On this page
White Foamy Mucus: Causes, Treatment, and When To Seek Help
White foamy mucus, also called frothy sputum, is mucus that looks white, bubbly, and a bit thick when you cough it up or clear your throat. A small amount can come from mild irritation, postnasal drip, or a simple cold. Larger amounts, especially with trouble breathing or chest pain, can be a sign of a more serious lung or heart problem.
We’ll walk through what white foamy mucus usually means, which causes are mild or serious, and how to decide between home care, a clinic visit, or the ER.
Sometimes it’s part of a simple cold. Other times, especially if it turns pink or comes with severe breathing trouble, it can be a medical emergency.
One-line: White foamy mucus is usually from irritation or infection, but big changes, pink foam, or breathing trouble can signal an emergency.
What White Foamy Mucus Actually Is
Your airways are lined with tiny glands that make mucus all day long. This thin, slippery fluid keeps your nose, throat, and lungs moist and traps dust, germs, and smoke so your body can move them out.
White foamy mucus happens when that mucus:
- Becomes thicker or more plentiful than usual
- Gets mixed with lots of tiny air bubbles as you breathe or cough
This makes the mucus look white, cloudy, and bubbly instead of clear and smooth.
Strong coughing or fluid in the lungs can whip extra air into mucus, which is what gives it that bubbly, foamy look.
Color also gives clues. Clear or white mucus can be normal, or it can show mild irritation, allergies, or early infection. Yellow or green mucus usually points toward a stronger infection. Pink, red, or brown mucus can mean bleeding and usually needs prompt attention from a doctor.
One-line: White foamy mucus is just regular mucus that has turned thicker, cloudier, and full of tiny air bubbles.
Mild Causes Around Your Nose and Throat
Plenty of people first notice white foamy mucus from nose and sinus problems, not from deep inside the lungs.
Postnasal drip is a top cause. Your nose and sinuses make extra mucus from:
- A cold or flu
- Seasonal allergies
- Dry air or dust
Instead of running out the front of your nose, this mucus slides down the back of your throat. You feel a constant need to swallow, clear your throat, or cough. As this thick drainage mixes with saliva and air, you can see white foamy mucus from your throat.
Allergies usually add itching, sneezing, and clear or white mucus that feels slippery but not sticky. Dry indoor air and smoke can do the opposite, drying your mucus and making it thicker and frothier.
Try to stay away from cigarette smoke and harsh fumes, since they can thicken and irritate mucus even more.
Acid reflux (GERD) is another common trigger. Stomach acid that splashes up can irritate the back of your throat and voice box. Your body tries to protect those tissues by making more mucus. That extra white mucus can pool overnight and look foamy when you cough or clear your throat in the morning.
One-line: Postnasal drip, allergies, and acid reflux are very common, mild reasons for white foamy mucus in the throat.
Infections That Can Cause White Foamy Mucus
Short-term infections in your airways are another common source of white foamy mucus.
Viral colds and flu usually start with clear, runny mucus. After a couple of days, your immune system sends more white blood cells into the area. The mucus can turn thicker and cloudy white and might look foamy when you cough it up or clear your throat.
Acute bronchitis is an infection of the large breathing tubes in your chest. At first the cough is dry. As swelling and mucus build up, you can start coughing up white or clear, frothy sputum. The cough often gets worse at night and first thing in the morning.
Pneumonia is a deeper infection inside the air sacs of the lungs. White foamy mucus can appear with pneumonia in milder or early cases, especially with viral or “walking” pneumonia. As the infection grows stronger, the mucus can turn yellow or green and you might have fever, chills, chest pain when you breathe in, and shortness of breath.
One-line: Colds, bronchitis, and pneumonia can all cause white foamy mucus, especially in the first days before mucus turns yellow or green.
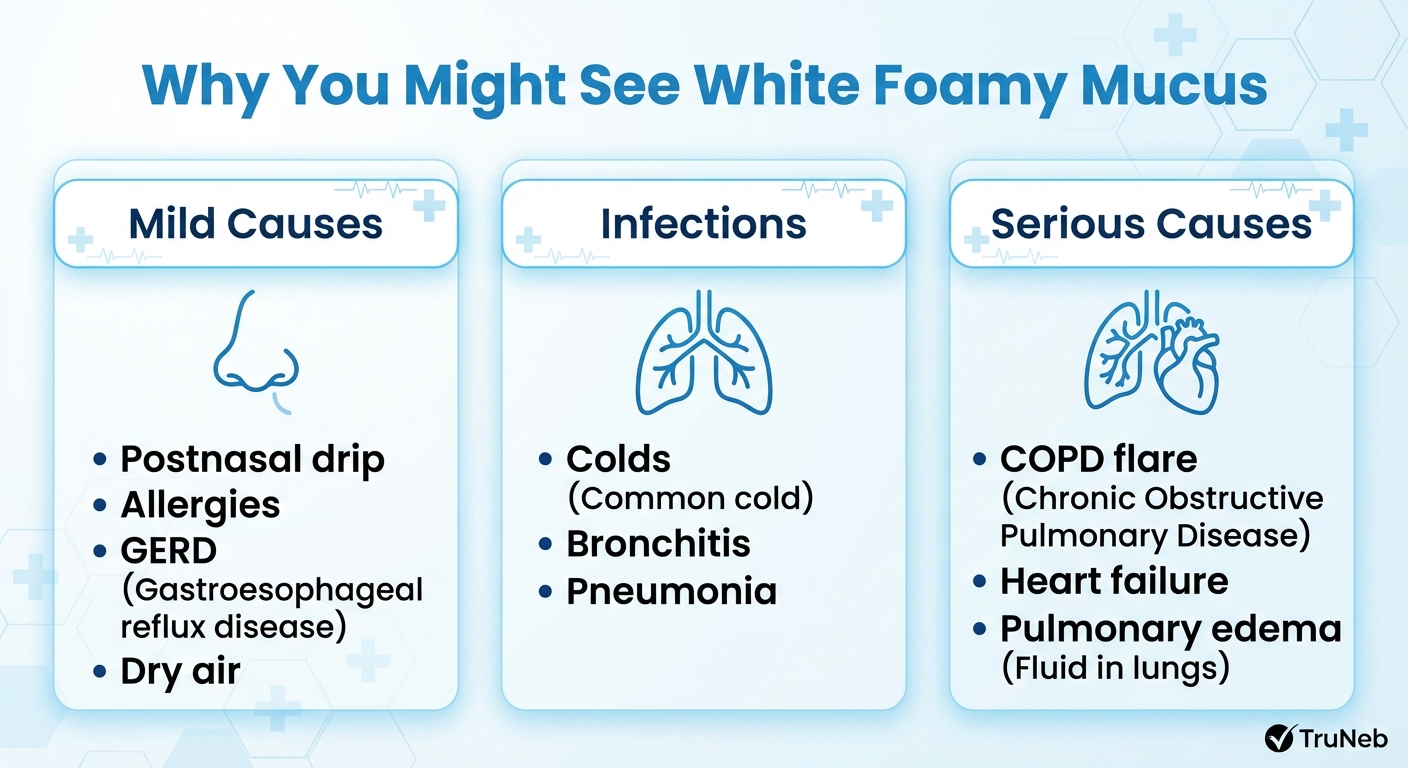
Chronic Lung Diseases Like COPD and Asthma
Chronic lung diseases often cause a thick white mucus cough that shows up day after day. Over time, this mucus can look frothy when you bring it up.
In COPD and chronic bronchitis, the airways stay swollen and irritated. The lining makes too much mucus, and the tiny hairs that normally move it out don’t work well. If you have COPD, you might notice:
- Daily morning cough with white or clear sputum
- More mucus with cold air, infections, or smoke
- A sudden change to thicker, yellow, or green mucus during a flare
Asthma also inflames the airways, but symptoms tend to come and go. During an asthma attack, the muscles around your airways tighten and extra mucus forms. You might wheeze, feel chest tightness, and cough up sticky, sometimes foamy, white mucus as your body tries to clear the blockage.
Bronchiectasis is another condition where airways are permanently widened and scarred. Mucus pools in these pockets and can become very thick. Coughing through large amounts of trapped mucus often makes it look bubbly or foamy.
If your usual cough suddenly changes—more mucus, a different color, or more shortness of breath—let your doctor know.
One-line: In COPD, asthma, and bronchiectasis, long-term airway damage and swelling lead to thick white mucus that can look foamy when you cough it up.
Dangerous Causes: Fluid in the Lungs and Heart Problems
Key point: Pink, frothy mucus with sudden breathing trouble is an emergency sign of possible fluid in the lungs.
Sometimes white foamy mucus is a sign that fluid is leaking into the air spaces of your lungs. When that fluid mixes with air and mucus, it creates frothy sputum that can be white or pink.
Pulmonary edema is the medical term for fluid in the lungs. The most common cause is sudden heart failure, when the heart can’t pump blood forward well enough. Pressure backs up into the lung blood vessels, and fluid seeps into the air sacs.
Clear warning signs can include:
- Sudden, severe shortness of breath
- Feeling like you’re drowning or can’t lie flat
- Fast heartbeat and anxiety
- Coughing up white or pink, foamy mucus
- Swelling in the legs or ankles
Serious infections such as severe pneumonia or a condition called acute respiratory distress syndrome (ARDS) can also flood the lungs with fluid. In these cases, people usually breathe very fast, need high levels of oxygen, and may become confused.
Any time white foamy mucus shows up with big changes in breathing, chest pain, or pink or blood-tinged foam, treat it like an emergency and get help right away.
If you suddenly feel like you can’t catch your breath, have chest pain, or cough up pink, frothy mucus, call 911 or go to the nearest emergency room right away.
One-line: White or pink frothy mucus combined with sudden shortness of breath or chest discomfort can signal dangerous fluid build-up in the lungs from heart or lung failure.
How Doctors Figure Out the Cause of White Foamy Mucus
When you see a doctor about white foamy mucus, they start with simple questions: how long it’s lasted, how much mucus you’re bringing up, what color it is, and what other symptoms you have, like fever, wheezing, chest pain, or weight loss.
They’ll listen to your lungs, check your heart, and measure your oxygen level with a fingertip sensor. These steps alone can usually tell the difference between a mild infection, a COPD or asthma flare, and a possible emergency.
Depending on what they find, your doctor might order:
- A chest X-ray to look for pneumonia or patterns that suggest fluid in the lungs
- Blood tests to check for infection or heart strain
- A sputum sample to look for bacteria or other germs
- Breathing tests (spirometry) to check for asthma or COPD
- An ultrasound of the heart (echocardiogram) if heart failure is suspected
These tests help match your symptoms and your white foamy mucus to a clear diagnosis so treatment can be tailored to you.
If your symptoms don’t start to improve after about a week, or if they keep getting worse, talk with your doctor.
One-line: Doctors combine your story, an exam, imaging, and sometimes sputum and breathing tests to pinpoint why you’re coughing up white foamy mucus.
Home Care and Over-the-Counter Options
For most mild cases, white foamy mucus treatment starts with simple steps you can take at home.
Drinking plenty of fluids, especially warm drinks, keeps mucus thinner so it moves out more easily. Using a cool-mist humidifier or taking a steamy shower adds moisture to the air and can calm irritated airways.
Saline nasal sprays or gentle rinses can wash out allergens and extra mucus from your nose and sinuses, easing postnasal drip. Propping your head up on an extra pillow at night can reduce the feeling of mucus pooling in your throat when you lie flat.
Over-the-counter expectorants that contain guaifenesin can help thin thick white mucus so it’s easier to cough up. Non-drowsy antihistamines might help if allergies are the trigger. Nasal decongestant sprays can open a very stuffy nose, but these sprays are meant only for short-term use. Using them for too long can actually make congestion worse, so check the package directions or ask your doctor or pharmacist how to use them safely.
You might see boxes labeled “steam inhaler” in the same aisle. These are for warm mist only and aren’t meant for breathing prescription medications.
Talk to your doctor before trying a new medication, even if it’s sold over the counter, especially if you have heart disease, high blood pressure, or are on other daily medicines.
One-line: Hydration, humidified air, saline rinses, and carefully chosen over-the-counter medicines can ease white foamy mucus when symptoms are mild.
Quick comparison: Home remedies vs over-the-counter options
| Option | Main effect | Best for | Key caution |
|---|---|---|---|
| Fluids & warm drinks | Thin mucus | Most mild mucus symptoms | Ask your doctor about limits if you have heart or kidney problems |
| Humidifier or steamy shower | Moisten airways | Dry air, irritated throat | Keep devices clean to avoid mold or germs |
| Saline nasal sprays/rinses | Rinse nose and sinuses | Postnasal drip, allergies | Use clean water and follow product instructions |
| Expectorants (guaifenesin) | Thin thick mucus | Chest congestion with thick phlegm | Check interactions with other medicines |
| Antihistamines | Calm allergy response | Allergy-related symptoms | Some types can cause drowsiness or dry mouth |
| Nasal decongestant sprays | Shrink swollen nasal tissue | Very stuffy nose | Short-term use only, ask a doctor or pharmacist if unsure |
Prescription Treatments, Nebulizers, and TruNeb Portable Mesh Nebulizer
When white foamy mucus comes from asthma, COPD, bronchiectasis, or other chronic lung problems, your doctor might prescribe inhaled medicines to calm swelling and help clear mucus.
Inhaled corticosteroids reduce airway inflammation over time. Long-acting bronchodilators relax the muscles around your airways so air can move more freely past thick mucus. Some people also use mucolytic medicines that thin very sticky mucus.
Nebulized treatments turn liquid medicine into a fine mist you can breathe deep into your lungs. For some patients, doctors prescribe nebulized hypertonic saline (3% or 7% salt solution) to draw water into the airways and loosen thick mucus so it’s easier to cough out.
A portable mesh nebulizer like TruNeb™ can make this kind of treatment easier to fit into daily life. Mesh nebulizers are small, quiet devices that use a vibrating mesh to create a fine mist, so you can take treatments at home or on the go without a bulky compressor. For some people, that convenience makes it easier to keep up with their airway-clearance routine.
Use nebulized medicines and hypertonic saline only under a doctor’s guidance, since they can sometimes tighten sensitive airways or interact with other treatments.
One-line: For chronic lung conditions, prescribed inhalers, mucus-thinning medicines, and portable mesh nebulizers such as TruNeb can all be part of a long-term white foamy mucus management plan.
Simple Guide: Watch at Home, Call Your Doctor, or Go to the ER
Key point: How you feel matters more than how the mucus looks. Breathing trouble, chest pain, or pink foam are a reason to get urgent care.
This plain guide can help you decide what to do next, but it doesn’t replace medical advice.
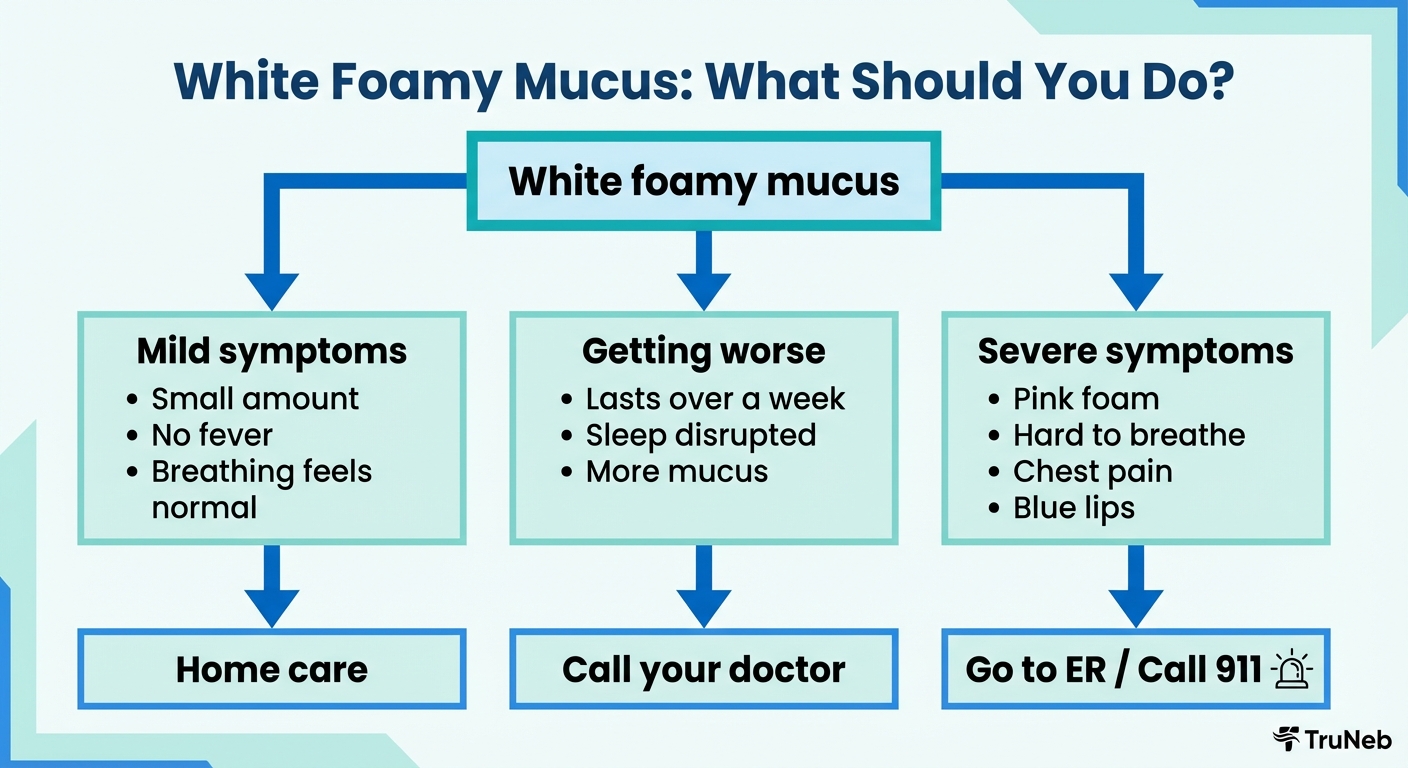
- Usually Safe To Watch At HomeYou have a small amount of white foamy mucus, feel mostly okay, can breathe normally, and either have a mild cold, allergy symptoms, or known reflux. You don’t have chest pain, high fever, or leg swelling. In this situation, lots of people manage symptoms at home and keep a close eye on how they feel.
- Call Your Doctor SoonYour white foamy mucus lasts more than a week, your cough is getting in the way of sleep or work, or you have a history of asthma, COPD, or heart disease and notice more mucus or more shortness of breath than usual. It’s a good idea to arrange a clinic visit within a day or two.
- Go To The ER Or Call 911 NowYou have sudden severe trouble breathing, chest pain or tightness, fast heartbeat, confusion, blue lips or fingers, or you’re coughing up large amounts of pink or blood-tinged foam. These are emergency signs of possible fluid in the lungs, a blood clot, a major infection, or heart failure.
If you’re ever unsure where you fit, it’s safer to call your doctor’s office or an urgent care line and ask.
One-line: Small, improving amounts of white foamy mucus can be watched, but fast-worsening symptoms or pink froth are a reason to get urgent care.
Frequently Asked Questions About White Foamy Mucus
Tap or click a question below to see the answer:
No. White foamy mucus can come from infections, but it can also be caused by allergies, postnasal drip, acid reflux, or chronic lung diseases like asthma and COPD. Your other symptoms and how you feel overall give the best clues.
Pink, red, or rust-colored foam is more serious. It can mean blood is mixing with fluid in your lungs. If you see pink foamy mucus along with shortness of breath, chest pain, fast heartbeat, or feeling faint, seek emergency care right away.
If you feel well otherwise, mild white foamy mucus from a cold or allergies usually settles within one to two weeks. If it lasts longer than about three weeks, keeps getting worse, or comes with fever, night sweats, weight loss, or chest pain, you should book a visit with a doctor.
Anxiety and panic attacks can make you breathe faster and cough more, which can bring up mucus that was already in your airways. Anxiety itself doesn’t usually create new mucus, but it can uncover problems like reflux or asthma that do.
Nebulizers are tools, not treatments by themselves. The safety depends on what medicine or solution you put in them. Hypertonic saline and other nebulized medicines can help some people clear mucus, but they can irritate others. Always talk with your doctor or clinician before starting, stopping, or changing any nebulized treatment.
One-line: These quick answers explain when white foamy mucus is harmless and when it’s a sign to get medical help.
Disclaimer: This article is for informational purposes only and doesn’t replace professional medical advice. Always talk with your doctor about your symptoms, questions, or before changing any treatment.






