On this page
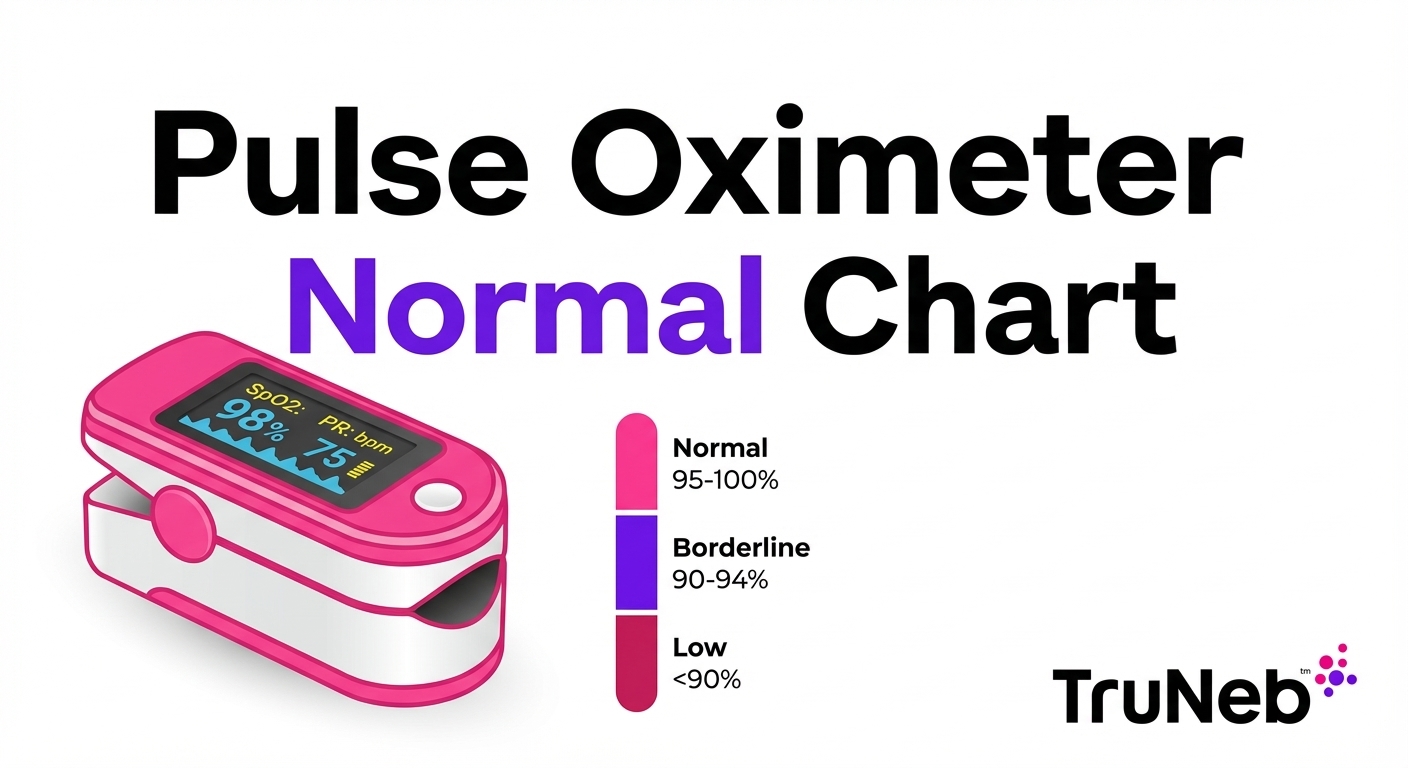
A pulse oximeter clips on your finger and shows two numbers: your blood oxygen saturation (SpO₂) and your pulse rate. For most healthy adults at sea level, a normal SpO₂ is between 95% and 100%, and a normal resting pulse is usually between 60 and 100 beats per minute.
Key point: For most adults, SpO₂ of 95–100% at rest is normal, numbers under 90% are usually considered low and need medical attention, and 88% or lower is a red‑flag level that usually needs emergency care, especially with symptoms.
Think of SpO₂ as a percentage of how many of your red blood cells are carrying oxygen. The higher the number (up to 100%), the better your blood is being oxygenated. Your pulse rate is simply how many times your heart beats in one minute.
Always remember: these are general ranges. Your own “normal” can be a little different if you have lung disease, heart problems, or live at high altitude. Your doctor is the one who should set your personal target.
Talk to your doctor before changing any medications or oxygen settings based on home readings.
One-liner: A pulse oximeter’s top number is your blood oxygen saturation (SpO₂) and the lower number is your pulse rate in beats per minute, with 95–100% SpO₂ considered normal for most healthy adults at rest.
Normal Pulse Oximeter Readings for Healthy Adults

For a healthy adult at sea level, a normal blood oxygen level on a pulse oximeter is usually between 95% and 100%. This means almost all of your hemoglobin is carrying oxygen, which is what your body needs to work well.
Most people will see readings in the high 90s when they’re resting, breathing comfortably, and not sick. A normal resting heart rate for adults is generally between 60 and 100 beats per minute, with athletes or very relaxed people sometimes being a bit lower.
SpO₂ readings below the mid‑90s can be a sign that something is off. Some guidance says 94% or less is usually considered below normal for a healthy person at sea level. A single reading of 93–94% when you feel fine might not be an emergency, but it’s worth watching. If you stay in the low‑90s (around 90–94%) or start to feel short of breath, that’s a sign to talk with a doctor.
Pulse oximeters have a small error range, usually around ±2%. So if you see 95%, your true oxygen level might be anywhere from about 93% to 97%. That’s why patterns over time matter more than any one number.
One-liner: For most healthy adults at sea level, a normal resting SpO₂ on a pulse oximeter is about 95–100%, with values below 90% usually considered low.
Common SpO₂ ranges for a healthy adult
95–100%: This is the normal range for most adults at sea level. Your blood is carrying plenty of oxygen and no action is needed if you feel well.
90–94%: This is a slightly low or borderline range. Sometimes this happens from minor issues like a cold finger, poor sensor placement, or a mild illness. Recheck the reading, fix any obvious problems, and keep an eye on your numbers and symptoms.
88–89%: For a healthy person, this is considered low (mild hypoxemia). Make sure the reading is accurate by sitting still, warming your hand, and checking again. If it stays under 90% or you feel unwell, you should call your doctor for advice.
88% or lower: This is dangerously low for most adults. Guidance from large medical centers usually uses 88% as a clear danger sign. If your reading is 88% or lower and doesn’t quickly improve, especially if you feel short of breath, confused, or notice bluish lips or fingers, you should get emergency care.
Key point: An SpO₂ of 88% or lower is widely used as a threshold for severe low oxygen and usually means you should seek urgent or emergency care.
One-liner: SpO₂ in the mid‑90s is usually normal, low‑90s need watching, and any persistent reading at or below 88% is a medical red flag.
People with chronic lung diseases like COPD usually have lower “normal” oxygen levels than healthy adults. Their lungs simply can’t keep SpO₂ in the high 90s all the time, even when they’re stable.
For people with moderate to severe COPD, an oxygen saturation around 88–92% can be acceptable and safe when it’s set by their doctor. This range is usually the target when they use home oxygen. In this case, an SpO₂ of 90% might be normal for them but would be low for someone without lung disease.
Even in COPD, there’s a lower limit. When readings stay below 88%, that’s usually considered too low and can put organs at risk. Some guidance notes that readings around 84% or lower are dangerous and usually need hospital care.
The most important thing is that your doctor should set your personal target range. For example, your doctor might say to keep your oxygen between 90% and 94% on your home oxygen, and to call the clinic if it stays below 88%. You shouldn’t change your oxygen flow or ignore low readings on your own.
One-liner: Lots of people with COPD have a doctor‑set target SpO₂ around 88–92%, but any persistent reading below 88% is considered too low even for chronic lung disease.
Oxygen Saturation Levels: Healthy Adult vs COPD

Oxygen levels can dip a little during sleep, but they should still stay in a safe range. In healthy adults, normal oxygen saturation during sleep is usually about 95–100%, similar to daytime levels.
Short, small drops into the low‑90s can happen in deeper sleep stages or if you live at higher altitude. These brief dips are usually not a problem if your oxygen comes right back up and you feel well during the day.
What isn’t normal is for your SpO₂ to stay low for long periods while you sleep. Frequent or long drops below about 90% can point to a breathing problem like sleep apnea. Readings below 88% at night are especially concerning.
If you use an overnight oximeter and see many episodes in the 80s, or if your average overnight oxygen is low, it’s important to tell your doctor. Signs like loud snoring, gasping in sleep, morning headaches, or strong daytime sleepiness along with low readings can be clues to sleep apnea or another sleep‑related breathing disorder.
One-liner: During normal sleep, most healthy adults keep SpO₂ around 95–100%, and repeated drops below 90% or any sustained levels under 88% at night should be checked by a doctor.
Home pulse oximeter numbers can jump around from one reading to the next. A lot of these changes are tied to how the device is used, not sudden shifts in your health.
Cold hands or poor circulation can make it hard for the sensor to pick up a clear signal. This can cause falsely low readings. Warming your hands, rubbing your fingers, or letting your arm hang and swing gently for a moment can improve blood flow before you test.
Placement and movement matter too. If the clip is loose, crooked, or you’re moving your hand, the device can show shaky or wrong numbers. When you check, sit still, rest your hand at heart level on a table, and wait a few seconds for the reading to settle.
Dark nail polish and some artificial nails can block or weaken the light from the sensor. Certain colors, like dark blue, green, black, or brown, can cause the oximeter to read lower than your true oxygen level by a few points. If possible, take polish off the finger you use, or try a different finger.
Research has also found that standard oximeters can be slightly less accurate in people with darker skin tones, sometimes overestimating oxygen when it’s low. This effect is usually small, but it can delay noticing a problem. If you have darker skin and get a borderline reading, but you feel clear symptoms of low oxygen, treat that seriously and contact a doctor.
Cheap or poorly made devices and weak batteries can add more error. Most good devices are within about 2–4 percentage points of the true value when you use them correctly, but some low‑cost models can be less precise.
One-liner: Common causes of shaky pulse oximeter readings include cold fingers, movement, poor placement, nail polish, skin tone effects, and low‑quality or low‑battery devices.
Things to make your pulse oximeter readings more reliable

Sit down and rest for a couple of minutes before checking. Place the oximeter on a warm, clean finger, usually the index or middle finger. Rest your hand on a flat surface at about heart level and avoid talking or moving while the device measures.
Give the device time to settle. Many oximeters will show quickly changing numbers at first. Wait at least 10–20 seconds until the reading stops jumping before you note the value.
If the number looks odd or doesn’t fit how you feel, recheck on a different finger. You can also try using another oximeter, if you have access to one, to compare. Even with perfect use, most devices have a small error range of a few percentage points.
If you use a pulse oximeter often for a medical condition, bring it to your next appointment. Ask your doctor or nurse to compare your device against their office monitor so you know how close it runs. This can help you trust the trends you see at home.
Talk to your doctor before trying any new medications or changing existing treatments based on home pulse oximeter readings.
One-liner: For more accurate home readings, use a warm finger, sit still with your hand at heart level, wait for the numbers to stabilize, and verify unusual results on another finger or device.
Instead of worrying about one reading, it helps to track your pulse oximeter numbers over days and weeks. This is especially useful if you have COPD, asthma, heart disease, or are recovering from an illness.
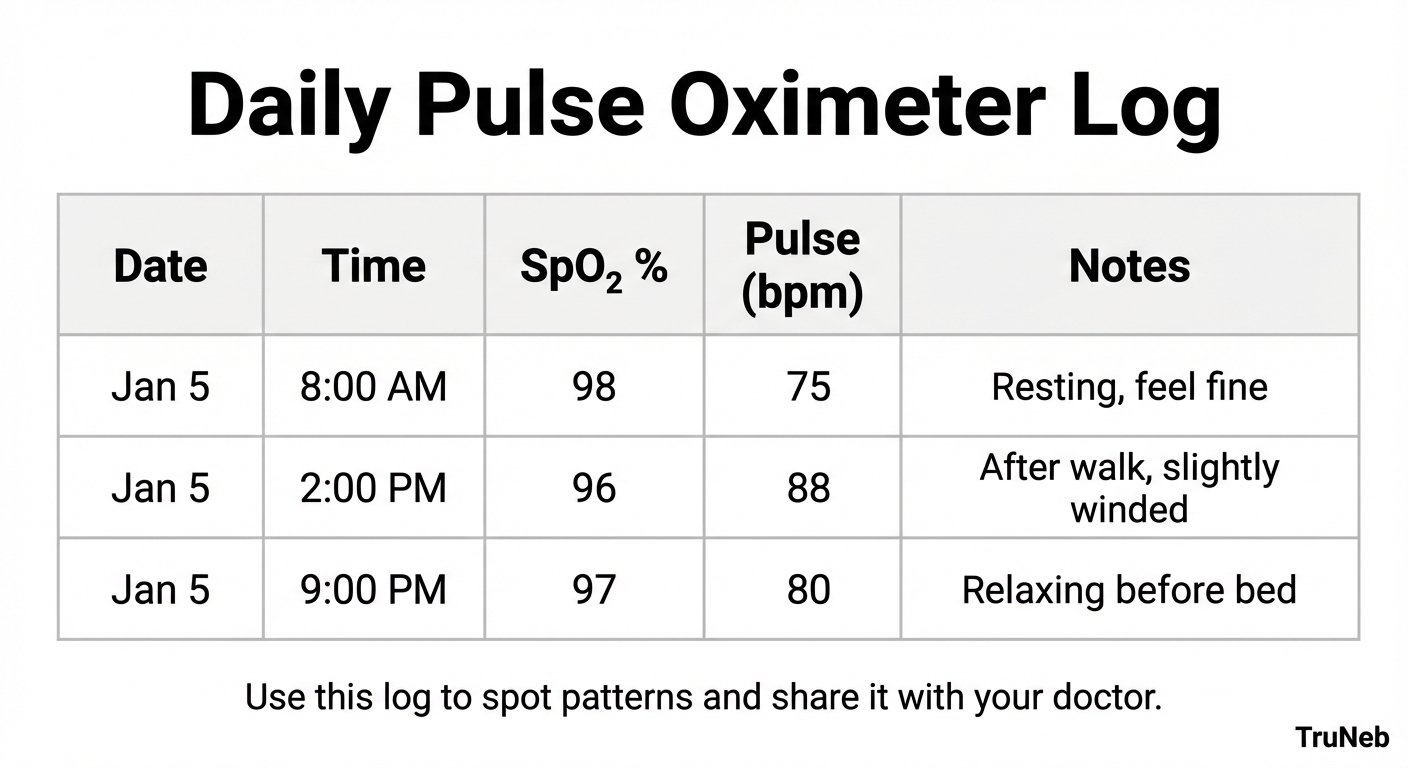
You can use a simple notebook, a printed chart, or a basic spreadsheet. For each check, write the date, time, SpO₂, pulse, and a short note about what you were doing and how you felt. For example:
- Jan 5, 8:00 AM – SpO₂ 98%, pulse 75 (resting, feel fine)
- Jan 5, 2:00 PM – SpO₂ 96%, pulse 88 (after short walk, slightly winded)
- Jan 5, 9:00 PM – SpO₂ 97%, pulse 80 (relaxing before bed)
Over time, this kind of log lets you and your doctor see patterns. You might notice that your oxygen dips at a certain time of day, during certain activities, or when you’re coming down with a cold. For people on home oxygen, noting the flow rate at each reading (for example, “on 2 L/min”) adds important context.
Bring this log to your clinic visits. It gives the care team a clearer picture than one quick office reading. Some oximeters and apps can record data automatically, but a simple written log works just as well if you fill it out regularly.
One-liner: A basic daily log of SpO₂, pulse, time, and symptoms can turn scattered readings into a clear pattern your doctor can use.
Daily Pulse Oximeter Log
Numbers on your pulse oximeter only make sense when you match them with how you feel.
If your SpO₂ is in the low‑to‑mid 90s (around 90–94%) and you feel okay, it’s a sign to watch closely. Recheck the reading, make sure your hands are warm, and fix any issues with placement. If that range is unusual for you or it stays there, contact your doctor’s office to let them know.
If your SpO₂ repeatedly falls to 92% or below, or it stays under 92% for about an hour, most guidance says you should call your doctor or clinic the same day. They can tell you if you need to come in, adjust part of your plan, or go to urgent care.
If your SpO₂ is 88% or lower and doesn’t quickly improve, treat that as an emergency. A lot of large medical centers use 88% as a clear cutoff for severe low oxygen. You should go to the emergency room or call emergency services, especially if you have trouble breathing, chest pain, confusion, or see a bluish color on your lips or fingertips.
Also listen to your body. If you feel like you can’t breathe, feel faint, or have severe chest pain, seek emergency care right away, even if the oximeter number doesn’t look very low.
Talk to your doctor before trying any new medication or changing prescribed treatments in response to home readings.
One-liner: In general, low‑90s SpO₂ calls for close watching, repeated readings at or below 92% deserve a same‑day call to your doctor, and 88% or lower is an emergency level that usually needs ER care.
Frequently Asked Questions
Tap or click a question below to see the answer:
What do the two numbers on a pulse oximeter mean? ▼
The higher number is your oxygen saturation (SpO₂), which is the percentage of oxygen in your blood. The other number is your pulse rate in beats per minute, often labeled PR or shown next to a heart symbol. For example, if you see 98 and 75, that usually means your SpO₂ is 98% and your heart rate is 75 beats per minute.
What is a normal oxygen level for adults? ▼
For most healthy adults at sea level, a normal resting oxygen level is about 95–100% SpO₂. Levels in the low-90s (around 90–94%) can be a little lower than ideal and need watching, especially if they stay there. Values below 90% are usually considered low and should be discussed with a doctor.
What is a normal oxygen level for someone with COPD? ▼
Lots of people with COPD have a lower normal range set by their doctor, often around 88–92% SpO₂. A COPD patient might sit at 90% and be stable if that matches their plan. But if their reading is consistently below their usual range, especially under 88%, that is too low and needs medical help.
When should I go to the ER for a low oxygen reading? ▼
You should go to the ER or call emergency services if your SpO₂ drops to 88% or below and does not quickly improve, especially if you also feel short of breath, have chest pain, feel confused, or notice blue lips or fingers. Do not ignore serious symptoms just because the number does not look very low.
How accurate are home pulse oximeters? ▼
Good-quality home oximeters are usually within about 2–4 percentage points of your true oxygen level when used correctly. So a reading of 95% might mean your actual oxygen is somewhere between about 91% and 99%. Accuracy can be affected by cold fingers, movement, nail polish, skin tone, device quality, and low batteries.
Can I rely only on a pulse oximeter to decide if I am okay? ▼
No. A pulse oximeter is just one tool. Do not ignore serious symptoms like trouble breathing, chest pain, confusion, or blue lips and fingers just because your number looks okay. Always match the reading with how you feel and talk with your doctor about any concerns.
One-liner: A home pulse oximeter is a helpful tool to track trends in SpO₂ and pulse, but your personal targets and action steps should always come from your doctor.