On this page

What walking pneumonia is and how it differs from typical pneumonia
Walking pneumonia is a milder form of pneumonia that can feel more like a lingering chest cold than a severe lung infection. When people talk about walking pneumonia symptoms, they usually mean a slow-building mix of cough, fatigue, and chest discomfort that doesn’t match a routine cold.
Pneumonia means there’s an infection in the tiny air sacs of your lungs, called alveoli. These air sacs normally fill with air. With pneumonia, they can fill with mucus and fluid, which makes breathing harder and can lower oxygen levels.
In a lot of cases, walking pneumonia comes from a bacterium called Mycoplasma pneumoniae. According to the CDC, this germ is a common cause of community‑acquired pneumonia, especially in school‑age kids and young adults.
Key facts about walking pneumonia
- It’s a real pneumonia infection in your lung air sacs, not “just a bad cold.”
- Symptoms build slowly and can keep you on your feet, but worn down.
- Fever can be mild or even absent.
- It spreads through close contact, especially in families and schools.
- You should call your doctor if a cough and chest discomfort drag on or breathing feels harder.
What walking pneumonia means
The word “walking” simply means you still feel well enough to be up and moving around. You might keep going to work or school, even though you have pneumonia in your lungs.
It does not describe a different disease. Walking pneumonia is still pneumonia, just with milder, more drawn‑out symptoms.
Why it is called atypical pneumonia
Doctors sometimes call walking pneumonia an “atypical” pneumonia. This doesn’t mean rare or strange. It means it doesn’t always follow the classic pattern of sudden high fever, shaking chills, and very fast breathing.
Atypical pneumonia tends to:
- Start slowly
- Cause a nagging cough and fatigue
- Come with only a low‑grade fever, or no clear fever at all
Other germs besides Mycoplasma pneumoniae can cause atypical pneumonia too, such as Chlamydophila pneumoniae and Legionella species. More “typical” community‑acquired pneumonia is often linked to bacteria like Streptococcus pneumoniae or Haemophilus influenzae.
Mini glossary
Atypical pneumonia is a milder, slower‑moving type of pneumonia that doesn’t always cause high fever or make you look extremely ill at first.
Low‑grade fever is a temperature that’s only a little higher than normal, around 99–100.3°F (37.2–37.9°C).
Productive cough means a cough that brings up mucus or phlegm from your lungs instead of staying dry.
In medical coding, Mycoplasma pneumonia can be labeled as ICD‑10 J15.7.
How it differs from regular pneumonia
Typical or “classic” pneumonia is often caused by bacteria like Streptococcus pneumoniae or Haemophilus influenzae. It tends to come on more suddenly, with higher fever, strong chills, and faster, more labored breathing. People usually feel too sick to do normal daily tasks.
Walking pneumonia usually:
- Builds over several days, sometimes after what seems like a regular cold
- Causes a stubborn, hacking cough
- Brings fatigue and chest discomfort, but not always high fever
- Shows only small, patchy changes on a chest X‑ray rather than one big white area
Doctors still take walking pneumonia seriously. In older adults, or people with asthma, COPD, heart disease, or weak immune systems, even a “mild” pneumonia can turn into something more serious if it isn’t watched closely.
Takeaway: Walking pneumonia is a milder, slower‑moving type of community‑acquired pneumonia that still infects the air sacs in your lungs, even if it feels on the surface like a lingering chest cold.
Walking pneumonia symptoms to watch for
Walking pneumonia symptoms can start out looking like a stubborn cold or mild flu, then linger longer than you expect. The first signs of walking pneumonia are easy to miss, because you might still feel well enough to keep up with daily life.
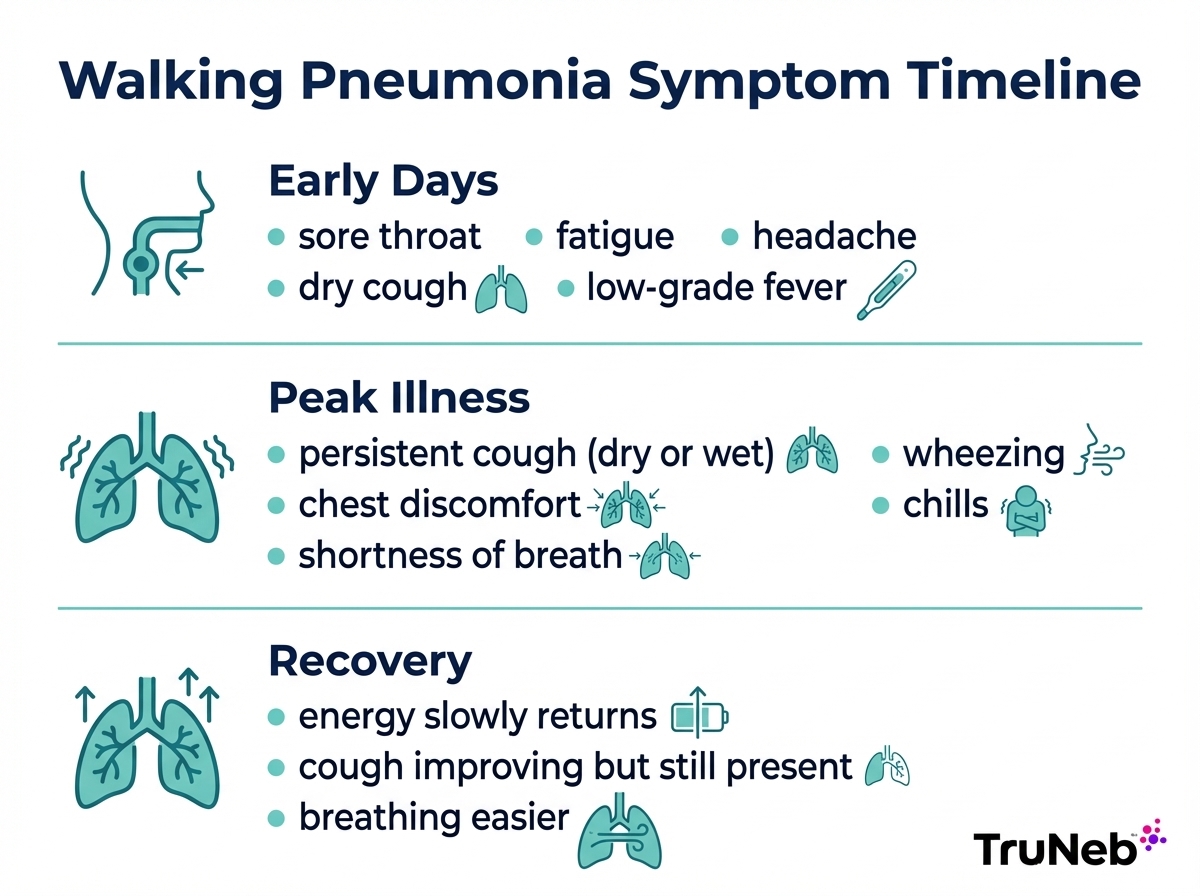
Early symptoms
These early symptoms build over several days and are easy to brush off as “just a virus”:
- Sore or scratchy throat that doesn’t settle down
- Tiredness or fatigue that feels out of proportion to a mild cold
- Headache and general achiness
- Dry or hacking cough that keeps you up at night
- Mild chest discomfort or tightness when you cough or take a deep breath
- Low‑grade fever, sometimes with light chills
- Mild ear pain or a full feeling in the ears, especially in kids
Early walking pneumonia can feel like a cold that has moved deeper into your chest and doesn’t respond to the usual rest‑and‑tea routine.
Signs the illness is getting worse
As the infection settles deeper into the lungs, symptoms can shift and intensify, even if you’re still out of bed and moving around.
Worsening signs include:
- Cough that lasts more than a week and is getting harsher or more frequent
- Cough that starts to bring up yellow, green, or rust‑colored mucus
- Stronger chest discomfort or pain when you breathe or cough
- Shortness of breath when walking across a room, climbing stairs, or talking
- Wheezing or a whistling sound when you breathe out
- Chills, sweats, or feeling feverish even with only a low‑grade fever
A cough that hangs on and slowly worsens, especially with shortness of breath or chest pain, is a common reason doctors check for walking pneumonia or other lung problems.
Can walking pneumonia happen without fever?
Yes. Walking pneumonia can show up with a mild fever or no clear fever at all. Older adults and people who take certain medicines sometimes never see the thermometer climb, even when they have a real lung infection.
Because of that, doctors look at the full picture: how long the cough has lasted, how your chest feels, whether you’re short of breath, how run‑down you feel, and whether the cough is disturbing sleep.
People who ask “what does walking pneumonia feel like” usually describe a nagging, chest‑based cough, tight or sore breathing, and deep fatigue that stretches far beyond a standard cold.
A “cold” that isn’t improving after 10–14 days, or a cough that keeps you up at night for weeks, is a common reason doctors evaluate for walking pneumonia or other breathing problems.
Takeaway: A cough that outlasts a normal cold, especially with chest discomfort, fatigue, or shortness of breath and little or no fever, is a common warning sign of walking pneumonia.
Walking pneumonia symptoms in adults and children
Adults and kids can both get walking pneumonia, but they don’t always look the same. When people talk about walking pneumonia in adults vs kids, adults usually describe a nagging chest cold, while children can just seem extra tired, fussy, or “off.”
Common symptoms in adults
Adults with walking pneumonia usually describe a slow, nagging illness rather than a sudden crash. A dry or hacking cough is one of the main symptoms. It can start mild and then hang on, sometimes keeping you up at night.
Adults commonly notice a sore throat at the beginning, headache, low‑grade fever, chills, and feeling wiped out. Chest discomfort is common. You might feel tightness or a heavy feeling in your chest, or a sharp twinge when you cough or take a deep breath.
Shortness of breath can show up when you climb stairs, walk farther than usual, or talk a lot. People with asthma or COPD sometimes notice that their usual inhalers don’t seem to help as much.
A helpful rule of thumb: in adults, symptoms feel like a chest cold that overstays its welcome, especially when the cough lasts longer than 7 to 10 days.
Common symptoms in children
School‑age children and teens often have symptoms similar to adults: a long‑lasting cough, mild fever, sore throat, and fatigue. They might complain that their chest hurts when they cough or run in gym class, but still try to stay active.
Younger children, though, might not describe chest pain at all. Instead, you can see:
- Runny nose and nasal congestion
- Watery or red eyes
- Wheezing or noisy breathing
- Poor appetite or refusing to feed
- Vomiting or diarrhea
- Being more irritable, clingy, or low‑energy than usual
Because of this, walking pneumonia in toddlers can look more like a cold or a stomach bug than a classic chest infection, which makes it easy to miss at first.
Child breathing warning signs parents should not miss
In babies and younger kids, how they breathe tells you more than what they can say. Warning signs include:
- Fast, shallow breathing
- Nostrils that flare with each breath
- Skin or ribs pulling in between or under the ribs (rib retractions)
- Grunting noises with each breath
- Pauses in breathing or very irregular breathing
Other red flags are a child who can’t drink or breastfeed well, has very few wet diapers, seems floppy or unusually sleepy, or has blue or gray color around the lips or fingertips.
If you notice these breathing changes, don’t wait to see if things improve on their own. Call your child’s doctor or seek urgent care right away.
Takeaway: Adults usually describe walking pneumonia as a nagging chest cold, while children tend to show wheezing, runny nose, watery eyes, or stomach upset, so watching their breathing and energy is more helpful than waiting for them to say “my chest hurts.”
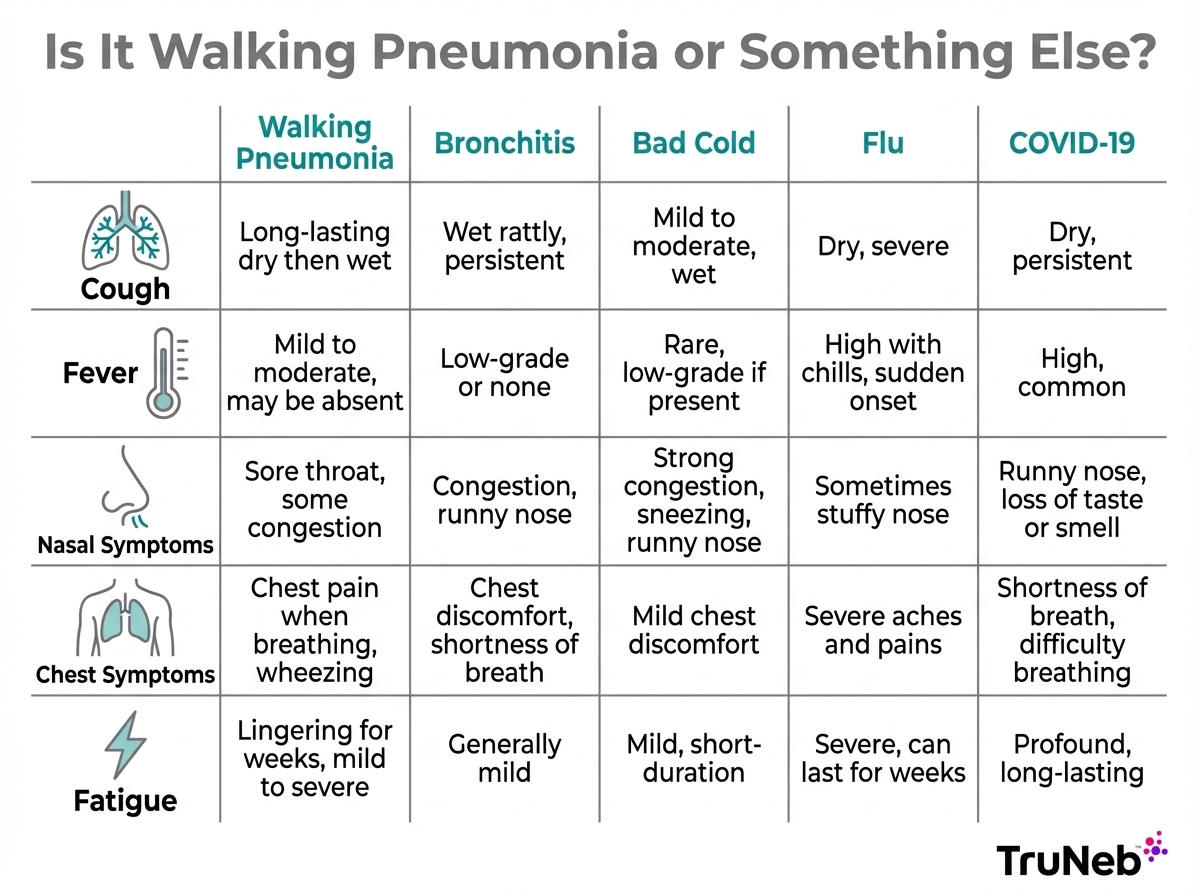
Walking pneumonia vs bronchitis, a bad cold, flu, and COVID
Walking pneumonia can masquerade as bronchitis, a stubborn chest cold, flu, RSV, or COVID‑19. The main differences come from where the infection sits in your airways and how your cough, fever, and energy change over time when you compare walking pneumonia vs bronchitis or other illnesses.
How the cough and chest symptoms differ
With walking pneumonia, the infection is in the air sacs (alveoli) of the lungs. The cough usually starts dry and hacking, then can become more productive as mucus builds. Chest discomfort, tightness, or pain with deep breaths are common, and you can feel short of breath when you move around.
Bronchitis mainly affects the bronchial tubes, the larger airways. It typically causes a loud, wet‑sounding cough with more mucus and wheezing, but less trouble getting enough air at rest. A chest cold vs walking pneumonia comparison often shows that a regular chest cold brings stronger runny nose and congestion first, with chest symptoms that are milder and shorter. To learn more about how these conditions overlap, you can explore the difference between bronchitis and pneumonia.
The flu tends to come with higher fever, stronger body aches, and a sudden, heavy hit of fatigue. COVID‑19 can look like any of these, but loss of taste or smell, more pronounced shortness of breath, and a clear exposure are important clues. RSV in kids can bring lots of congestion, wheezing, and fast breathing.
Signs it may be more than a cold
A simple cold usually peaks within a few days, then starts to improve. Nasal congestion, sore throat, and a mild cough fade over a week or so.
With walking pneumonia, nasal symptoms can be light or absent, but the chest cough and fatigue linger or worsen. Clues that it’s more than a cold include:
- A cough that lasts more than two weeks
- Feeling winded with light activity, like talking or walking across a room
- New or growing chest discomfort
- Fever that appears several days after you first felt sick
When these patterns show up, doctors start to think about walking pneumonia, bronchitis, flu, COVID‑19, RSV, or another lower‑airway infection. If you also live with asthma, it can be helpful to review how clinicians tell asthma from pneumonia in practice.
When symptoms overlap
Symptoms from walking pneumonia, bronchitis, influenza, RSV, asthma flares, COPD flares, and COVID‑19 can blur together. Some people even have more than one problem at the same time, such as pneumonia on top of chronic bronchitis or asthma.
You can use the comparison table below as a quick snapshot, but it’s not a substitute for a medical exam. There’s no perfect way to diagnose yourself at home, and chest infections can change quickly.
If you’re not improving, or you live with lung or heart conditions like asthma or COPD, a doctor visit is the safest way to sort out what’s going on. You may also find it helpful to read about how long pneumonia is contagious if you are worried about family members.
Takeaway: A cold that fades in a week is common, but a deep, lingering cough with chest discomfort and growing fatigue points more toward walking pneumonia than a simple chest cold or routine bronchitis, especially when symptoms drag on for weeks.
| Condition | Cough | Fever | Nasal symptoms | Chest or breathing | When to seek care |
|---|---|---|---|---|---|
| Walking pneumonia | Dry or mixed dry/wet, lasts for weeks | Low-grade or none | Mild or absent | Deep ache, tightness, shortness of breath with activity | Call a doctor if cough lasts longer than a week or breathing feels harder. |
| Bronchitis | Wet, rattly, lots of mucus | Low to moderate | Typically starts after a head cold | Chest tightness and wheeze | Call a doctor if cough is severe, you wheeze, or symptoms last more than three weeks. |
| Chest cold (bad cold) | Mild to moderate, throat-based | Rare and usually low | Prominent runny nose and congestion | Little or no chest pain | Home care is usually fine; see a doctor if symptoms are severe or not improving after about 10 days. |
| Flu | Dry or wet, starts suddenly | High with chills | Can include congestion | Chest pain from harsh coughing | Call a doctor if you are high risk or breathing is hard. |
| COVID-19 | Dry or wet, variable | Low, high, or none | Sore throat or congestion can appear | Shortness of breath can be more obvious | Seek urgent care for trouble breathing or chest pain. |
| RSV (more common in kids) | Wet cough with wheeze | Low to moderate | Heavy congestion and runny nose | Fast breathing, rib retractions in babies | Go to the ER if breathing looks hard, lips look blue, or feeding is poor. |
When to call a doctor and when to go to the ER
Chest infections can change quickly. Knowing when to seek help is just as important as knowing the name of the illness.
Signs you should contact a doctor soon
Call your doctor or schedule a visit if:
- Your cough is still going strong after 10–14 days.
- A low‑grade fever lasts more than three days.
- Chest discomfort makes deep breathing uncomfortable.
- You feel more short of breath with normal activity.
- Your energy keeps dropping instead of improving.
You should also reach out if you live with asthma, COPD, heart disease, diabetes, are pregnant, or have a weak immune system. These issues raise the risk that walking pneumonia, bronchitis, flu, or COVID‑19 will hit you harder. If you’re unsure whether symptoms are from asthma or infection, this guide to how to tell asthma from pneumonia can be a useful reference to discuss with your clinician.
Emergency warning signs in adults
Go to the emergency room or call emergency services if:
- Breathing is hard, fast, or very uncomfortable, even at rest
- You can’t speak full sentences without gasping
- You notice blue or gray color around your lips or face
- Chest pain or pressure feels heavy, crushing, or like a sharp stab with each breath
- You feel confused, very drowsy, or have trouble staying awake
- You cough up blood
These signs can point to a serious pneumonia, a blood clot in the lungs, a heart problem, or another emergency that shouldn’t wait for a clinic visit.
Emergency warning signs in babies and children
In babies and children, watch their breathing first. Red flags include:
- Fast or labored breathing
- Nostrils that flare with each breath
- Skin pulling in between or under the ribs (rib retractions)
- Grunting with each breath
- Pauses in breathing
You should seek emergency care if a child is very sleepy or hard to wake, seems floppy or unusually quiet, can’t drink or breastfeed, has very few wet diapers, or has blue or gray color around the lips or fingertips.
⚠️ Call 911 or your local emergency number right away if breathing is very hard or fast, lips or face look blue or gray, or someone seems confused, difficult to wake, or unable to speak in full sentences.
When in doubt, call your doctor or an after‑hours nurse line for guidance rather than waiting at home.
Takeaway: If breathing looks or feels harder, chest pain is sharp or heavy, or an adult or child shows blue lips, confusion, or rib retractions, focus less on the label and more on getting urgent medical care right away.
How walking pneumonia is diagnosed
Doctors diagnose walking pneumonia by putting your story, physical exam, and sometimes tests together rather than relying on one single test.
What a clinician looks for
Your doctor will ask when your symptoms started, how they’ve changed, and what makes them better or worse. You’ll likely be asked about contact with sick people at home, school, work, or during travel.
They listen to your lungs with a stethoscope, a step called auscultation. They’re listening for crackles, wheezes, or areas where breath sounds are quieter than they should be. They also check your temperature, heart rate, breathing rate, and oxygen level.
When a chest X-ray or swab may be used
If your symptoms, exam, or risk factors suggest pneumonia, your doctor might order a chest X‑ray. With walking pneumonia, the X‑ray can show patchy or subtle areas of infection rather than one big solid white area.
In some situations, they use nasal or throat swabs to look for Mycoplasma pneumoniae or other germs. These tests can be single PCR swabs or part of a larger respiratory pathogen panel that checks for several viruses and bacteria at once.
If you’re coughing up mucus, a sputum sample — mucus from your lungs (sputum) that you cough into a cup — can be sent to the lab, especially if you’re very sick, have been in the hospital, or aren’t getting better with usual treatment.
Why testing is not always straightforward
A normal chest X‑ray or a negative swab doesn’t always rule out walking pneumonia. Early in the illness, changes can be subtle, and lab tests aren’t perfect.
Walking pneumonia is frequently a clinical diagnosis, which means doctors rely on your symptoms, how long they’ve lasted, your exposure history, and the lung exam first, then add tests when results are likely to change the plan.
Because of that, a normal test result never replaces how you feel. If you’re not improving or you’re getting worse, it’s important to go back and be rechecked.
Takeaway: There’s no single test that always proves walking pneumonia, so doctors depend on your story and lung exam first and use X‑rays or swabs as added tools when needed.
Walking pneumonia treatment and recovery
Treatment for walking pneumonia focuses on clearing a bacterial infection when needed and easing cough, chest discomfort, and fatigue while your lungs heal.
When antibiotics may help
If your doctor suspects a bacterial cause such as Mycoplasma pneumoniae, they might prescribe an antibiotic. Common choices include macrolides such as azithromycin or clarithromycin, or doxycycline in some older children and adults.
These medicines target certain atypical bacteria but don’t treat viruses like influenza, RSV, or COVID‑19. That’s why antibiotics aren’t used for every cough or chest cold.
Doctors choose antibiotics based on your age, allergies, other conditions, and local resistance patterns, and they aren’t needed for every case of walking pneumonia.
Never start, stop, or change prescription antibiotics on your own. Talk with your doctor about what’s right for you.
Home care that can ease cough and chest discomfort
Supportive care is just as important as any prescription.
Rest helps your body fight infection. Try to protect your sleep and avoid heavy exercise while you’re still short of breath or coughing a lot.
Hydration thins mucus so it can move out of your lungs more easily. Water, broths, and electrolyte drinks all help if your stomach allows.
A cool‑mist humidifier or warm shower can loosen mucus and calm a dry, hacking cough. Keeping the air slightly moist can also ease chest tightness. If congestion is a major issue, your clinician may also talk with you about options like nebulizers for congestion relief.
For fever and pain, your doctor might suggest medicines such as acetaminophen or ibuprofen. Follow dosing instructions carefully, and ask your child’s doctor before giving any medication to infants or young children.
If you have asthma or COPD, using your prescribed inhalers as directed during an illness can help keep your airways open. Ask your doctor how they want you to use inhalers or other breathing treatments when you’re sick.
Gentle airway‑clearance positions, sitting more upright, and slow, controlled coughing can also help move mucus.
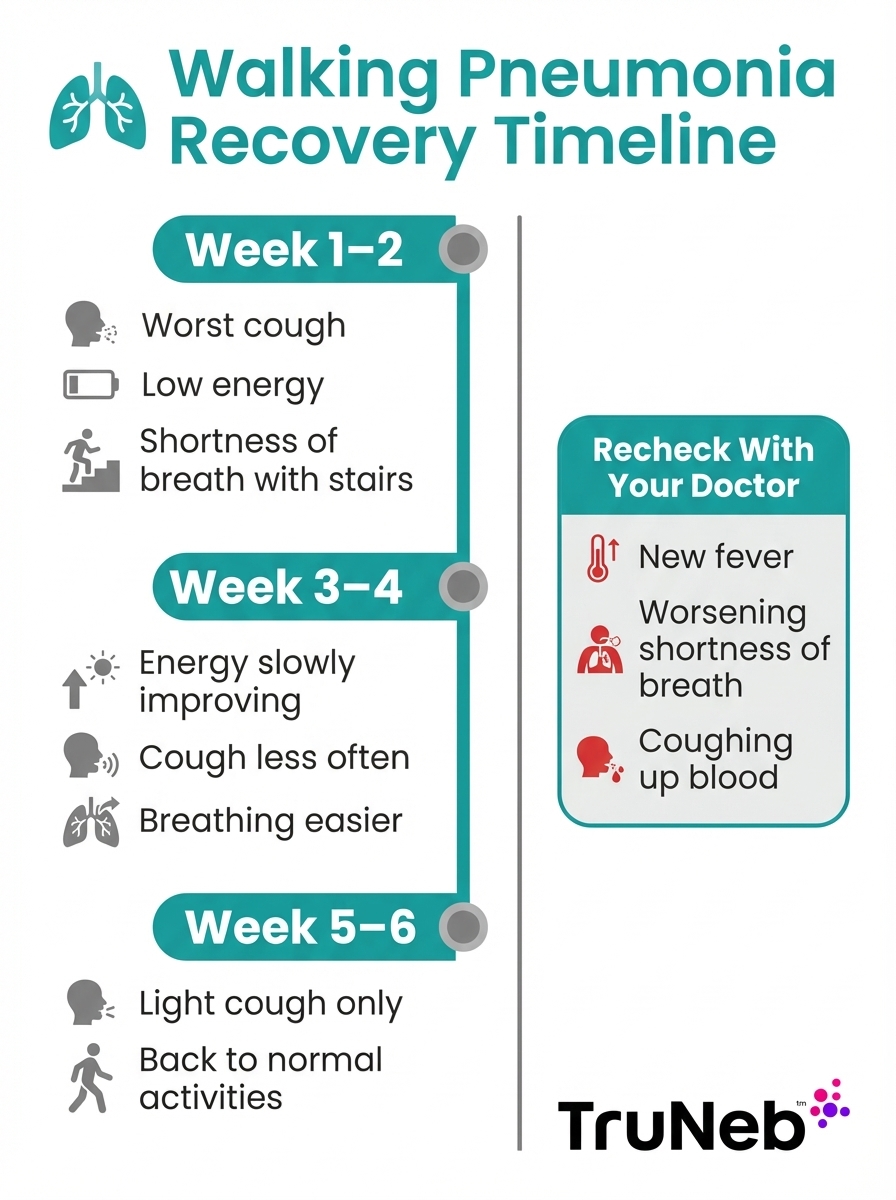
What recovery usually looks like
Most people with walking pneumonia start to feel better in one to two weeks, especially once the right treatment is in place. Energy slowly returns, and fever and chills fade.
The cough, though, tends to linger. A walking pneumonia cough can last several weeks, sometimes up to six weeks or more, even as you feel better overall. This happens because the airways stay irritated and need time to heal.
You should call your doctor again if your fever returns after going away, your cough suddenly worsens, your phlegm becomes much thicker or blood‑streaked, or your breathing becomes more difficult instead of easier. In some cases, doctors may suggest additional therapies such as using a nebulizer for pneumonia support when symptoms are slow to resolve.
Note: A cough that slowly improves over weeks, while your energy and breathing get better, usually fits normal recovery from walking pneumonia. A cough that’s getting harsher or paired with new fever or shortness of breath should always be rechecked.
How TruNeb may fit into clinician-guided mucus relief
For some people, the hardest part of recovery is thick mucus and chest congestion, especially if they already live with asthma, COPD, or another chronic lung condition.
In these situations, some doctors recommend a portable mesh nebulizer and saline treatments, such as 3% or 7% hypertonic saline, to help thin secretions and support mucus clearance. A device like the TruNeb™ Portable Mesh Nebulizer is one example of a handheld nebulizer that delivers saline or prescribed medications as a fine mist.
This type of therapy can sometimes help make coughing more productive and help some people feel like breathing is easier, but it doesn’t cure the infection itself and never replaces medical evaluation or prescribed antibiotics when they’re needed.
Use only the solutions your doctor specifically approves for you.
⚠️ Don’t put essential oils or homemade mixtures in any nebulizer, and don’t rely on a steam inhaler to deliver prescription breathing medications. Always follow your doctor’s instructions for devices and solutions.
Talk to your doctor before trying a new medication, changing any dose, or starting nebulized saline. For an overview of how to use a portable device effectively, the step‑by‑step guide to a portable mesh nebulizer can be a helpful companion to your clinician’s instructions.
Takeaway: Walking pneumonia usually improves over one to two weeks, but the cough can last for several weeks, so focus on steady progress, comfortable breathing, and regular check‑ins with your doctor if symptoms change.
Is Walking Pneumonia Contagious And How Long Does It Last
Walking pneumonia is contagious, but it tends to spread quietly through close contact over time rather than in one dramatic burst.
How It Spreads
According to the CDC, Mycoplasma pneumoniae spreads through respiratory droplets when an infected person coughs, sneezes, talks, or shares close air space. School‑age children, families living together, college dorms, military barracks, and crowded indoor settings are common places for spread.
The incubation period, or time between exposure and symptoms, can be longer than for most other infections. Symptoms can appear one to three weeks after contact, and sometimes even later.
How Long Symptoms And Cough Can Linger
A lot of people feel clearly sick for one to two weeks, then start to improve. Fatigue and a lingering cough can stretch on for several more weeks as the lungs heal.
You can still be contagious while you feel only mildly unwell. People are usually most contagious in the early phase of illness, before they realize they have more than a simple cold.
Exact timelines vary by person, and different medical sources give different ranges. Your doctor can give more specific guidance based on your case and whether you're taking antibiotics.
How To Lower The Chance Of Spreading It
Simple steps go a long way. Stay home from work, school, or daycare while you have a fever or a strong, frequent cough. Cover coughs and sneezes with your elbow or a tissue, wash your hands with soap and water, and avoid sharing drinks, utensils, or toothbrushes.
Wearing a well‑fitted mask in crowded indoor spaces can reduce the spread of respiratory droplets, especially early in illness or if you live with someone at high risk, such as an older adult or a person with asthma, COPD, or a weak immune system.
Regular cleaning of high‑touch surfaces and good ventilation also help. There is no vaccine that directly prevents Mycoplasma pneumoniae, but staying up to date on flu, COVID‑19, and other recommended vaccines lowers your chances of getting very sick from overlapping infections.
Takeaway: Walking pneumonia spreads slowly through close contact and can cause a cough that lingers for weeks, so handwashing, masking in crowded indoor spaces, and staying home when you're coughing or feverish help protect the people around you.
Frequently Asked Questions
Tap or click a question below to see the answer:
Early signs usually feel like a slow‑burning chest cold. You might notice a scratchy throat, dry or hacking cough, mild headache, and feeling more tired than usual. A low‑grade fever or chills can show up, but not always. When the cough and fatigue keep dragging on instead of improving, doctors start to suspect walking pneumonia.
Yes. You can have walking pneumonia with only a small temperature rise or no clear fever at all. This is especially common in older adults and in people who take medicines that blunt fever. Pay more attention to how long the cough lasts, how your chest feels, and whether you're short of breath, not just the thermometer reading.
At home, it's hard to tell bronchitis from walking pneumonia. Bronchitis usually follows a cold and brings a wet, rattly cough with lots of mucus. Walking pneumonia is more likely to cause a deep, lingering cough, tiredness, chest discomfort, and shortness of breath. A doctor exam, and sometimes a chest X‑ray, is needed to sort it out.
A walking pneumonia cough usually lasts longer than a regular cold. The main illness phase improves over one to two weeks, but the cough can hang on for three to six weeks while the airways heal. Call your doctor if the cough suddenly gets worse, you cough up blood, or breathing becomes harder.
Yes. Walking pneumonia is often mild, but it can spread to more of the lungs or become a more severe pneumonia. This risk is higher in very young children, older adults, smokers, and people with asthma, COPD, heart disease, or weak immune systems. Worsening shortness of breath, chest pain, or new high fever should trigger urgent care.
A bacterial walking pneumonia, such as one caused by Mycoplasma pneumoniae, usually becomes less contagious after you've taken the right antibiotic for a few days. Exact timing differs from person to person. Your cough can still last for weeks, so keep covering coughs, washing hands, and follow your doctor's advice about when to return to work or school.
Mycoplasma pneumoniae tends to cause gradual symptoms like sore throat, dry or hacking cough, low‑grade fever, headache, and fatigue. Some people also notice ear pain or mild chest discomfort. Children might have wheezing, watery eyes, nasal congestion, or stomach upset. Because the early picture is mild, it's a common cause of walking or atypical pneumonia.
After COVID‑19, some people notice extra shortness of breath, chest tightness, or fatigue when they later develop walking pneumonia. Symptoms from COVID and walking pneumonia can overlap, so testing and a doctor exam are important. A new spike in fever, fresh chest pain, or worse breathing after COVID should be checked quickly.
Takeaway: Persistent cough, fatigue, and breathing changes are strong reasons to ask a doctor about walking pneumonia, even if your fever is mild or has gone away.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always talk with your doctor about your symptoms, questions, or before starting or changing any treatment.