On this page
How Much Does an Oxygen Concentrator Cost
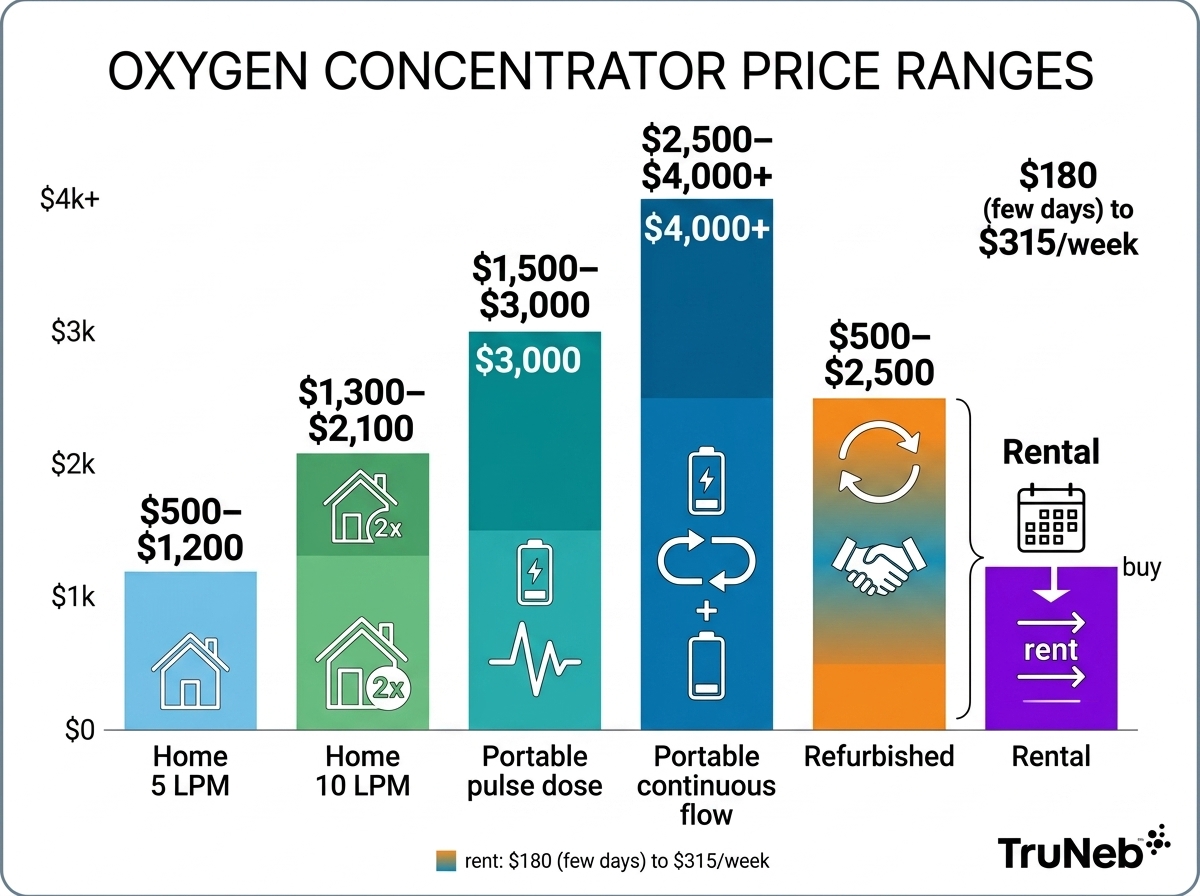
Most people see two price bands. A home (stationary) oxygen concentrator often costs about $500 to $2,000. A portable oxygen concentrator usually runs $1,500 to $4,000 or more, depending on features and batteries. Certified used or refurbished machines can start around $500 to $1,500. Short-term portable rentals often cost around $180 for a few days to about $300 per week.
What these devices do: An oxygen concentrator pulls oxygen from room air to deliver medical-grade oxygen for people who are prescribed oxygen therapy.
Key point: Don’t judge by sticker price alone—match the device to your prescription first, then compare warranty, batteries, and total monthly costs.
| Oxygen option | Typical price range | Best fit |
|---|---|---|
| 5 LPM home (stationary) concentrator | $500 to $1,200 | Home use with continuous flow at lower to moderate LPM |
| 10 LPM home (stationary) concentrator | $1,300 to $2,100 | Higher-flow home oxygen needs |
| Portable pulse-dose concentrator | $1,500 to $3,000 | Active users who qualify for pulse dose |
| Portable continuous-flow concentrator | $2,500 to $4,000+ | Users needing portable continuous flow |
| Used or refurbished unit | $500 to $2,500 | Budget buyers, backups; warranty required |
| Rental portable concentrator | $180 per short rental to ~$315/week | Travel, temporary use, try-before-you-buy |
One-liner: Home oxygen concentrators are usually hundreds to low thousands, while portable units cost more because of batteries and travel-ready design.
Why Oxygen Concentrator Prices Vary So Much
Several design choices change the price: how oxygen is delivered, how much flow you need, and how portable the device must be.
Flow Type
Continuous flow sends oxygen in a steady stream. Pulse dose sends short bursts only when you inhale. Portable continuous-flow machines are larger and usually cost more than pulse-dose models. Your prescription rules this choice.
Flow Capacity
Many home units deliver up to 5 liters per minute (LPM); higher-flow models reach 10 LPM. More capacity typically costs more.
Portability and Battery Life
Portable concentrators pack sensors, lightweight housings, and lithium batteries. Extra or extended batteries raise total price. FAA-accepted models for airline travel involve added testing and documentation and are still subject to airline rules.
Core Components and Durability
Inside every concentrator are a compressor and sieve beds that separate oxygen from room air. Heavier-duty compressors and larger or longer-lasting sieve beds add cost up front, but can reduce maintenance frequency and repair risk later.
New, Refurbished, and Used Condition
New devices include current models and a full warranty. Certified refurbished units can save money if the supplier tests oxygen purity, replaces filters or columns, checks the sieve beds, and discloses operating hours. Warranty length matters.
Accessories and Package Contents
Cannulas, oxygen tubing, swivel connectors, oxygen masks, humidifier bottles, filters, carry cases, carts, chargers, and spare columns or batteries can change the final price. Check what’s in the box before judging value.
One-liner: Price climbs with continuous flow, higher LPM, lighter weight, longer battery life, and stronger warranty support.
Home Oxygen Concentrator Prices
Typical Home Unit Price Ranges
Home (stationary) concentrators are built for steady, continuous flow. Typical ranges: standard 5 LPM models about $500 to $1,200; higher-flow 10 LPM models about $1,300 to $2,100; compact premium home units about $1,600 to $2,000.
Best Use Cases for Home Units
A home unit makes the most sense for overnight oxygen, daily continuous oxygen at home, or oxygen bleed-in to CPAP or BiPAP when prescribed. If you don’t need frequent outside mobility, a stationary oxygen concentrator usually delivers the best value.
What to Compare Before Buying
Check the LPM on your prescription, noise level for sleep, weight and wheels for room-to-room use, estimated electricity use, warranty length, supplier support and return policy, and availability of routine parts like filters, humidifier bottles, and masks. If a home unit lists a very low price, make sure it still meets your required LPM and continuous-flow needs.
One-liner: A standard 5 LPM home oxygen concentrator covers many prescriptions for hundreds of dollars less than most portable units.
Portable Oxygen Concentrator Prices
Typical Portable Unit Price Ranges
Portable oxygen concentrators (POCs) are built for errands, appointments, and travel. Lightweight pulse-dose models often cost $1,500 to $3,000. Premium pulse-dose models tend to be $2,400 to $3,000. Portable devices that can deliver continuous flow generally range $3,000 to $4,000 or more. Certified refurbished POCs can land around $1,000 to $2,500 depending on hours and condition.
Why Portable Units Cost More
They add batteries, smart sensors, compact housings, and FAA-accepted design and labeling for air travel—still subject to airline rules. Extended batteries, external chargers, and carry cases raise the total.
Travel Cost Considerations
Travel can raise the total cost. You may need spare batteries, a car charger, and an airline-accepted setup with enough battery capacity for the whole flight plus buffer time. Some travelers rent a POC for a single trip to test before buying. Examples of market options include Inogen Rove 6, CAIRE Freestyle Comfort, SeQual Eclipse 5, and OxLife Independence (examples only, not endorsements).
One-liner: You pay more for mobility—POCs add batteries and travel features that home units don’t need.
New, Used, Refurbished, and Rental Oxygen Concentrators
Buying New
Buying new means current models, a full warranty, and lower risk, but it’s the highest upfront cost. Work with a reputable Durable Medical Equipment (DME) supplier so service and parts are clear.
Buying Used or Refurbished
Certified refurbished or used units can save money and work well as backups if the DME supplier tests oxygen purity, replaces wear parts, and backs the device with a real warranty. Ask about the hour meter (total operating hours), sieve-bed condition, compressor checks, and documented purity. If you see an oxygen concentrator for sale online without proof of testing, be cautious.
Payment options to ask about: HSA/FSA eligibility and financing plans that spread costs without large fees.
Renting
Rentals are usually best for short-term needs, like recovery or travel, or while you wait for insurance approval. Get the weekly rate and calculate the break-even point versus buying, because long rentals can add up fast.
Quick questions: Who refurbished it and how? How many hours are on it? What’s the warranty and who services it? Does it match your prescription (flow type and LPM)? Which accessories are included (tubing, cannulas, oxygen mask, batteries, charger, bag)? What’s the rental’s minimum term and return policy?
One-liner: Rentals are helpful for short trips or recovery, but months of weekly fees can outpace a purchase.
How Insurance Changes Home Oxygen Costs
Insurance changes how you pay and what you receive.
Medicare
Medicare Part B may cover rental of oxygen equipment and accessories for home use when you qualify. After you meet the Part B deductible, you typically pay 20% of the Medicare-approved amount. Rental payments usually last 36 months. If you still need oxygen, your DME supplier must keep providing covered equipment and supplies for up to 5 years total (the equipment’s useful lifetime). Medicare generally does not pay for oxygen used specifically for air travel. Coverage of a portable oxygen concentrator with Medicare depends on medical need, documentation, and supplier availability.
Private Insurance
Plans often require prior authorization, a prescription, and medical documentation. You may need to use in-network DME suppliers, meet a deductible, and pay coinsurance. Ask if the plan covers purchase, rental, or both, and whether a portable unit is covered along with a home unit.
Medicaid and VA Benefits
Medicaid coverage varies by state rules and medical need. The VA may cover oxygen equipment for eligible veterans. Always confirm documentation requirements and approved suppliers.
Medicare Advantage and Medigap
Medicare Advantage (Part C) plans manage coverage through their own networks and rules; coinsurance and supplier access can differ from Original Medicare. Medigap doesn’t add benefits, but it can help pay your share of Original Medicare’s costs.
How You Qualify Clinically (in plain language)
Doctors prescribe oxygen when you have low blood oxygen (hypoxemia) from conditions like normal lungs vs COPD lungs, emphysema, chronic bronchitis, pulmonary fibrosis, pneumonia recovery, cystic fibrosis, some heart failure, or certain sleep-related disorders. Qualification is based on measurements such as oxygen saturation by pulse oximetry or arterial blood gas, along with medical records.
Questions to ask: Is this DME covered as a rental or purchase? What documentation is required? Which suppliers are in network? What is the monthly coinsurance after my deductible? Are accessories included? What happens if I travel?
⚠️ Safety: Do not use oxygen equipment or change oxygen flow settings without your doctor’s instructions. Oxygen supports combustion—follow fire safety at home and when traveling.
⚠️ Emergency: Seek emergency care right away for severe shortness of breath, chest pain, blue lips, confusion, or suddenly worsening breathing symptoms.
Disclaimer: This article is for informational purposes only and is not a substitute for medical advice. Always follow your doctor’s instructions about oxygen therapy, medications, and respiratory equipment.
Key point: Under Medicare, many patients pay 20% coinsurance after the Part B deductible for covered oxygen rentals, with a 36-month rental period and supplier obligations up to 5 years.
One-liner: Coverage rules can lower costs—but they also set the path (usually rental first) and the suppliers you can use.
Oxygen Concentrator vs Oxygen Tank Costs
Oxygen tanks have lower upfront costs but need regular refills or delivery. Concentrators cost more upfront but make oxygen from room air and avoid refill trips. Many care plans still keep a tank for backup during power outages or specific activities. Some patients use liquid oxygen systems in certain programs; these can be convenient for higher-flow portability but require specialized delivery and handling.
| Option | Upfront cost | Ongoing cost | Best fit |
|---|---|---|---|
| Oxygen tank (compressed) | Lower | Refills and delivery | Backup or short-use needs |
| Home concentrator | Medium | Electricity and supplies | Daily home oxygen |
| Portable concentrator | Higher | Batteries and supplies | Mobility and travel |
Note: Liquid oxygen systems are another option where available; costs and delivery models vary by region and supplier.
As a reference point for tank hardware, one retailer lists approximate tank purchase prices like M2 around $75, M4 and M6 around $70, M9 around $80, an E-cylinder around $100, and an H-cylinder around $600 to $700. Treat these as examples, not universal prices.
One-liner: Tanks can be cheaper at the start, but concentrators often win over time by avoiding frequent refills.
Total Cost of Ownership
Think in months and years, not just the day you buy.
Electricity
Monthly electricity cost = watts ÷ 1,000 × hours per day × 30 × local kWh rate. Example: a 350-watt home unit used 24 hours per day at $0.16/kWh is roughly 0.35 × 24 × 30 × $0.16 ≈ $40 per month. Portable units use less while on battery but need charging time.
Accessories
Plan for routine items like nasal cannulas, oxygen tubing, swivel connectors, oxygen masks, humidifier bottles, and intake or cabinet filters. These are small costs that add up over time. A carry bag or rolling cart can help at home. For portable units, include chargers and any extra batteries you truly need.
Portable Batteries
Extra or extended batteries are the biggest add-on for POCs. Buy what matches your real use: daily errands may only need one spare; long flights usually need multiple spares to meet airline rules. Remember oxygen concentrator battery replacement cost over time—many batteries need replacement after a few hundred cycles or a couple of years of regular use.
Maintenance and Repairs
Suppliers recommend filter changes and periodic oxygen purity checks. Sieve beds and compressors are core components; warranties can protect you from large repair bills during the covered period.
Lifespan
With routine maintenance, many home concentrators are designed to run tens of thousands of hours. Some retailer guidance notes typical operation lifespans around 20,000 to 30,000 hours for many home units.
One-liner: Your monthly cost is the sum of electricity, supplies, and any batteries or maintenance—not just the purchase price.
Real World Cost Examples
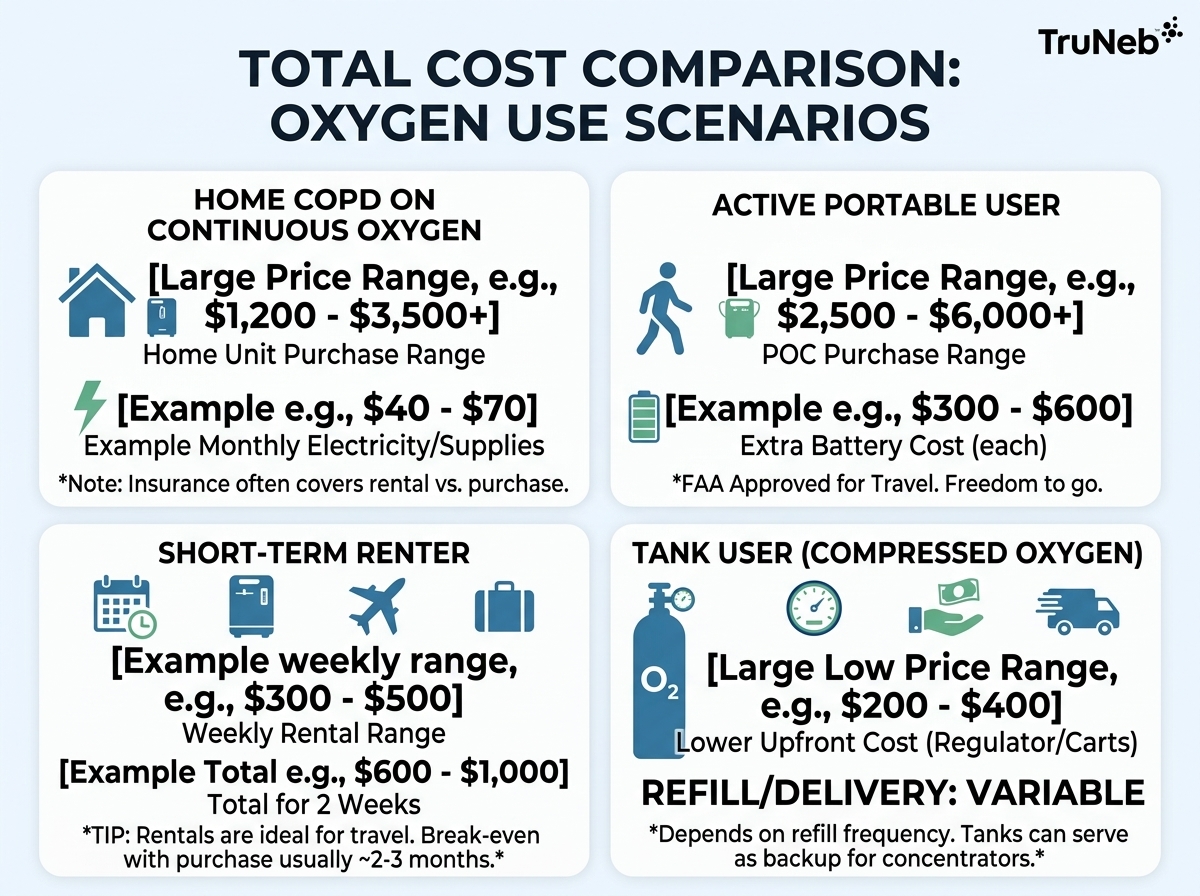
COPD Patient Using Continuous Home Oxygen
A home user on continuous flow might choose a 5 LPM unit around $700 to $1,200 (or 10 LPM around $1,300 to $2,100 if prescribed). Monthly electricity can be a few tens of dollars depending on watts and local rates. If eligible, Medicare may cover a rental with 20% coinsurance after the Part B deductible.
Active User Who Needs Portable Oxygen
A pulse-dose POC may cost $1,500 to $3,000; a continuous-flow-capable portable can be $3,000 to $4,000+. Extra batteries and a car or external charger can add several hundred dollars. Medicare generally will not pay for oxygen used specifically for air travel.
Caregiver Buying a Backup
A certified refurbished home unit can make sense as a backup if it meets your prescription and passes oxygen purity checks with a warranty. Some households keep an oxygen tank for power outages as part of an emergency plan.
Short-Term User Considering Rental
For recovery or a vacation, a rental can be the practical move. But run the math: several weeks of rental can exceed the price of a basic home unit or a used POC.
One-liner: Plan your budget by scenario—home user, active traveler, backup buyer, or short-term renter each face different cost drivers.
How to Choose the Right Oxygen Setup for Your Budget
Start With the Prescription
Your prescription decides the device: pulse dose or continuous flow, and the exact LPM. Don’t compromise on medical needs to chase a lower price. Doctors prescribe oxygen for low blood oxygen (hypoxemia) from conditions such as COPD, emphysema, chronic bronchitis, pulmonary fibrosis, pneumonia recovery, cystic fibrosis, some heart failure, or certain sleep-related disorders—based on measurements like oxygen saturation by pulse oximeter readings chart or arterial blood gas.
Match Device Type to Daily Life
| If you need | Consider | Avoid |
|---|---|---|
| Nighttime continuous oxygen | Home continuous-flow concentrator | Pulse-dose-only POC unless prescribed |
| High-flow oxygen | 10 LPM home unit | Low-output portable unit |
| Travel and errands | FAA-accepted portable concentrator | Heavy home unit for on-the-go use |
| Short-term oxygen | Rental or covered DME | Large cash purchase you won’t use long |
| Backup oxygen | Tank or reliable backup unit | Unverified used device without testing |
Note: Airline rules still apply even for FAA-accepted models.
Compare Package Contents
Check what’s in the box: batteries and chargers for POCs, cannulas and tubing, oxygen mask, humidifier bottle, filters, warranty, and return policy. Small parts change real cost.
Avoid Unsafe Shortcuts
You’ll see non-medical oxygen gadgets online. They are not the same as prescription oxygen concentrators. Medical oxygen concentrators require a prescription; insurance also requires documentation and approved supplier steps.
One-liner: Choose the machine that fits your prescription and daily rhythm, then compare price, warranty, and what’s included.
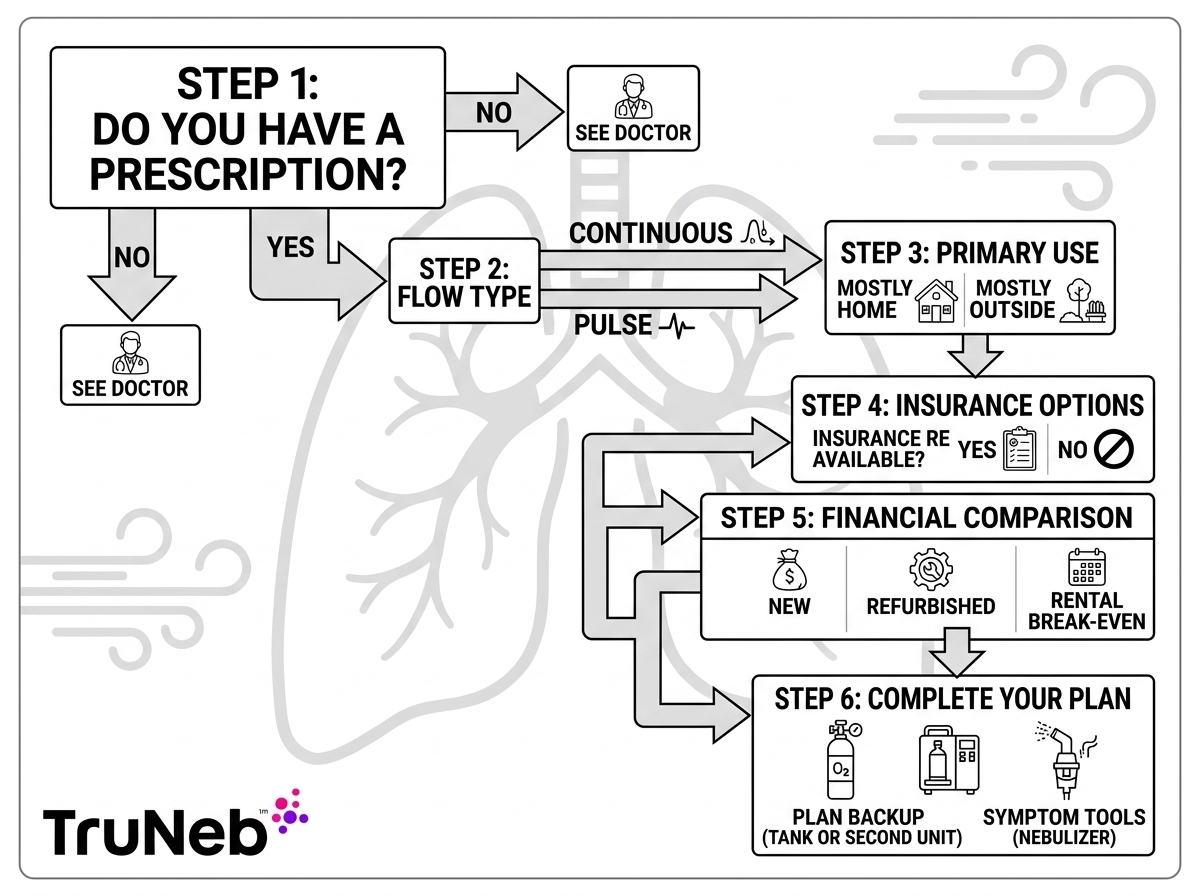
Where TruNeb Fits in a Respiratory Care Budget
Oxygen therapy treats low blood oxygen. A nebulizer does something different: it delivers prescribed medications or saline as a mist to fit into symptom-management routines like mucus clearance and airway hydration when your doctor recommends it.
The TruNeb Portable Mesh Nebulizer and compatible saline solutions (including hypertonic saline when prescribed) can fit alongside oxygen therapy for people whose care plans include nebulized treatments. It can be used for prescribed medication or saline routines when your doctor recommends nebulized therapy—never as a replacement for prescribed oxygen.
If symptoms change or you’re unsure how to combine treatments, talk with your doctor or a respiratory therapist. Build a budget that separates oxygen equipment from nebulizer supplies, saline, inhalers, tubing, and doctor visits.
⚠️ Emergency: Seek emergency care right away for severe shortness of breath, chest pain, blue lips, confusion, or rapidly worsening breathing.
One-liner: A portable mesh nebulizer like TruNeb can support prescribed medication or saline routines, but it does not replace oxygen therapy for low blood oxygen.
Buying Checklist Before You Pay
Before you buy, check the essentials.
1) Confirm your prescription flow type (pulse vs continuous) and LPM. 2) Verify the device matches home, sleep, or travel needs. 3) Ask if your plan covers rental or purchase and which DME suppliers are in network. 4) Compare new vs refurbished vs rental and note the break-even point. 5) Check warranty length and repair support. 6) Confirm what’s included (cannulas, oxygen mask, tubing, filters, humidifier bottle, batteries, chargers). 7) Ask about oxygen purity testing and the hour meter on used units. 8) Set a backup plan for power outages. 9) If you use nebulized therapy, keep that decision separate from oxygen equipment unless your doctor advises otherwise. 10) Ask about HSA/FSA eligibility and financing options if paying cash. 11) Avoid non-medical devices that claim to provide oxygen without a prescription.
One-liner: The right buy is safe, prescription-matched, warranty-backed, and clear on total monthly costs.
Frequently Asked Questions
Tap or click a question below to see the answer:
Home units are about $500–$2,000. Portable units are usually $1,500–$4,000+. Used/refurbished and rentals can lower the upfront cost—compare warranty and what’s included.
They add batteries, light housings, sensors, and FAA-accepted design for travel. Extra batteries and chargers raise total cost.
Medicare Part B may cover oxygen as a rental when medically necessary. Coverage of a portable oxygen concentrator with Medicare depends on your medical need and your DME supplier’s inventory.
Medical oxygen concentrators require a prescription. Be cautious with non-medical oxygen gadgets sold online—they are not the same thing.
Short-term rental is usually cheaper. For longer use, weekly fees can exceed a purchase. If using insurance, rules often start with rental.
Use watts ÷ 1,000 × hours/day × 30 × your kWh rate. Example: 350 watts 24/7 at $0.16/kWh is roughly $40/month.
It varies by supplier, cylinder size, delivery, and region. Frequent refills can cost more over time than owning a concentrator. Liquid oxygen systems are another option in some areas.
Choose certified refurbished units from reputable DME suppliers. Look for a warranty, documented purity testing, and the hour meter reading.
The one that matches your prescription (flow type and LPM), fits your space and noise needs, and comes with solid service and warranty support.
Start with reputable DME suppliers who can verify testing, provide a warranty, and match your prescription. Be wary of listings without proof of medical-grade performance.
No. A nebulizer can help deliver prescribed medication or saline, but it doesn’t treat low blood oxygen or replace prescribed oxygen therapy.