On this page

Does a Nebulizer Help with COVID-19 Symptoms?
Short answer: a nebulizer can help some COVID-19 symptoms, but it doesn’t treat the virus.
If you’re wondering whether to use a nebulizer for COVID symptoms, it helps to know what it can and can’t do.
Portable Nebulizer: Purchase HERE
A nebulizer turns liquid medicine into a fine mist you breathe in. For many people, COVID-19 causes cough and irritation, not always tight, narrow airways. If you have asthma or COPD and COVID-19 sets off wheezing or chest tightness, a bronchodilator (like albuterol) by nebulizer can open airways and make breathing easier.
If you don’t have a lung condition that needs inhaled medicine, a nebulizer usually doesn’t do much for a typical dry COVID cough. It is a tool for airway symptoms, not an antiviral treatment. If breathing feels hard or you’re unsure what you need, call your doctor. If COVID-19 is causing severe shortness of breath or suspected pneumonia, a home nebulizer isn’t enough—those situations need urgent medical care.
A nebulizer can ease COVID-related wheeze or bronchospasm, but it does not treat the virus itself.
Nebulized Saline and Other Treatments: Are They Effective for a COVID Cough?
Hypertonic saline is sterile salt water that is saltier than normal (3% or 7%). When nebulized, it can pull water into the airways and thin thick mucus. Your doctor might use it to help you clear thick mucus in certain lung conditions. For COVID-19, saline can sometimes help if you’re dealing with mucus after the infection, but it is not a proven treatment for the virus. Using hypertonic saline for a COVID-related cough is an off-label, symptom-focused approach that should only be part of a doctor-directed care plan, not a stand-in for recommended COVID treatments.
If your doctor recommends saline, medical-grade options like TruNeb™ 3% and 7% Hypertonic Saline Solutions are designed for nebulizers. Use only what your doctor prescribes and follow the label.
⚠️ Do not add new medicines, home mixtures, or products like hydrogen peroxide, essential oils, or household cleaners to your nebulizer—these can harm your lungs.
Talk to your doctor before trying a new medication or saline strength.
In short, nebulized hypertonic saline can thin mucus and make coughs easier to clear after COVID, but it hasn’t been proven to treat the virus itself.
When Should You Use a Nebulizer If You Have COVID-19 (and When Not)?
- If you already use a nebulizer for asthma, COPD, or another lung condition, keep following your doctor’s plan. Staying on your prescribed inhaled meds can prevent dangerous flare-ups, even if you have COVID-19.
- If you don’t have a prescription for nebulized meds, don’t start one for COVID-19 on your own. Most dry, mild COVID coughs don’t need a nebulizer. Call your doctor if you’re unsure.
- ⚠️ Get urgent care for warning signs—fast or struggling breathing, blue or gray lips, chest pain that won’t go away, confusion, or oxygen levels dropping. A home nebulizer is not enough; call emergency services or go to the ER right away.
- Nebulizer vs inhaler for COVID: if you can use a metered-dose inhaler with a spacer, many doctors prefer that during contagious illness because it doesn’t fill the room with extra aerosol. Ask your doctor what’s best for you.
Nebulizer or Inhaler – Which Should COVID Patients Use?
An inhaler with a spacer delivers bronchodilator medicine effectively without creating room aerosol, so it’s usually safer around others. A nebulizer can be appropriate if you can’t coordinate an inhaler or need longer, steady dosing—follow your doctor’s plan. If a nebulizer is your only option, use it in isolation with ventilation and clean your equipment after each treatment.
A nebulizer doesn’t prevent COVID-19 or stop it from getting worse; it’s only for managing certain breathing symptoms when your doctor has prescribed it.
Rule of thumb: use your nebulizer when it’s part of your prescribed care; don’t add new treatments without medical advice.
How to Use a Nebulizer Safely at Home When You Have COVID-19
Nebulizers create a visible mist. That mist can linger in the air and can carry virus breathed out during coughing.
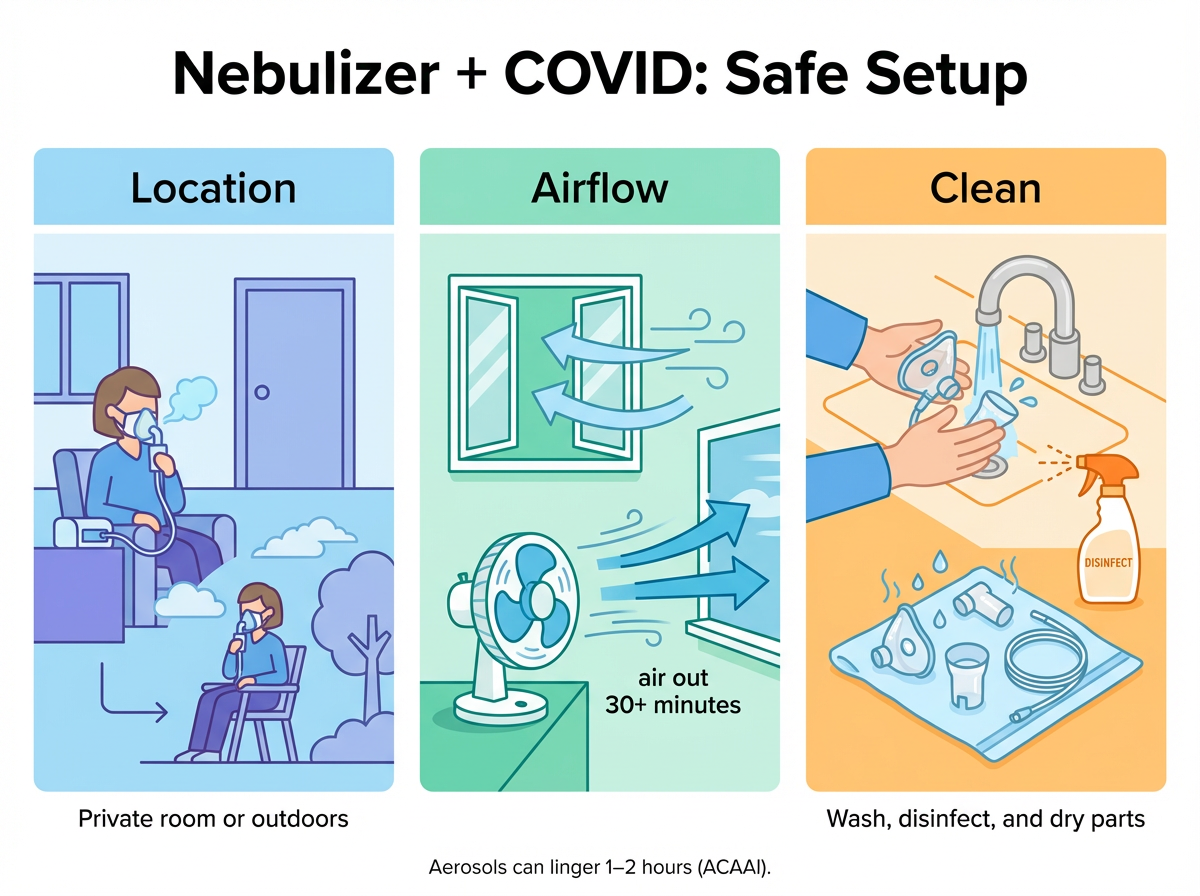
Early guidance from allergy and respiratory groups such as the American College of Allergy, Asthma & Immunology (ACAAI) warned that coronavirus particles can stay airborne in an enclosed space for up to 1–2 hours after nebulizer use. Because nebulizing is considered an aerosol-generating procedure, it can increase aerosol transmission risk if you don’t isolate and ventilate. That’s why location, airflow, and cleaning matter.
- Choose a safe spot. Use the nebulizer alone in a closed room with windows open, or step outside to a porch, balcony, or garage if weather allows.
- Ventilate. Open windows and run a fan to move air out. After you finish, keep the room aired out for at least 30 minutes.
- Protect helpers. If someone must assist (for a child or elder), they should wear a well-fitted N95 and eye protection, and stay out of your direct exhaled airflow.
- Use a mouthpiece if you can. It can reduce leakage compared with a face mask. If your kit has an exhalation filter, attach it as directed.
- Post-session hygiene. Put on a mask before leaving the room. Wipe nearby surfaces where droplets might settle.
- Clean your gear. Wash the cup and mouthpiece or mask with warm soapy water, rinse, and air-dry. Disinfect as your manufacturer directs. No one else should use your set.
⚠️ Don’t confuse steam inhalers or facial steamers with nebulizers—they don’t deliver medication to your lungs and shouldn’t be used as breathing treatments.
Some infection-control guidance and CDC summaries note that most aerosol from a nebulizer comes from the medication, not body fluids. Even so, coughing during treatment can release virus, so keep up the precautions.
Bottom line: isolate, ventilate, and clean—those three steps make home nebulizer use safer when you have COVID-19.
Choosing the Right Nebulizer: Jet vs. Mesh (Why It Matters During COVID-19)
Jet nebulizers use a compressor and tubing. They work well but are bigger, plug into the wall, and can be noisy. Mesh nebulizers are small, quiet, and battery-powered. They use a vibrating mesh to make a fine mist.
For home isolation, a portable mesh unit is easy to carry to a porch or a well-ventilated room, and treatments are often shorter. That convenience can make safe use simpler.
Example: The TruNeb™ Portable Mesh Nebulizer is pocket-sized, quiet, and USB-rechargeable, so you aren’t tied to an outlet. Both jet and mesh nebulizers generate aerosol and carry similar infection-spread risk, so follow the same safety steps with either type.
| Feature | Jet nebulizer | Mesh nebulizer |
|---|---|---|
| Power | Wall plug with compressor | Battery/USB rechargeable |
| Noise | Louder | Quiet |
| Portability | Bulky, less portable | Small, travel-friendly |
| Treatment time | Longer on some models | Often shorter |
| Medication compatibility | Wide range of solutions | Most standard solutions |
| Cleaning | Multiple parts to wash | Fewer parts, still need daily cleaning |
Times and performance vary by device and medication.
Bottom line: mesh is small and quiet, but both mesh and jet need the same safety steps.
FAQs: Using a Nebulizer During COVID-19
Here are quick answers to common questions about using a nebulizer during COVID-19. Tap or click a question below to see the answer:
Yes. If it’s part of your prescribed plan (for asthma or COPD), keep using it as your doctor directed and follow precautions to protect others. Use it in a separate, well-ventilated space and clean the equipment after each treatment.
A nebulizer can be safe to use when it’s prescribed and you take steps to protect others. Use it alone in a ventilated room, keep doors closed, and disinfect parts after. If you’re unsure, ask your doctor.
It can help if the cough comes with wheeze or tight airways. For a typical dry COVID cough, a nebulizer probably won’t help much unless your doctor identifies bronchospasm.
Yes, nebulizing is an aerosol-generating procedure, and the mist can linger in the air, especially in closed rooms. Isolate during treatment, improve airflow, and avoid having others in the room.
An inhaler with a spacer delivers medicine without filling the room with aerosol, so it’s usually better around others. A nebulizer is reasonable if you can’t use an inhaler effectively—follow your doctor’s advice and safety steps.
Conclusion & Key Takeaways
- Nebulizers can help certain COVID-19 symptoms, especially if you have asthma or COPD and your airways get tight. They do not treat the virus.
- So yes, using a nebulizer for COVID can be helpful for certain airway symptoms—but always as part of your doctor’s plan, not as a stand-alone cure.
- Use them safely: isolate, ventilate, and clean.
- If your doctor recommends home nebulizer therapy, a portable mesh device like TruNeb™ can make it easier to take treatments in a safe spot.
Talk to your doctor before trying a new medication or changing any saline strength.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always talk with your doctor about your symptoms, conditions, and before starting, changing, or stopping any treatment.