On this page
Wheezing that shows up or gets worse when you lie down is a clue, not a diagnosis. It usually means something is narrowing your airways or making it harder for your lungs to work when your body is flat.
Wheezing that shows up or gets worse when you lie down is a clue, not a diagnosis. It usually means something is narrowing your airways or making it harder for your lungs to work when your body is flat.
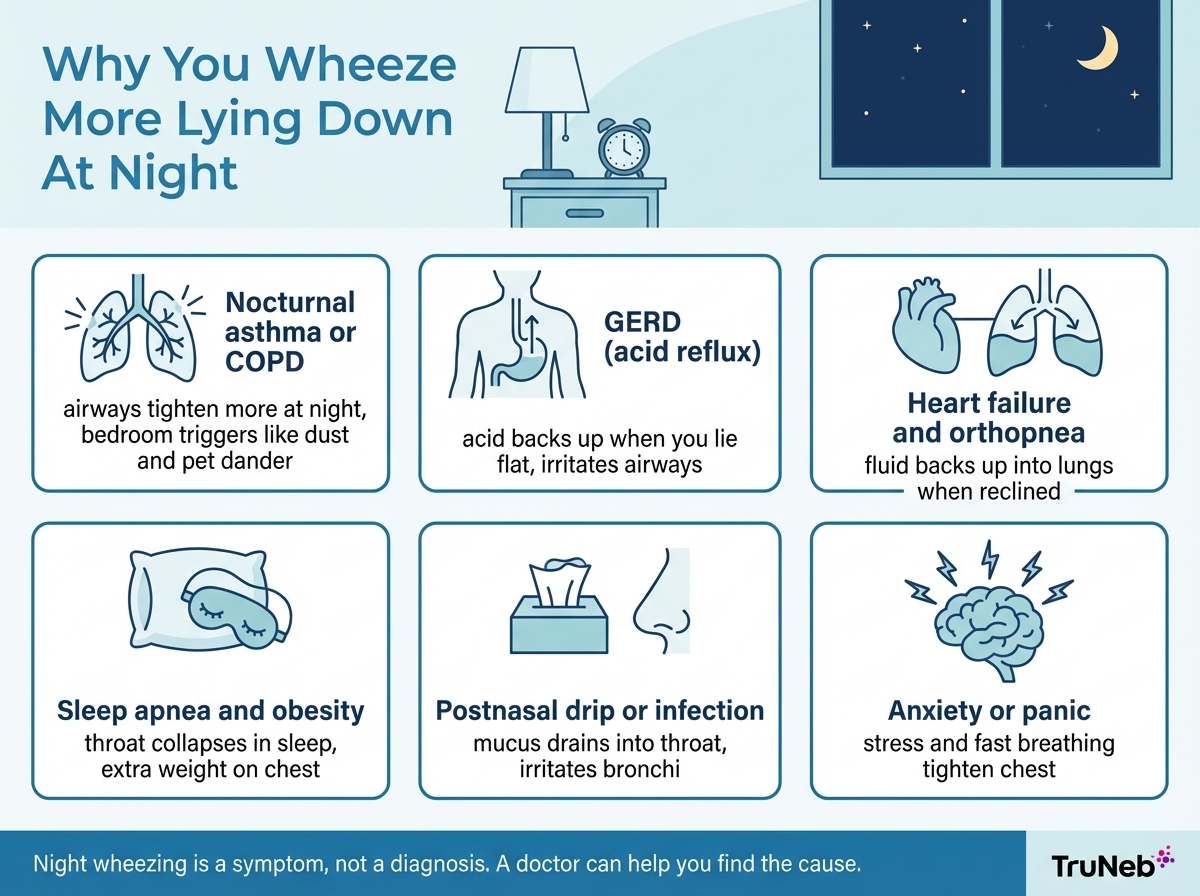
When you recline, gravity shifts. Blood, fluid, and mucus move differently through your chest. For some people, that shift exposes a problem like asthma, heart failure, or acid reflux. For others, it’s more about weight on the chest, postnasal drip, or anxiety.
Wheezing that starts or clearly worsens when you lie down is called positional or nocturnal wheezing and can come from lung, heart, reflux, sleep apnea, or anxiety-related causes.
In this guide, you’ll see how to connect your pattern of symptoms to likely causes, what you can safely do at home, how devices like inhalers and nebulizers fit in, and when night wheezing crosses the line into an emergency.
Wheezing that starts or gets worse when you lie down is a sign that something is affecting your breathing at night, and it’s worth figuring out the cause with your doctor.
Talk to your doctor before trying a new medication or changing how you use your inhaler or nebulizer.
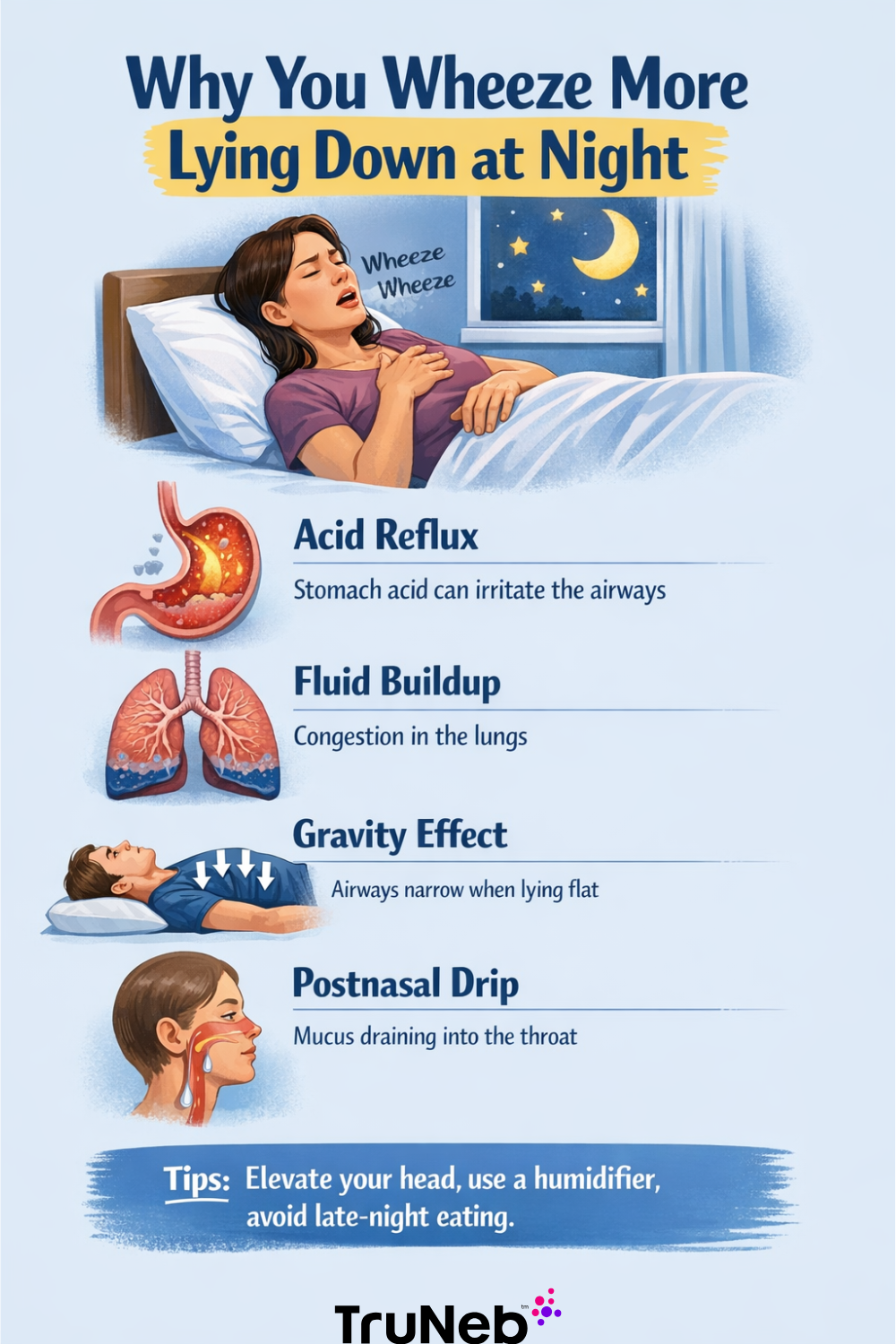
Asthma and COPD are two of the most common reasons for wheezing when you lie down.
In asthma, the small airways spasm and swell. In COPD, the airways are damaged and partly blocked over time. In both, air has trouble getting out of the lungs, which creates that high-pitched whistling sound, especially on exhale.
Symptoms usually flare at night. Cooler air, lying flat, hormone changes, and bedroom triggers like dust mites or pet dander all make nocturnal wheezing more likely.
What it feels like
- Wheezing louder when you breathe out than when you breathe in
- Tight, heavy feeling in your chest
- Cough that wakes you up, sometimes dry or with a bit of mucus
- Needing extra pillows or preferring to sleep slightly upright
People with COPD report this a lot. More than three out of four say breathing gets harder once they get into bed, and a number of them end up sleeping in a recliner instead of flat.
What you can do
- Follow your asthma or COPD action plan exactly as your doctor recommends.
- Use your preventive (controller) inhaler at the time your doctor recommends, which for some people with nocturnal asthma is in the evening.
- Keep your quick-relief inhaler by your bed so you can use it right away if you wake up wheezing, following your doctor’s instructions.
- Raise your head and upper chest with extra pillows or an adjustable bed so your lungs can expand more easily and mucus can drain down instead of pooling.
- Make your bedroom a low-trigger zone: no smoking, less dust, fewer pets on the bed, and good airflow.
Night wheezing from asthma or COPD should steadily ease after you use your rescue medication as directed. If it does not, or if you need your rescue inhaler most nights, your long-term treatment likely needs to change and you should talk with your doctor.
One-line takeaway: Asthma and COPD often show up as wheezing on exhale when you lie down, and needing frequent rescue medication at night is a sign your condition is not well controlled.
Talk to your doctor before trying a new medication or changing how often you use your inhalers.
Gastroesophageal reflux disease (GERD) is long-term acid reflux. It doesn’t just cause heartburn. In some people it also triggers coughing and wheezing, especially when they lie down.
When you recline on a full stomach, acid can wash up from your stomach into your esophagus and even reach your throat. That acid irritates nearby airways and can cause them to spasm. If you already have asthma, reflux can set off an attack.
Typical clues
- Wheezing that starts or gets worse after a meal or late-night snack
- Burning in the chest (heartburn) or sour taste in your mouth
- Nighttime cough, hoarse voice, or feeling like there is a lump in your throat
- Symptoms that ease when you sit or stand up, or after you take an antacid
How to calm GERD-related wheezing at night
- Stop eating 2–3 hours before lying down so your stomach is emptier.
- Skip trigger foods and drinks in the evening like spicy meals, fatty foods, chocolate, citrus, caffeine, and alcohol.
- Raise the head of your bed by about 6–8 inches using blocks or a wedge pillow so gravity keeps acid in your stomach.
- Aim for a healthy weight and avoid tight waistbands at night, which can push acid upward.
- Ask your doctor if an over-the-counter acid reducer is appropriate for you, and follow their directions closely.
Fixing reflux usually improves both heartburn and nighttime wheezing. If you’re using asthma medicine correctly but still wheeze when lying down after meals, GERD is worth looking at with your doctor.
One-line takeaway: GERD wheezing at night usually comes with heartburn and coughing after you lie down, and better reflux control usually eases the breathing issues too.
Talk to your doctor before starting or changing any acid-reducing medication.
Not all wheezing is from the lungs themselves. In heart failure, a weak heart struggles to pump blood forward. When you lie flat, more blood returns to the chest, pressure rises in the lung blood vessels, and fluid can leak into the air spaces.
This makes breathing feel tight or heavy and can cause a wet kind of wheeze, sometimes called cardiac wheezing. Doctors use the word orthopnea for shortness of breath that clearly gets worse when you lie down and better when you sit or stand up.
How it tends to look
- You need several pillows or a recliner just to sleep without gasping
- Your legs, ankles, or feet are swollen by the end of the day
- You wake up at night coughing or feeling like you’re drowning
- Your cough may produce frothy or pink-tinged mucus
- You feel unusually tired or have gained weight quickly from fluid
Why this is serious
Orthopnea wheezing points to fluid in the lungs, not just narrow airways. It usually means the heart is under real strain. Trying to self-treat this at home with inhalers alone is not safe.
What helps in the moment
- Sit upright right away when you feel breathless lying down.
- Keep your upper body elevated to sleep until you see a doctor.
- Limit very salty meals and heavy late dinners, which can worsen fluid retention.
You will still need medical care. Doctors may use diuretics (water pills) and other heart medicines to pull fluid off your lungs and ease breathing.
⚠️ If you ever have severe trouble breathing, chest pain, or notice blue lips or pink frothy mucus, get emergency medical help right away.
One-line takeaway: Heart failure wheezing at night almost always comes with other signs like swelling, weight gain, and needing more and more pillows to sleep, and it needs prompt medical evaluation.
If you ever cough up pink, frothy mucus, have crushing chest pressure, or cannot catch your breath even sitting up, call emergency services right away.
Obstructive sleep apnea (OSA) is another common reason for breathing noises at night. In OSA, the soft tissues in your throat relax and partly or fully block the airway over and over during sleep.
Most people think of loud snoring and gasping with sleep apnea. But some also notice a wheezy or choking sound as the airway snaps back open. In some cases, what sounds like wheezing is really air squeezing through a narrowed upper airway, not the lungs.
Obesity can make this worse. Extra weight around the neck, chest, and belly puts pressure on your airway and diaphragm when you lie down. That pressure makes each breath take more effort.
Signs that point to sleep apnea or weight-related breathing
- Loud snoring most nights
- Pauses in breathing that someone else notices
- Waking up choking, gasping, or with a racing heart
- Morning headaches, very dry mouth, or sore throat
- Daytime sleepiness even after a full night in bed
- Wheezing or feeling short of breath mostly at night, especially when supine
For some people with severe obesity, breathing can be shallow even while awake and worsens lying down. Doctors call this obesity hypoventilation syndrome.
What can help
- Ask your doctor about a sleep study if any of these signs fit you.
- If you are diagnosed with OSA, consistent use of CPAP or another device your sleep specialist prescribes can keep your airway open and usually stops the nighttime wheeze-like sounds.
- Try sleeping on your side instead of your back; this simple change can reduce airway collapse in a lot of people.
- Gradual weight loss, even a modest amount, can ease pressure on the lungs and make it easier to breathe lying down.
- Avoid sedatives and excess alcohol at night, since both relax throat muscles and make apnea worse.
One-line takeaway: Noisy, wheezy breathing only during sleep, along with snoring and daytime fatigue, commonly points to obstructive sleep apnea or obesity-related airway narrowing rather than classic asthma.
Talk to your doctor before starting any sleep apnea treatment or weight loss medication.
Sometimes the cause of wheezing when you lie down is higher up in the airway.
When you have allergies, a cold, or sinusitis, mucus can drip from the back of your nose down your throat. Lying flat makes that drip more constant. The mucus irritates your throat and bronchial tubes, which can trigger cough and a reactive wheeze, especially if you already have sensitive airways.
A chest infection like acute bronchitis or pneumonia can also make breathing worse when you recline. In those cases, the airways or lung tissue themselves are inflamed or filled with mucus or fluid.
What this tends to feel like
- Stuffy or runny nose, sinus pressure, or itchy eyes
- Frequent throat clearing, especially at night
- Cough that gets worse once you lie down
- Rattling sound or mild wheeze with each breath
- With infections: fever, chills, feeling achy or unwell, thicker yellow or green mucus, or sharp chest pain when you breathe deeply
What you can do at home
- Rinse your nose with saline or take a warm shower before bed to clear mucus.
- Use allergy medication or a nasal steroid spray if your doctor recommends it.
- Wash bedding weekly in hot water and keep pets off the bed to cut down dust and dander.
- Sleep with your head slightly raised so mucus doesn’t pool in your throat.
- Stay well hydrated to thin secretions and make them easier to clear.
If you suspect pneumonia or a more serious infection (high fever, fast breathing, chest pain, or coughing up blood-streaked mucus), see a doctor promptly. Infections that involve the lungs usually need prescription treatment.
One-line takeaway: Night wheezing that comes with a stuffy nose, drip in the throat, or a recent cold is often from postnasal drip or infection and usually improves as the congestion clears.
Talk to your doctor before using decongestants long term or combining multiple over-the-counter cold medicines.
Anxiety and panic attacks can make breathing feel tight even when your lungs are structurally normal.
At night, when the house is quiet and you finally lie down, your brain has space to worry. That stress can trigger rapid, shallow breathing. Hyperventilation changes carbon dioxide levels in your blood and can make your chest feel squeezed, your throat tight, and your breathing noisy.
In people with sensitive airways, this can lead to temporary bronchospasm and a wheeze. In others, it simply feels like they “can’t get a full breath,” even though oxygen levels are okay.
Common signs
- Sudden rush of fear or sense of doom, sometimes with no clear trigger
- Racing heartbeat, sweaty palms, shaking, or tingling in fingers and around the mouth
- Chest tightness, feeling like you can’t get enough air
- Symptoms that rise fast and then ease as you calm down
What can help in the moment
- Slow your breathing on purpose: inhale through your nose for 4 seconds, hold for 4–7 seconds, and exhale gently through pursed lips for 6–8 seconds as one example of a breathing exercise.
- Sit up and prop yourself comfortably instead of staying flat, which usually feels more reassuring.
- Relax your shoulders and jaw and focus on long, controlled exhales.
If a doctor has already checked your heart and lungs and feels your episodes are anxiety-based, work with them on a long-term plan. Therapy, lifestyle changes, and sometimes medication can make night panic far less common.
Still, it’s important not to assume wheezing is “just anxiety” until serious causes have been ruled out.
One-line takeaway: Anxiety can cause very real chest tightness and wheezing at night, but those symptoms should always be checked once to be sure an underlying lung or heart problem is not being missed.
Talk to your doctor before starting or changing any anxiety medication or supplements.
You usually can’t fix the root cause of wheezing overnight, but you can make nights easier while you and your doctor work on it.
Simple changes usually help your lungs work with gravity instead of against it.
Better positions for night breathing
- Try sleeping with your head and chest raised instead of lying perfectly flat. An adjustable bed, a wedge pillow, or a stack of firm pillows can all work.
- Plenty of people breathe more comfortably on their side rather than on their back. Side-sleeping can ease sleep apnea and reduce reflux.
- If you have COPD or heart failure, a slightly reclined position in a chair sometimes feels safest, especially during a flare.
Bedroom habits that can ease wheezing
- Keep smoke, strong fragrances, and harsh cleaning chemicals out of the bedroom.
- Wash pillowcases and sheets in hot water every week to cut dust mites and dander.
- Keep pets off the bed if you notice more symptoms when they sleep near you.
- Run a HEPA air purifier if you can, especially in older, dusty, or damp homes.
- Avoid big, heavy meals, alcohol, and smoking in the hours before bed.
Always have your prescribed rescue medications close enough to reach without getting out of bed. If you use an inhaler or nebulizer at night, keep it ready and checked so you are not scrambling to set it up during a bad episode.
One-line takeaway: The best sleep position for wheezing is usually with your upper body elevated and your body on its side, combined with a clean, low-trigger bedroom.
Talk to your doctor before making large changes to your sleeping setup if you have spine, heart, or blood pressure issues.
For asthma, COPD, and some other lung conditions, medicines you inhale are the main way to open tight airways fast and keep them from closing again.
Rescue inhalers
Short-acting bronchodilators are designed to give quick relief. If you wake up wheezing and your action plan from your doctor tells you to use your rescue inhaler, take it exactly as prescribed.
If your wheezing:
- eases within about 10–15 minutes and
- stays better for several hours,
that is a sign the medicine is doing its job.
If you need your rescue inhaler a lot at night, that is a sign your long-term control is not strong enough, not that you should simply keep increasing rescue doses on your own.
Nebulizers for night wheezing
A nebulizer turns liquid medicine into a fine mist you breathe in through a mask or mouthpiece. Some people find this easier to use during a flare, especially when they are very short of breath.
Modern portable mesh nebulizers are small and quiet, which makes them easier to use beside the bed. A device like the TruNeb™ portable mesh nebulizer can deliver bronchodilators or saline as your clinician prescribes without a loud compressor or needing a wall outlet.
For some conditions with thick mucus, clinicians may also prescribe inhaled saline.
- Isotonic saline (about 0.9%) mainly keeps airways moist.
- Hypertonic saline (3% or 7%) draws water into the mucus, thinning it so it is easier to cough up.
These solutions can help with mucus-heavy diseases like cystic fibrosis and bronchiectasis and, in some cases, chronic bronchitis, but they are not rescue medications.
How to use devices safely at night
- Follow the written asthma or COPD action plan your doctor gives you.
- Do not start hypertonic saline or change doses on your own; some people can feel more tightness if it is not used correctly.
- If your inhaler or nebulizer does not ease your wheezing, or you think you need treatments more often than your plan allows, seek medical care.
One-line takeaway: Use rescue inhalers and nebulizers for night wheezing exactly as your doctor directs, and treat frequent nighttime use as a sign to review your overall treatment plan, not as something to simply push through.
Talk to your doctor before trying hypertonic saline or changing how often you use your inhaler or nebulizer.
Quick comparison: Rescue inhalers vs nebulizers at night
| Feature | Rescue inhaler | Nebulizer (including portable mesh) |
|---|---|---|
| How it works | Pressurized spray you inhale in a quick breath | Turns liquid medicine into a mist you breathe over several minutes |
| Typical use time | Very fast, a few breaths | Longer session, usually several minutes per treatment |
| Effort needed | Requires timing a deep breath with a spray | Less timing, you breathe normally through a mask or mouthpiece |
| Nighttime convenience | Small, easy to keep on a bedside table | Portable mesh devices are compact and quiet, older compressor models can be bulkier and louder |
| Who decides which to use | Your doctor, based on your action plan | Your doctor, based on your diagnosis and prescribed medicines |

Most people with asthma, COPD, or reflux will have occasional mild night symptoms they can manage at home. But some signs mean you need urgent help.
Go to the emergency room or call 911 right away if:
- You can only speak a few words at a time because you are so short of breath.
- Your wheezing does not improve after using your rescue inhaler or nebulizer as directed.
- Your lips, face, or fingertips look blue, gray, or very pale.
- You feel faint, confused, or unusually sleepy during a breathing episode.
- You have sudden chest pain or pressure along with wheezing.
- You cough up pink, frothy mucus or any amount of blood.
- Your wheezing starts quickly after a sting, food, or medication, and you also notice swelling, hives, or vomiting.
Call your doctor soon (or book a visit) if:
- You wheeze when lying down at least a few nights each week.
- You suddenly start having night wheezing when you never did before.
- You need more pillows or must sleep upright to breathe comfortably.
- You notice ankle swelling, rapid weight gain, or ongoing heartburn with your symptoms.
- You need your rescue inhaler at night more than a couple of times a week.
One-line takeaway: Treat severe night wheezing with trouble speaking, blue lips, or no relief from medication as an emergency, and treat new or frequent night wheezing as a reason to see your doctor soon.
Talk to your doctor before changing any long-term treatment, and never delay emergency care if your breathing feels out of control.
FAQs About Wheezing When Lying Down
Tap or click a question below to see the answer:
Lying flat changes how blood, fluid, and mucus move in your chest. That shift can expose problems like asthma, GERD, heart failure, or sleep apnea that are less obvious when you are upright. It is a pattern worth discussing with your doctor so you can find the cause.
Wheezing on exhale is common in asthma and COPD because air has more trouble getting out of narrowed airways. It is not automatically more serious than wheezing on inhale, but if it is new, frequent, or wakes you at night, it should be checked by a doctor.
Yes. Acid that reaches your throat when you lie down can irritate your airways and trigger wheezing or coughing. People typically notice this after late or heavy meals or when they wake with heartburn and a cough. Better reflux control often eases the breathing issues too.
Heart-related orthopnea usually comes with needing extra pillows, ankle swelling, rapid weight gain from fluid, or waking up gasping and coughing up frothy mucus. Those are red flags for heart failure and need prompt medical care rather than home treatment alone.
Nebulized bronchodilators can help when wheezing is from narrowed airways, like in asthma or COPD. They will not fix wheezing from heart failure, reflux alone, or anxiety. A portable mesh nebulizer, such as TruNeb, can be a convenient way to take prescribed treatments at night, but only as part of a plan your clinician designs.
It is an emergency if you cannot speak in full sentences, your rescue medicine does not help, your lips or face turn blue, you feel like you might pass out, you have severe chest pain, or you cough up pink, frothy mucus or blood. In those situations, get emergency help immediately.
You can make nights easier by changing your sleep position, clearing bedroom triggers, and using medicines exactly as prescribed. But you should not try to self-manage ongoing or severe wheezing without medical input. A doctor can find and treat the cause so you can sleep and breathe more comfortably.
These common questions highlight that wheezing when you lie down is usually manageable once you know the cause and work with a doctor on a plan.
Talk to your doctor before starting, stopping, or changing any inhalers, nebulized treatments, or other medications for nighttime wheezing.