | See a doctor; call 911 for red‑flag symptoms |
Note: Severe symptoms or red flags require urgent care rather than self‑testing.
Takeaway: Shortness of breath on stairs is more concerning when your usual activity threshold drops or symptoms start happening with milder activity.
Red Flags That Need Urgent Medical Care
Call 911 now
- Sudden or severe shortness of breath
- Chest pain, pressure, tightness, or heaviness; pain spreading to the arm, jaw, neck, back, or upper belly
- Fainting, feeling like you might pass out, or new confusion
- Blue lips, face, or nails
- Severe dizziness or severe, irregular palpitations
- Coughing blood or pink, frothy mucus
- Sudden breathlessness after surgery, immobilization, or long-distance travel
- Severe wheezing or inability to speak in full sentences
Make a doctor's appointment soon
New or worsening breathlessness on stairs, wheeze, a persistent cough, fever or chills, swollen ankles or feet, trouble breathing when lying flat, or breathlessness that limits normal tasks, especially if you have known heart or lung disease.
Do not test yourself by pushing harder. If symptoms are severe or paired with red flags, stop the activity and seek care.
Takeaway: Sudden or severe shortness of breath, especially with chest pain, fainting, blue lips, or coughing blood, is a medical emergency.
Common Causes of Being Out of Breath Walking Up Stairs
Deconditioning and reduced aerobic fitness
If you have been less active, your heart, lungs, and muscles aren’t as efficient. Your muscles ask for more oxygen to do the same work, and you clear carbon dioxide less efficiently. That gap shows up fast on stairs and hills. The good news: gradual activity and strength work usually help.
Weight, recent illness, and recovery
Extra body weight means more vertical work per step. A recent cold, influenza, RSV, or COVID-19 can leave airways irritated and stamina lower for weeks. Bed rest, surgery, or travel can lower conditioning, too. As you rebuild routine, stairs tend to feel better.
Asthma and exercise-triggered airway narrowing
Wheezing, chest tightness, cough, and breathlessness that flare with cold air, allergens, smoke, air pollution, or exercise can point toward asthma or exercise-induced bronchoconstriction. Quick-relief medicine is part of a prescribed plan, but diagnosis and a tailored action plan come first.
COPD and other chronic lung disease
A long smoking history, chronic cough, mucus, wheeze, and a slow decline in activity tolerance can signal COPD. Other lung conditions like bronchiectasis, interstitial lung disease (including pulmonary fibrosis), or pulmonary hypertension can also make stairs feel harder.
Infections and inflammation
Recent respiratory infections (COVID-19, influenza, RSV) or flare-ups of chronic lung disease can temporarily raise breathing work.
Anemia and thyroid disease
If red blood cells or hemoglobin are low, your body carries less oxygen to working muscles. You might feel breathless, tired, lightheaded, or look pale with exertion. Thyroid problems can also affect heart rate, breathing, and stamina.
Anxiety and panic
Anxiety can speed breathing and make normal exertion feel alarming. Don’t assume anxiety is the only cause if stair breathlessness is new or worsening. Talk with your doctor about the full pattern.
Pregnancy
Shortness of breath can happen in pregnancy as blood volume, oxygen needs, and diaphragm position change. New, severe, or worrisome symptoms still warrant a check-in with your doctor.
Environment and weather
Air pollution and extreme heat or cold can worsen exertional breathlessness, especially with asthma or chronic lung disease.
Less common but serious
Conditions like pleural effusion or pneumothorax are less common but can cause significant breathlessness and need prompt medical care.
Heart and circulation causes (high-level)
Coronary artery disease, angina, heart failure, arrhythmias, cardiomyopathy, aortic stenosis, valve disease, and pulmonary hypertension can limit oxygen delivery or raise pressures in the lungs during exertion. These usually need specific testing and care. See the heart-versus-lung comparison below for patterns to share with your doctor.
Takeaway: Stair breathlessness can come from fitness changes, lung disease, heart disease, anemia, thyroid disease, anxiety, environment, pregnancy, or recovery after illness.
Heart vs Lung Causes of Exertional Dyspnea
Clues that point toward a heart cause
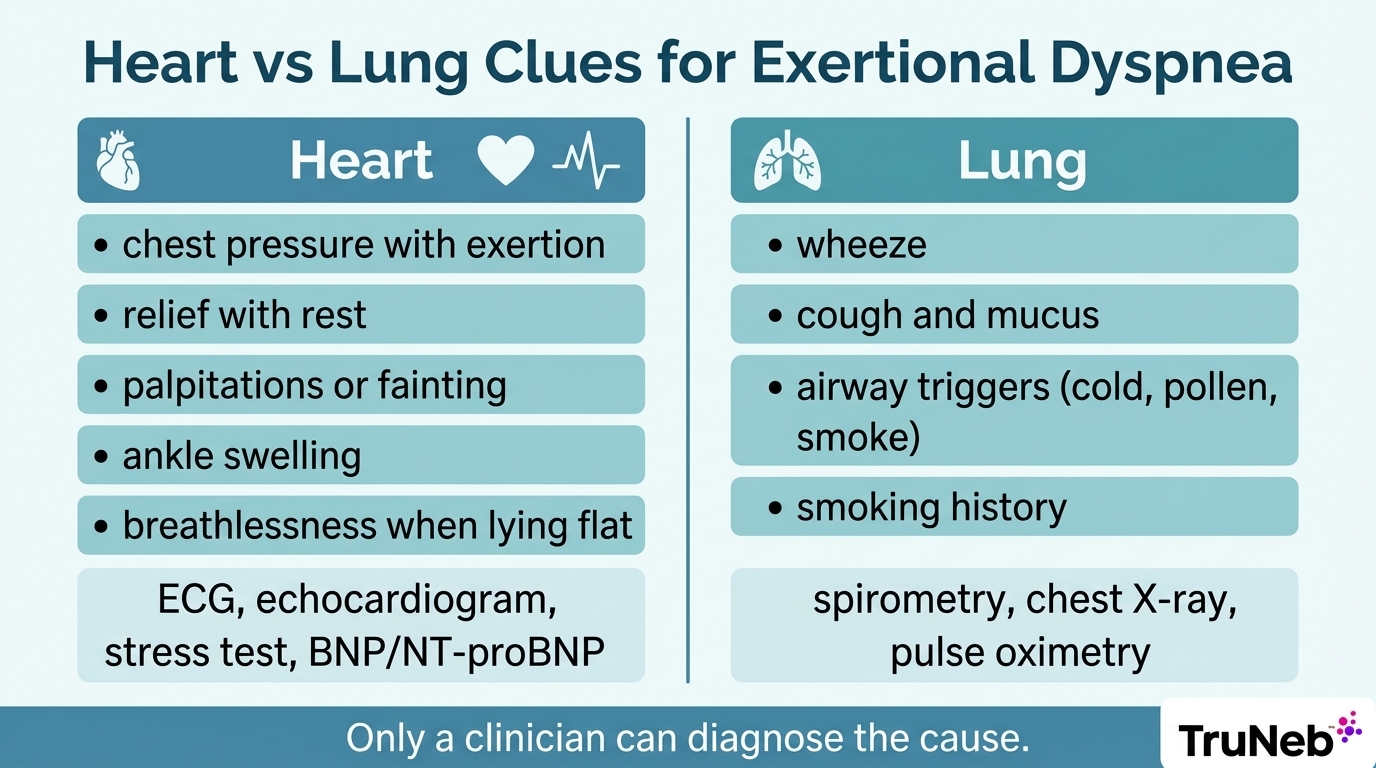
Chest pressure, heaviness, or tightness with exertion that eases with rest is a classic angina pattern. Palpitations, fainting or near-fainting, ankle swelling, and trouble breathing when lying flat can also point to heart causes, including heart failure, cardiomyopathy, or valve disease such as aortic stenosis. Risk factors like high blood pressure, diabetes, high cholesterol, smoking, family history, or known coronary artery disease raise concern.
Clues that point toward a lung cause
Wheezing, cough, and mucus suggest airway involvement. Chest tightness with airway symptoms, triggers like cold air, pollen, smoke, air pollution, infections, or exercise, a smoking history, or known asthma, COPD, bronchiectasis, interstitial lung disease, or pulmonary hypertension all lean lung.
Why overlap is common
Some people have both heart and lung contributors. Others have fitness plus a medical issue. Patterns guide testing, but only an exam and the right tests can confirm the cause. Avoid self-diagnosis.
Tests your doctor may use
Pulse oximetry can check oxygen saturation. A complete blood count can look for anemia. An ECG and a chest X-ray give fast heart and lung clues. Spirometry looks for airflow limits. An echocardiogram checks heart structure and valves. A stress test looks at exertion response. BNP or NT-proBNP can point toward heart failure. Troponin might be checked in urgent settings. If a pulmonary embolism is suspected, doctors can use a risk score with a D-dimer. When the cause is unclear, cardiopulmonary exercise testing can sort cardiac from pulmonary limits.
Key point: Heart-related dyspnea often pairs with chest pressure, swelling, palpitations, or relief with rest; lung-related dyspnea often pairs with wheeze, cough, mucus, and clear airway triggers.
Orthopnea vs Exertional Dyspnea
Exertional dyspnea
Exertional dyspnea happens during activity. It shows up on stairs, hills, walking, or exercise and improves with rest.
Orthopnea
Orthopnea happens when lying flat. It eases when you sit up or stand. It can be related to heart failure, COPD, obesity, pulmonary hypertension, or other conditions that change pressures or airflow when you recline. See also: TruNeb features overview.
Paroxysmal nocturnal dyspnea
This pattern wakes you from sleep short of breath. It often needs prompt evaluation.
If your pattern changes, from only with effort to also when lying down, or from rare to frequent, tell your doctor. The timing and triggers help guide testing and treatment.
Takeaway: Exertional dyspnea happens during activity, while orthopnea happens when lying flat.
Breathing Techniques for Climbing Stairs
Pursed-lip breathing (practice when calm)
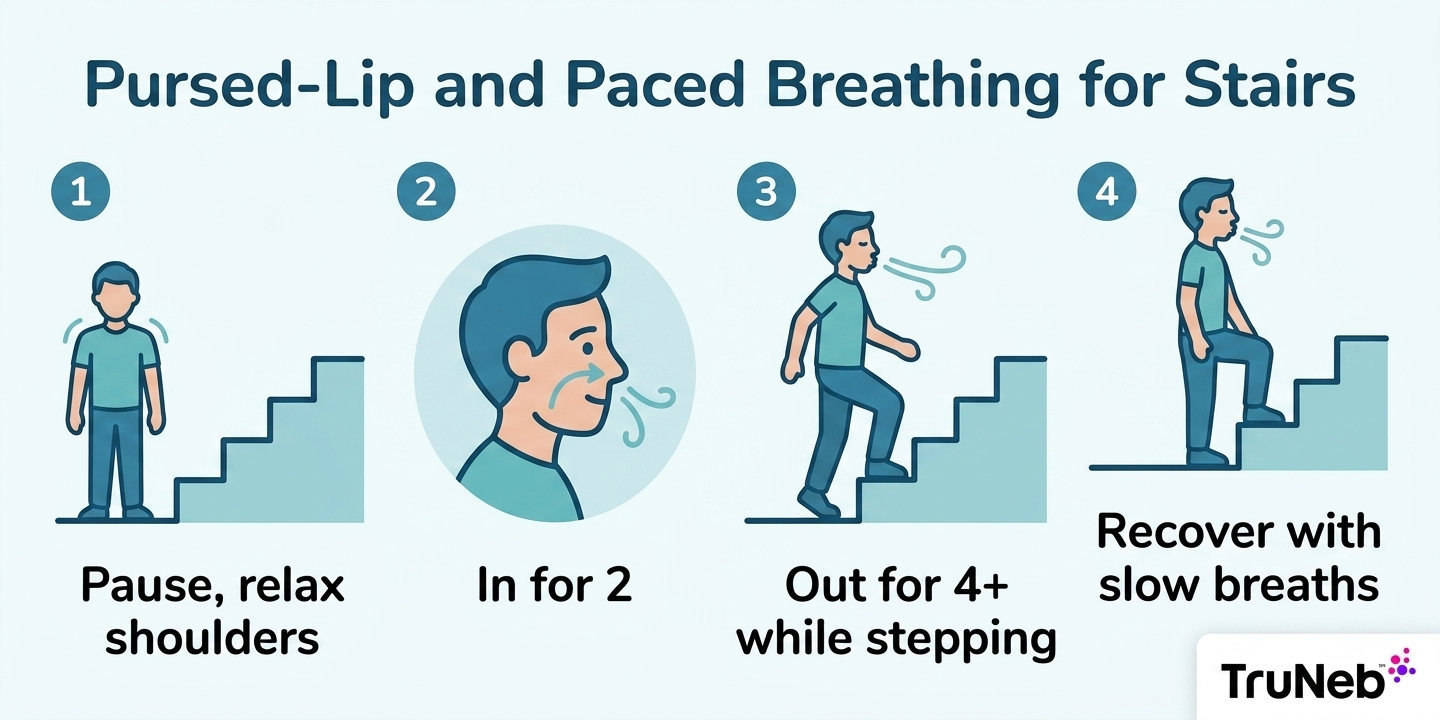
Pursed-lip breathing can help before you feel desperate for air. Relax your shoulders and neck. Breathe in through your nose for about two counts, then breathe out slowly through gently pursed lips for four or more counts. Do not force the air.
Pacing and posture
Some people find it easier to match breathing to their steps. It can help to pause at the bottom before you start, take a steady inhale, then step up as you exhale through pursed lips. Try one step per long exhale. Others prefer two small steps during one slow exhale. Use the rail, start a touch slower, stay tall or slightly forward at the hips, and keep your gaze ahead. Avoid breath-holding.
Diaphragmatic breathing
If your doctor or rehab team has shown you diaphragmatic belly breathing, use it to keep breaths low and steady rather than shallow and fast.
Safety callout
Warning: If breathing becomes severe, or you have chest pain, fainting, blue lips, or sudden worsening, stop and seek urgent care rather than trying to push through.
Recover at landings or the top with a few rounds of pursed-lip breathing until you can speak in short phrases without gasping.
Takeaway: Pursed-lip breathing, steady pacing, and posture can help you control your breathing and reduce that sudden panicky feeling on stairs.
How to Improve Shortness of Breath While Walking and Climbing Stairs
Get cleared first
If symptoms are new, severe, or getting worse, get medical guidance before starting or changing activity. A plan like the one below fits mild, stable symptoms or a cleared return to activity.
Baseline and simple tracking
Note how long you can walk comfortably, how many stairs you can take before you stop, how long recovery takes, and if you can talk in short phrases while moving. Write it down. Some people also use a 0 to 10 Borg scale to rate breathlessness or effort during sessions under a doctor's guidance.
A gentle four-week progression
Week 1: Easy walks 5 to 10 minutes most days, paying attention to breath and recovery time.
Week 2: Add short, slightly faster intervals 30 to 60 seconds with easy walking between.
Week 3: Add gentle inclines or one controlled flight of stairs with a rest at the landing, keeping breathing steady.
Week 4: Add low step-ups or repeat short stair sets with full recovery between rounds. If you can only speak one or two words, ease up or stop to recover.
Strength and the talk test
Exercises like sit-to-stands from a stable chair, calf raises, low step-ups, wall pushups, and gentle squats can build the leg strength used on stairs. If you can talk in short phrases, the effort is usually moderate.
Rehab can help
Consider pulmonary or cardiac rehabilitation if you have a chronic heart or lung condition. These supervised programs tailor exercise to your diagnosis and monitor safety.
Takeaway: For mild, stable symptoms, gradual walking, leg strength, and pacing can improve stair tolerance over time.
If You Have Asthma, COPD, Bronchiectasis, or Mucus-Heavy Lung Disease
Follow your prescribed plan
Use your maintenance inhalers, rescue inhaler, oxygen, nebulized medications, and airway clearance routine as directed by your doctor. Do not change medications on your own.
Airway mucus can make stairs feel harder. Mucus, airway inflammation, and narrowing raise the work of breathing. Clearing mucus as prescribed and using proper breathing techniques can lower that load.
Where a nebulizer fits
If your doctor has recommended nebulized treatments or saline airway clearance, a compact portable mesh nebulizer device like the TruNeb portable mesh nebulizer can make routines easier at home or on the go. A portable device can be easier to keep with you for a prescribed routine at home or while traveling. 3% hypertonic saline solution and 7% saline for mucus clearance is used to support mucus clearance only when recommended by a doctor for the right conditions, for example bronchiectasis or cystic fibrosis. It does not replace rescue medication, oxygen, emergency care, or your doctor's plan.
Consumer note: A nebulizer delivers prescribed inhaled treatments. It is not the same thing as a steam inhaler.
Safety note: Talk to your doctor before trying a new medication.
Takeaway: If you already have a diagnosed lung condition, following your prescribed plan is the safest way to manage breathlessness on stairs.
What to Tell Your Doctor About Stair Breathlessness
What to bring
Share when symptoms began, whether they are new, worsening, or stable; how many stairs or minutes of walking trigger them; and how long recovery takes. Note any chest pain or pressure, wheeze, cough or mucus, palpitations, dizziness, swelling, fever, or recent infection. Include smoking history, recent surgery, long travel, or immobility, and list all medications and inhalers. Mention what helps and what makes it worse, including air pollution or extreme temperatures.
Home readings and timing
If you use a home pulse oximeter, jot down typical readings at rest and during/after stairs, plus how quickly you return to baseline. Share these with your doctor. Track whether symptoms are worse at certain times of day or seasons.
Tests you might get
Depending on your pattern, a doctor can check oxygen saturation, blood counts, and thyroid-stimulating hormone (TSH). An ECG and chest X-ray look for heart and lung clues. Spirometry checks airflow. An echocardiogram and a stress test assess heart structure and response to exertion. If the cause is unclear, more advanced tests can pinpoint whether limits are cardiac, pulmonary, or both.
Takeaway: The more specific you are about triggers, recovery time, and related symptoms, the easier it is for your doctor to narrow down the cause.
Medical Terms You May Hear
Dyspnea: Feeling of hard or uncomfortable breathing.
Exertional dyspnea: Shortness of breath that appears with activity such as stairs, hills, or walking.
Orthopnea: Breathlessness when lying flat that eases when you sit or stand.
Paroxysmal nocturnal dyspnea: Waking from sleep suddenly short of breath that improves when you sit up.
Angina: Chest pressure or discomfort with exertion from reduced blood flow to the heart muscle.
Cardiomyopathy: Disease of the heart muscle that can weaken pumping or stiffen filling.
Aortic stenosis: Narrowing of the aortic valve that limits blood flow out of the heart.
Spirometry: A breathing test that measures airflow to look for obstruction.
Echocardiogram: An ultrasound test that shows heart structure and valve function.
Stress test: A test that looks at heart response to exertion.
Interstitial lung disease: A group of conditions that scar the lungs (for example, pulmonary fibrosis) and make breathing feel stiff.
Pleural effusion: Fluid around the lungs that can cause breathlessness.
Pneumothorax: Air leaking around a lung that can cause sudden shortness of breath and chest pain.
Pulmonary rehabilitation: A supervised program that builds breathing strength and stamina for lung conditions.
Hypertonic saline: A salty solution (such as 3% or 7%) used in doctor-directed airway clearance plans for certain diagnoses.
Airway clearance: Techniques and treatments that help move mucus out of the lungs.
Borg scale: A simple 0–10 rating some people use to describe breathlessness or effort.
Pulse oximeter: A small device that estimates oxygen saturation on your finger.
Takeaway: These terms describe patterns of breathlessness and the tests doctors use to figure out what is causing them.
Frequently Asked Questions
Tap or click a question below to see the answer:
It can be, if symptoms are mild, predictable, and fade within a few minutes of rest—especially after time off or rushing. If it is new, getting worse, severe, or paired with red flags, get medical care.
Hills and stairs make you lift your body against gravity, so oxygen demand and breathing work rise quickly compared with flat walking.
Call 911 for sudden severe breathlessness or if it occurs with chest pain or pressure, fainting, new confusion, blue lips, severe palpitations, coughing blood, or symptoms after long travel or recent surgery.
Heart clues include chest pressure with exertion, relief with rest, fainting, palpitations, swelling, or trouble lying flat. Lung clues include wheeze, cough, mucus, and clear triggers. Only a doctor can diagnose the cause.
Pursed-lip breathing with steady pacing helps many people: inhale through your nose, then exhale slowly through pursed lips as you step. Avoid breath-holding.
Build gradually: easy walks, short intervals, gentle inclines, then controlled stairs with full recovery. Use the talk test; stop and seek care if symptoms are severe.
A nebulizer can help only if it’s part of your prescribed plan for conditions like asthma, COPD, bronchiectasis, or cystic fibrosis. Use it as directed. It does not replace emergency care.
Note how many stairs trigger symptoms, recovery time, and any chest pain, wheeze, palpitations, swelling, fever, or recent infections. If you use a pulse oximeter, write down typical readings and changes.
Breathlessness can happen in pregnancy because oxygen needs and your diaphragm position change. If symptoms are new, severe, or worrying, check in with your doctor.
Some people track typical readings to share with a doctor, but numbers need context. If you’re worried about oxygen levels or symptoms, get medical advice rather than self-diagnosing.