On this page
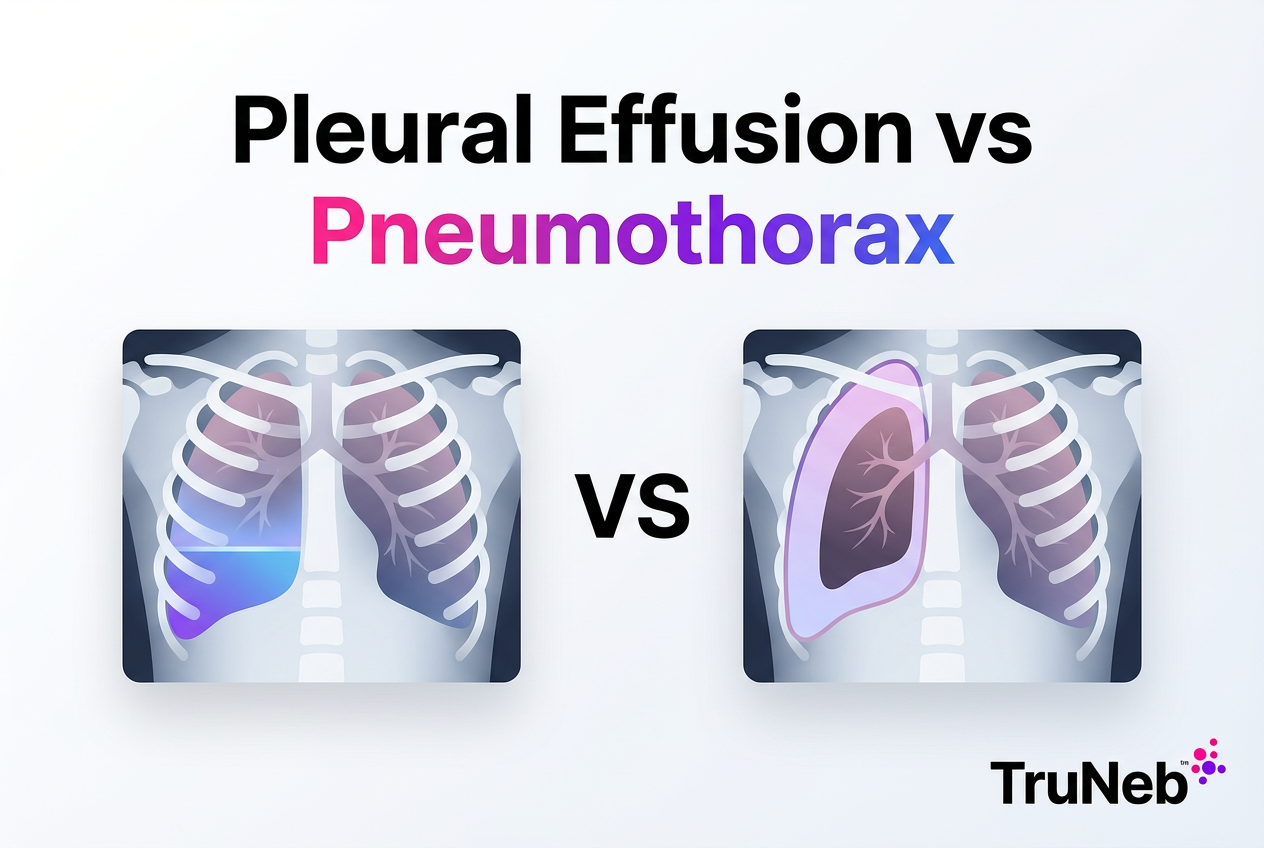
Pleural Effusion vs Pneumothorax: Causes, Symptoms, Imaging Differences & Emergency Treatment
Here’s the simple difference: a pleural effusion is fluid building up in the pleural space around your lung. A pneumothorax is air in that space that can make the lung collapse.
Both affect breathing. Both need medical care. The paths to care are different.
At a glance:
- Pleural effusion = fluid around the lung, often from another illness like heart failure or infection.
- Pneumothorax = air leak in the chest, often sudden after an injury or from weak spots in the lung.
- Imaging tells them apart quickly and guides treatment.
Pleural effusions are common, with well over a million cases in the U.S. each year. Pneumothorax is less common but can strike suddenly. The good news: doctors can usually treat both effectively once they confirm what’s going on.
Key takeaway: Pleural effusion is fluid around the lung, while pneumothorax is air in the pleural space that can collapse the lung.
Understanding the Pleural Space and Why It Matters
Your lungs are wrapped in a thin lining called the pleura. Between the lung and the chest wall is a tiny space in the chest cavity with a few drops of slippery fluid so your lungs can glide as you breathe.
That space should stay almost empty. When fluid fills it (effusion) or air slips in (pneumothorax), pressure builds and the lung can’t fully expand. Even a small pocket of extra air is abnormal and can collapse part of the lung, while small amounts of extra fluid might be silent until larger volumes build. Breathing can feel tight, painful, or both.
Key takeaway: The pleural space is a thin slide zone around your lungs, and extra fluid or air in that space prevents your lungs from fully expanding.
Causes of Pleural Effusion and Pneumothorax
Why these happen:
Pleural effusion (fluid around the lung):
- Heart failure (most common cause)
- Lung infection like pneumonia
- Cancer involving the lung or pleura
- Blood clots in the lung (pulmonary embolism)
- Kidney disease or liver cirrhosis
- Tuberculosis or autoimmune disease
Pneumothorax (air leak and lung collapse):
- Spontaneous rupture of a small air blister (bleb) on the lung surface, which can happen in tall, thin people
- Chronic lung disease (COPD/emphysema, cystic fibrosis, severe asthma)
- Trauma (rib fracture, stab wound, car crash)
- Damage from medical procedures or from high pressure on a ventilator (iatrogenic/barotrauma)
- Smoking increases risk of spontaneous pneumothorax
Some effusions come from pressure or fluid balance problems like heart failure (transudative), while others come from inflammation, infection, or cancer (exudative).
Big picture: Effusions usually come from another illness, while pneumothorax usually comes from a sudden air leak or injury.
Key takeaway: Pleural effusion usually develops as a complication of another condition, while pneumothorax typically comes from a sudden air leak or chest injury.
Symptoms and Signs: Fluid vs Air on the Lungs
Both can cause chest discomfort and shortness of breath. The timing and feel can differ.
Pleural effusion (fluid):
- Shortness of breath that can build over days
- Dull chest ache or a sense of heaviness
- Cough; fever if due to infection
- Breathlessness can worsen when lying flat or with exertion
- On exam, breath sounds are reduced on the affected side; tapping the chest sounds dull over fluid
Pneumothorax (air):
- Sudden, sharp chest pain on one side
- Abrupt shortness of breath
- Anxiety, fast breathing; blue lips or fingers if severe
- On exam, breath sounds can be absent; tapping the chest can sound hollow over extra air
If pressure builds fast (tension pneumothorax), the windpipe can shift away from the affected side and blood pressure can drop. That’s an emergency.
Because the symptoms overlap with each other—and even with heart attacks or pulmonary embolism—you can’t safely self-diagnose. Doctors use imaging to confirm exactly what’s going on.
Key takeaway: Pleural effusion symptoms usually build over time, while pneumothorax symptoms tend to start suddenly with sharp one‑sided chest pain.
Diagnosis and Imaging: How Doctors Tell Pleural Effusion and Pneumothorax Apart
Doctors combine your story and a physical exam with imaging. Exam clues can include reduced or absent breath sounds and a dull (effusion) versus hollow, hyperresonant (pneumothorax) sound when the chest is tapped, but imaging confirms the diagnosis.
Chest X‑ray: Pleural effusion typically shows blunted costophrenic angles and a curved meniscus of fluid at the lung base. Pneumothorax shows a thin, sharp pleural line with no lung markings beyond it and, in larger cases, a visible edge of a partially collapsed lung.
Ultrasound: At the bedside, effusion appears as a dark (anechoic) fluid pocket; pneumothorax shows no lung sliding.
CT scan: Used when the X‑ray is unclear, the case is complex, or to assess underlying disease (for example, small pneumothoraces, loculated effusions, trauma, or suspected cancer).
Thoracentesis: Removing a sample of pleural fluid helps determine the cause of an effusion (infection, cancer, or heart‑failure‑related) and can relieve symptoms.
On imaging, pleural effusion looks like fluid layering around the lung, while pneumothorax shows a dark rim of air with a visible pleural line.
| Modality | Pleural effusion shows | Pneumothorax shows | When doctors use it |
|---|---|---|---|
| Chest X‑ray | Blunted costophrenic angle, meniscus sign, fluid at lung base | Thin pleural line, no lung markings beyond, lung edge visible | First‑line test to confirm and estimate size |
| Ultrasound | Dark (anechoic) fluid pocket; can estimate volume | Absent lung sliding | Bedside confirmation when speed matters |
| CT scan | Detects small/loculated effusions and underlying causes | Detects small pneumothoraces and related injuries | Complex or uncertain cases; guides procedures |
Note: Appearance can vary with patient position; doctors may use multiple views.
See the infographic description below for a side‑by‑side X‑ray view.
Infographic prompt: Simple side-by-side visual titled "Pleural Effusion vs Pneumothorax: What You See on X-ray". Left panel (Pleural Effusion): label "Fluid in pleural space", show blunted costophrenic angle and a curved meniscus line (white at lung base), small water droplet icon. Right panel (Pneumothorax): label "Air in pleural space", show a visible pleural line with no lung markings beyond and a dark rim of air, small air bubble icon. Footer notes: "Ultrasound: Effusion = dark fluid pocket; Pneumothorax = no lung sliding". One small stat: "Pleural effusions >1 million/year (US)". Clean, high-contrast, no tiny text.
Key takeaway: On imaging, pleural effusion shows fluid layering around the lung, while pneumothorax shows a dark rim of air and a visible collapsed lung edge.
Treatment and Emergency Management
Pleural effusion:
- Doctors sometimes watch small effusions while they treat the cause (for example, diuretics for heart failure or antibiotics when infection is present).
- If an effusion is large or really uncomfortable, doctors usually drain it with a procedure called thoracentesis, using a needle or small catheter. If fluid is infected or keeps coming back, a chest tube or pleurodesis may be needed.
- Long-term control focuses on treating the underlying cause so the fluid doesn’t return.
Pneumothorax:
- In the hospital, doctors sometimes observe small, stable pneumothoraces with oxygen; the air can absorb over days.
- Medium to large ones usually need air removed: needle aspiration or a chest tube until the lung re-expands.
- A tension pneumothorax is an emergency handled by doctors with immediate needle decompression, then a chest tube.
- These procedures are done by emergency or hospital teams, not at home.
- Recurrent cases sometimes need surgery (VATS) to repair leaks and prevent future collapses.
Bottom line: Both problems frequently need a tube to remove what doesn’t belong (fluid or air), but the steps and urgency differ.
Key takeaway: Effusion is drained and its cause treated; pneumothorax air is released so the lung can re-expand.
When to Seek Emergency Care
Both conditions can become life-threatening. Call 911 or go to the ER now if you have:
- Severe shortness of breath (can’t speak full sentences)
- Sudden, sharp one-sided chest pain
- Blue or gray lips or face (cyanosis)
- Dizziness, confusion, or fainting
- Very fast breathing or heart rate that doesn’t settle
- In tension pneumothorax, medics can see the windpipe pulled off center, low blood pressure, and bulging neck veins
Sudden chest pain plus shortness of breath could also be a heart attack or a pulmonary embolism—always better to be checked.
Don’t try to ride this out at home with an inhaler or a nebulizer. These are emergencies that need hospital procedures. Emergency teams can quickly use imaging and procedures to stabilize these conditions.
Key takeaway: Sudden one‑sided chest pain with severe shortness of breath is an emergency—get help now.
Managing Lung Health Afterward & Preventing Future Issues
After treatment, focus on keeping your lungs as healthy as possible:
- Follow up with your lung doctor (pulmonologist) and stick to the plan for your underlying condition.
- Stay up to date on vaccines (flu, pneumonia) to lower infection risk.
- Don’t smoke, and avoid secondhand smoke.
- If your doctor recommends airway clearance, that might include breathing exercises, devices, or physical therapy to help move mucus.
While good airway care doesn’t directly prevent a pleural effusion or a pneumothorax, it supports overall lung health and can reduce infections that put extra stress on your lungs.
Some people with mucus-heavy lung disease use a portable mesh nebulizer, such as TruNeb™, as part of their doctor‑guided airway clearance plan. Under your doctor’s guidance, nebulized hypertonic saline (3% or 7%) can help thin sticky mucus so it’s easier to clear. These solutions are prescription medications and aren’t right for everyone; your doctor will decide if they’re safe for you. Research suggests this approach can make mucus easier to clear, and some studies suggest it can reduce infections and flare‑ups in conditions like COPD, bronchiectasis, or cystic fibrosis. You might also see boxes labeled “steam inhaler”—those are for warm mist only and are not used for breathing medications the way a nebulizer is.
Safety note: Talk to your doctor before trying a new medication or nebulizer solution. A nebulizer does not treat an acute pleural effusion or a collapsed lung; those need emergency care and procedures.
Key takeaway: If you live with chronic lung disease, daily airway care and regular follow‑up can help cut down infections and flare‑ups that set you back.
Frequently Asked Questions
Tap or click a question below to see the answer:
The difference between pleural effusion and pneumothorax is simple: effusion is fluid around the lung, while pneumothorax is air in the pleural space that can collapse the lung. Imaging confirms which one it is.
Both can be serious. A large effusion can cause breathing failure if untreated. A tension pneumothorax is rapidly life‑threatening and needs emergency care.
Chest X‑ray is usually first. Effusion shows a fluid level; pneumothorax shows a clear rim of air with a sharp lung edge. Ultrasound and CT add detail. Effusions are sometimes sampled with a needle (thoracentesis) to find the cause.
Yes. Trauma, or occasionally a complication during drainage, can lead to both air and fluid in the pleural space. This is sometimes called a hydropneumothorax (air and fluid together). Doctors look for this on imaging and treat both.
Small effusions or pneumothoraces can improve in days. Larger ones usually need procedures and a short hospital stay. Full recovery depends on the cause and your overall lung health.
Key takeaway: Fluid vs air is the core difference; severe cases need prompt care and imaging to guide treatment.
Conclusion
In short: pleural effusion is fluid, pneumothorax is air, and both can make breathing hard. Imaging tells them apart fast, and modern treatments work well. If symptoms are sudden or severe, treat it like an emergency. If you ever have sudden chest pain or trouble breathing, don’t wait—get emergency care. For day‑to‑day lung care, work with your doctor and use tools that support airway health so you can stay active and breathe easier.
Key takeaway: Know the fluid‑vs‑air difference, act fast for severe symptoms, and protect your lungs every day.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always talk with your doctor about any symptoms, questions, or changes to your treatment plan.