On this page
Venturi Mask Basics – Mechanism and High-Flow Principle
A Venturi mask (also called an air-entrainment mask) is a fixed-performance oxygen device that delivers a precise oxygen percentage (FiO₂) by mixing oxygen with room air using interchangeable adapters.
How it works: oxygen flows through a small jet that entrains room air at a set ratio (air:oxygen) based on the adapter. This follows the Bernoulli principle, where a fast jet of gas creates a pressure drop that pulls in ambient air. The color-coded valve controls that mix so the FiO₂ stays steady even when breathing patterns change.
Why the Venturi Mask is a ‘High-Flow’ Device
At lower FiO₂ settings, the total gas flow to the patient (oxygen plus entrained air) can be very high and usually meets or exceeds how much air a person pulls in when breathing. For example, a 24% setting can reach roughly 100 L/min total flow. That helps keep the oxygen percentage steady.
Why this matters in COPD: in some people with COPD and CO₂ retention risk, too much oxygen can worsen carbon dioxide buildup. A Venturi mask lets clinicians control FiO₂ carefully to balance oxygenation and CO₂. For more on oxygen titration in COPD, see our guide on oxygen use in COPD.
Takeaway: A Venturi mask is a fixed-performance oxygen device that delivers a precise oxygen percentage by mixing oxygen with room air.
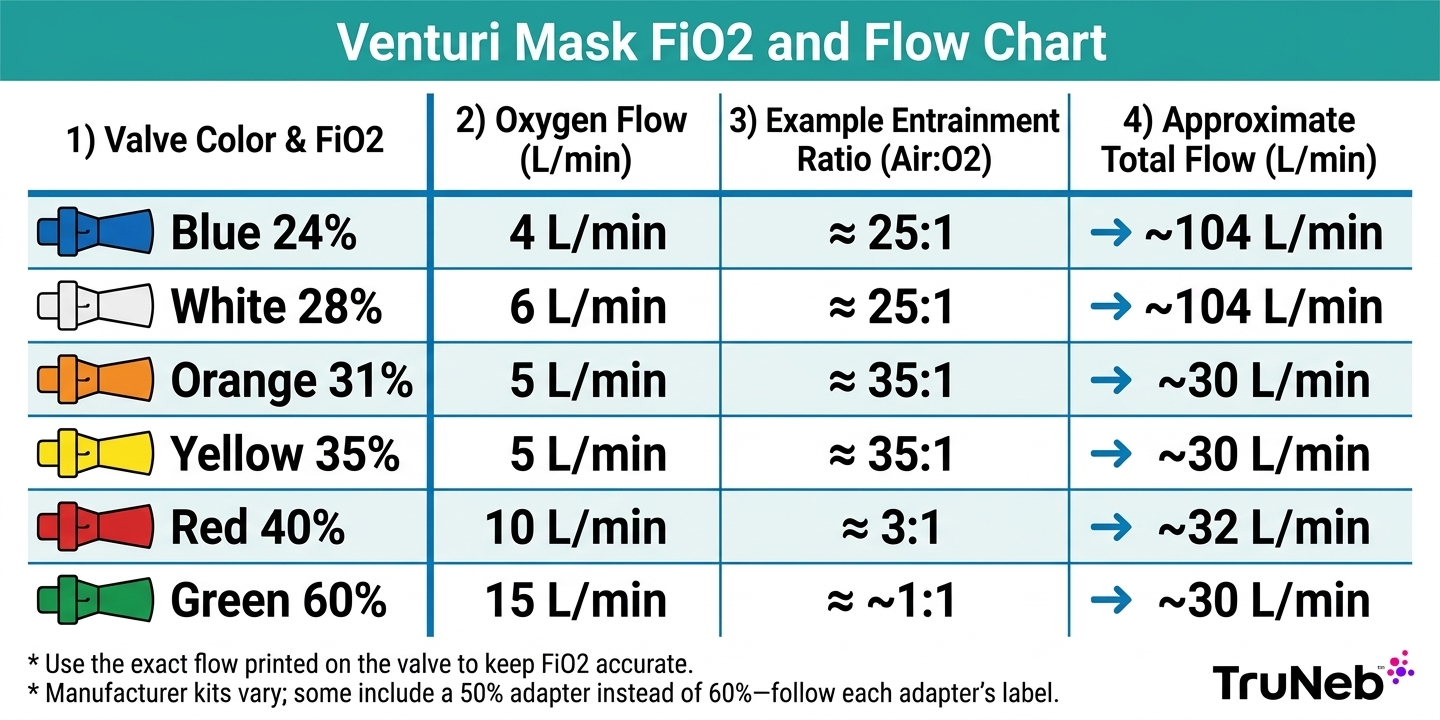

Venturi Mask Oxygen Flow Rates & FiO₂ Settings (Color-Coded Chart)
Quick answer: Venturi mask flow rate depends on the adapter you use, usually ranging from about 2 to 15 L/min. Each color-coded valve is designed to deliver a set FiO₂ when run at the printed oxygen flow.
Here’s what common settings mean in practice (colors can vary by manufacturer):
- 24% (often blue): about 2–4 L/min oxygen, very high total flow, very steady FiO₂.
- 28% (often white): about 4–6 L/min oxygen; a common starting point in COPD.
- 31% (often orange): about 6–8 L/min oxygen.
- 35% (often yellow): about 8–10 L/min oxygen.
- 40% (often red): about 10–12 L/min oxygen; moderate oxygen with control.
- 60% (green): about 12–15 L/min oxygen; one of the highest common Venturi settings.
Note: Valve colors and exact flow ranges differ by manufacturer, so use the setting printed on the adapter. Some kits include a 50% adapter instead of 60%.
Entrainment ratio explained: each adapter draws room air at a set air:oxygen ratio. Lower FiO₂ adapters entrain more room air (higher ratios), which increases the total flow to the patient; higher FiO₂ adapters entrain less room air, so total flow is lower.
What is the flow rate of a Venturi mask?
There isn’t a single rate. It ranges from roughly 2 to 15 L/min depending on the adapter in use.
What does a 28% Venturi mask mean?
It means the 28% adapter is on, and the oxygen source should be set to the flow printed on that adapter (commonly around 4–6 L/min) so the person breathes about 28% oxygen.
How much oxygen does a 40% Venturi mask deliver?
About 40% FiO₂ to the patient when the red adapter is run near its labeled flow (often around 10–12 L/min). For comparison with a higher-oxygen emergency device, see non-rebreather mask flow rates.
The adapter is designed to work at the flow printed on the valve; too little flow can change the mix and deliver a higher FiO₂ than intended.
Takeaway: Venturi mask flow rate is tied to the adapter, with each valve delivering a set FiO₂ when run at the printed oxygen flow.
When to Use a Venturi Mask – Indications and Best Practices
A Venturi mask is typically used when precise FiO₂ is needed, especially for people at risk of CO₂ retention. In COPD with CO₂ retention risk, guidelines commonly target SpO₂ 88–92% and start with lower FiO₂ settings (for example, 24–28%), adjusting based on monitoring. Clinicians interpret response with pulse oximetry and, when needed, arterial blood gases (ABGs). If you need a refresher on what home readings mean, review this pulse oximeter readings chart.
Takeaway: Venturi masks are used when oxygen needs to be controlled carefully, especially in people at risk of CO₂ retention.
Safety Tips for Venturi Mask Use
- Match the oxygen flow to the value printed on the adapter so FiO₂ stays accurate.
- Monitor SpO₂ and how the person is doing overall; clinicians check ABGs when needed to guide care.
- If oxygen levels stay low even on higher Venturi settings (around 50–60%), clinicians typically switch to a higher-support device.
- Standard practice is not to attach a bubble humidifier to a Venturi mask because it can interfere with the intended oxygen–air mix.
⚠️ If oxygen levels stay low, breathing gets harder, or the person becomes confused or very drowsy, seek urgent medical care right away.
Note: This guide is educational. Talk to your doctor before changing oxygen settings or trying a new medication.
Venturi Mask vs Other Oxygen Devices: Non-Rebreather, Simple Mask, HFNC
Takeaway: Venturi masks prioritize precise FiO₂ control, while other oxygen devices are chosen for higher oxygen delivery, simplicity, or added support.
Venturi Mask vs. Non-Rebreather Mask
A non-rebreather (NRB) is used for short periods when very high FiO₂ is needed fast (about 60–90%+ at 10–15 L/min). FiO₂ varies with mask fit and breathing. A Venturi mask typically tops out near 50–60% but keeps FiO₂ more consistent, which matters when too much oxygen could be risky (for example, some people with COPD).
Venturi Mask vs. Simple Face Mask
A simple mask (about 40–60% at 5–10 L/min) gives a less exact oxygen level because FiO₂ changes with breathing. Venturi masks provide a known FiO₂, which helps with careful titration and interpreting ABGs. Run simple masks at ≥5 L/min to reduce CO₂ rebreathing.
Venturi Mask vs. High-Flow Nasal Cannula (HFNC)
HFNC can deliver up to 60 L/min with 21–100% FiO₂ and built-in humidification. It’s used when higher flow, better comfort, or more support is needed. Venturi masks are simpler and useful when controlled FiO₂ on the ward is the main goal. If you want a broader overview, read our high-flow oxygen therapy guide.
Venturi Mask vs. Nasal Cannula
Nasal cannula is comfortable and common in home care, but delivered FiO₂ is approximate and varies with breathing pattern and mouth vs nose breathing. A Venturi mask is used when a more exact FiO₂ is required.
| Device | Typical O₂ flow | Approx FiO₂ | Best for | Key caveat |
|---|---|---|---|---|
| Venturi mask | ~2–15 L/min (per adapter) | ~24–60% (fixed) | Precise FiO₂ control (e.g., COPD with CO₂ retention risk) | Ceiling near 50–60%; follow adapter label |
| Non-rebreather (NRB) | 10–15 L/min | ~60–90%+ | Rapid, higher FiO₂ in acute settings | FiO₂ varies with mask fit and breathing |
| Simple face mask | 5–10 L/min | ~40–60% | Moderate oxygen when precision is less critical | Run ≥5 L/min to reduce CO₂ rebreathing; less exact FiO₂ |
| Nasal cannula | ~1–6 L/min (home use varies) | Approximate; depends on breathing | Comfort and mobility, home oxygen | Less predictable FiO₂ vs Venturi |
| High-flow nasal cannula (HFNC) | Up to ~60 L/min | 21–100% | Higher flow with humidification and comfort | Requires dedicated device and monitoring |
Notes: Ranges are typical; exact values vary by manufacturer and setup. Follow local protocols and device labeling.
Quick way to think about the options
- Need the highest FiO₂ fast in an emergency? NRB provides that.
- Need a consistent, known FiO₂? Venturi is designed for that.
- Need higher flows and humidification for ongoing support? HFNC offers that.

From Hospital Oxygen to Home Care – Nebulizers & Airway Clearance
Hospital oxygen devices and home nebulizers do different jobs, but people with chronic lung disease may hear about both. Oxygen devices raise oxygen levels. A nebulizer doesn’t replace oxygen; it delivers inhaled medicine or saline.
At home, nebulizer therapy is used for selected groups such as people with chronic bronchitis, bronchiectasis, cystic fibrosis, or those prescribed inhaled treatments. A portable mesh nebulizer like TruNeb portable mesh nebulizer can deliver medications or saline as a fine mist. In some care plans, hypertonic saline solution (for example, 3% or 7%) can help thin mucus and improve clearance—something oxygen alone can’t do. These therapies should follow a doctor’s plan.
Takeaway: Oxygen treats low oxygen levels, while nebulizers deliver inhaled treatments that can help with mucus or airway symptoms. You can also learn more in our articles on using a nebulizer with oxygen and airway clearance techniques for bronchiectasis.
Note: Treatments should match your plan. Talk to your doctor before trying hypertonic saline or changing any medication.
Frequently Asked Questions
These quick answers cover the most common questions about Venturi masks, flow rates, and home use. Tap or click a question below to see the answer:
High flow. With the right adapter and oxygen setting, the total flow (oxygen plus entrained room air) can meet or exceed a person’s breathing demand while keeping FiO₂ steady.
It’s uncommon and should be supervised. Most home oxygen uses a nasal cannula or simple mask because they’re easier day to day.
A cannula is comfortable, but FiO₂ is approximate and varies with breathing. Venturi masks are used when a known, consistent FiO₂ is needed.
Venturi masks generally aren’t used with bubble humidifiers because that can affect the intended oxygen–air mix and change FiO₂.
If oxygen levels stay low even on higher Venturi settings, clinicians may switch to a higher-support device (for example, a non-rebreather) or consider HFNC or ventilatory support.
⚠️ Seek emergency care right away for severe shortness of breath, blue lips, new confusion, chest pain, or oxygen levels that stay low despite treatment.
Disclaimer: This article is for informational purposes only and is not a substitute for medical advice. Talk to your doctor about oxygen therapy, medications, and changes to your treatment plan.