On this page

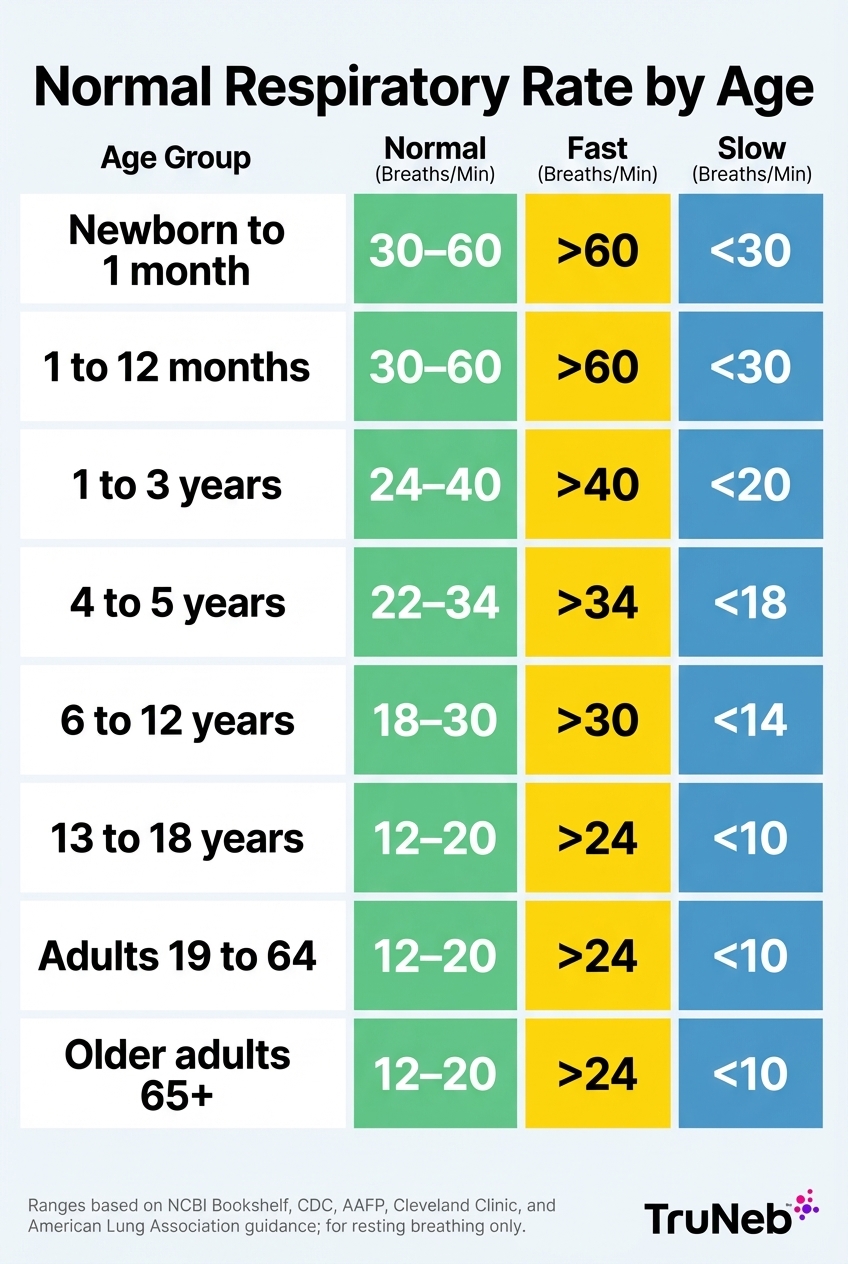
Normal Respiratory Rate by Age Chart
Respiratory rate is the number of breaths someone takes in one minute while resting.
This normal respiratory rate by age chart shows a typical resting respiratory rate chart by age, with breaths per minute for newborns through older adults.
These numbers apply to a calm person who is awake and resting, not right after activity, crying, or a treatment.
Key point: The number matters, but how hard someone is working to breathe matters even more.
| Age Group | Expected Resting Respiratory Rate (breaths per minute) | Fast Breathing That Can Be Concerning* | Slow Breathing That Can Be Concerning* |
|---|---|---|---|
| Newborn to 1 month | 30–60 | More than about 60 at rest | Fewer than about 30 with poor tone or color |
| 1 to 12 months (infant) | 30–60 | More than about 60 at rest | Fewer than about 30 with poor tone or color |
| 1 to 3 years (toddler) | 24–40 | More than about 40 at rest | Fewer than about 20 with low energy or color change |
| 4 to 5 years (preschooler) | 22–34 | More than about 34 at rest | Fewer than about 18 with symptoms |
| 6 to 12 years (school-age) | 18–30 | More than about 30 at rest | Fewer than about 14 with symptoms |
| 13 to 18 years (adolescent) | 12–20 | More than about 24 at rest | Fewer than about 10 with symptoms |
| Adults 19 to 64 years | 12–20 | More than about 24 at rest | Fewer than about 10, especially with sleepiness or confusion |
| Older adults 65+ years | 12–20 (some run 12–22) | More than about 24 at rest | Fewer than about 10, especially with medications like opioids or sedatives |
*These cutoffs are general alarm ranges for home monitoring, not strict hospital rules. These are approximate ranges from CDC, NCBI Bookshelf, AAFP, Cleveland Clinic, and the American Lung Association for resting respiratory rate, not strict hospital cutoffs.
If a breathing rate falls outside the expected resting range and you also see signs of respiratory distress such as retractions, nasal flaring, blue lips (cyanosis), or trouble speaking, treat it as urgent and seek medical care right away.
Talk to your doctor before making any decisions about medication or treatment based on respiratory rate at home.
Key takeaway: Normal breaths per minute change with age, and in general, infants breathe much faster than adults while older children and adults cluster around 12 to 20 at rest.
What Counts as a Normal Breathing Rate in Each Age Group
Normal breaths per minute depend on age. Babies breathe the fastest, and the rate gradually slows as the lungs grow and the body becomes more efficient.
Newborns and Infants
Newborns and infants typically breathe in quick, short bursts. Their lungs and chest wall are still developing, so a higher breathing rate is normal.
According to NCBI Bookshelf and CDC tables, most healthy newborns and infants at rest breathe about 30 to 60 times per minute. It’s also normal for their breathing to look a little irregular, with short pauses under 10 seconds.
Crying, feeding, fever, or excitement can push the number higher for a short time. For instance:
- A calm, sleeping 3‑month‑old at 36 breaths per minute is usually fine.
- A wide-awake, crying baby at 54 breaths per minute can still be within a normal response to stress.
Worry sooner if a baby is breathing faster than about 60 breaths per minute at rest and also shows nasal flaring, grunting, retractions (pulling in between the ribs), or poor feeding. Those can be signs of bronchiolitis, RSV, pneumonia, or other respiratory distress and need prompt medical care.
Toddlers, Preschoolers, and School-Age Children
As children grow, their lungs get larger and more efficient, so the normal respiratory rate gradually slows.
AAFP pediatric standards and CDC training materials suggest these resting ranges:
- Toddlers (about 1 to 3 years): typically 24 to 40 breaths per minute
- Preschoolers (about 4 to 5 years): around 22 to 34 breaths per minute
- School-age children (about 6 to 12 years): about 18 to 30 breaths per minute
For these ages, it’s important to count only when the child is calm. Counting right after running, laughing hard, or crying can give a misleading high number.
A few examples:
- A relaxed 4‑year‑old watching a show with a rate of 26 is usually normal.
- A 7‑year‑old breathing 32 times per minute while sitting still, plus cough and chest pulling in, can signal trouble.
If a child’s resting rate is above the expected range and they also have fever, wheezing, retractions, blue lips, or struggle to speak, they need urgent care. For parents, it helps to remember that the normal breathing rate for a child is higher than for an adult, so always use age-based ranges.
Teens, Adults, and Older Adults
By the teen years, respiratory rate starts to look like adults. Cleveland Clinic and the American Lung Association note that a normal respiratory rate normal range for adults at rest is about 12 to 20 breaths per minute.
In healthy adolescents and adults:
- A rate of 12 to 18 at rest is very typical.
- Some fit people can rest as low as 10 to 12 without symptoms.
For older adults, the normal respiratory rate for older adults is still about 12 to 20 breaths per minute, though some sit slightly higher (for example 20 to 22) because of reduced lung elasticity, deconditioning, or chronic illness. The key is what’s normal for that person.
Chronic conditions like asthma, COPD, heart failure, or anemia can shift the baseline a little higher, especially during flare-ups. Medications such as opioids and sedatives can slow breathing and, in higher doses, can cause dangerous respiratory depression (dangerously slow or shallow breathing) and dyspnea (shortness of breath).
According to MedlinePlus and the American Lung Association, a resting adult rate above about 24 breaths per minute or below about 10 with symptoms like confusion, blue lips, or extreme sleepiness can signal trouble.
Talk to your doctor before trying to change your medications or treatment plan based on breathing rate alone.
Key takeaway: A child’s normal breathing rate slowly drops from fast in infancy to around 18–30 in grade school, then settles at about 12–20 breaths per minute in the teen and adult years.
How to Check Respiratory Rate Correctly at Home
To check respiratory rate at home, you count how many breaths someone takes in one minute while they’re resting. This gives you their resting respiratory rate, which is the most useful number for spotting changes.
Best Time to Count Breaths
You get the most accurate reading when the person is resting:
- Sitting or lying down quietly
- Not talking, eating, or laughing
- At least several minutes after exercise, coughing, or a nebulizer treatment
For babies and young children, counting during sleep or while they’re quietly watching something can work well. Cleveland Clinic and Healthline advise avoiding measurements right after a big cry, a coughing fit, or active play because the rate will be temporarily higher.
Step-by-Step Counting Method
Here is a simple way to count breaths per minute at home:
- Make sure the person is at rest. Wait a few minutes after any activity.
- Watch the chest or belly. One breath equals one full rise and fall.
- Use a timer and count breaths for a full 60 seconds. For a child with very regular breathing, you can count for 30 seconds and multiply by 2, but a full minute is safer.
- For babies, try to count without touching or telling them you’re counting. Touch or talking can change their rate.
- Write the number down and note the time, whether they were awake or asleep, and any symptoms like wheezing or fever.
StatPearls and other vital sign training guides stress that a full 60‑second count is best when breathing is irregular or when you’re worried.
Common Mistakes That Lead to Wrong Readings
Several small errors can make a normal respiratory rate look abnormal:
- Counting right after running, playing, or crying
- Counting for only 10 or 15 seconds and multiplying by 4 when breaths are irregular
- Watching the clock instead of the chest and losing count
- Measuring while someone is anxious about being observed
- Trying to count when heavy clothing or blankets make chest movement hard to see
- Confusing fast, shallow panting during distress with a stable resting rate
If you’re checking breathing because of a chronic condition like asthma or COPD, your doctor can suggest whether to also monitor oxygen saturation with a pulse oximeter and how to record both numbers in an action plan. You can also review how to check respiratory rate for a focused guide.
Talk to your doctor before changing inhalers, nebulized medications, or other treatments based on home respiratory rate checks.
Key takeaway: To measure respiratory rate at home, watch the chest at rest and count each rise for a full 60 seconds without drawing attention to it.
Tachypnea and Bradypnea by Age
Tachypnea vs bradypnea describes fast breathing versus slow breathing compared with the normal respiratory rate for someone’s age.
Tachypnea means abnormally fast breathing for age. Bradypnea means abnormally slow breathing for age.
In medical terms, respiratory rate is only one part of the story. You also need to look at work of breathing, color, and mental status.
What Tachypnea Means
Tachypnea is the medical word for rapid breathing that’s faster than the normal range for someone’s age at rest.
Examples based on CDC and NCBI Bookshelf ranges:
- A 2‑month‑old at rest breathing 70 times per minute is likely tachypneic.
- A calm 4‑year‑old at 40 breaths per minute at rest is on the high side and can be tachypneic.
- An adult sitting quietly at 28 breaths per minute is breathing faster than normal.
Tachypnea can happen for several reasons, including fever, asthma, bronchiolitis, pneumonia, heart failure, anxiety, or pain. In some severe illnesses, such as diabetic ketoacidosis, breathing can become deep and fast in a pattern called Kussmaul respirations, which are deep, labored, fast breaths seen in serious metabolic problems. That pattern is a medical emergency.
Fast breathing plus signs of respiratory distress such as nasal flaring, retractions, grunting, wheezing, blue lips, or trouble speaking needs urgent medical care.
What Bradypnea Means
Bradypnea is the medical word for abnormally slow breathing for age.
A slow rate can be normal in some situations:
- Well-trained athletes can have a resting adult respiratory rate closer to 10 per minute without symptoms.
- During sleep, breathing normally slows a little in both children and adults.
However, very slow or shallow breathing, especially with confusion, extreme sleepiness, or blue color, can signal dangerous respiratory depression (dangerously slow or shallow breathing). Common causes include:
- High doses of opioids
- Sedatives or certain seizure medicines
- Serious brain or neurologic problems
- Worsening critical illness
For instance, an adult on opioids breathing only 6 times per minute and hard to wake needs emergency help.
Why the Same Number Means Different Things at Different Ages
The same respiratory rate can be normal for one age and abnormal for another. That’s why age-specific charts are so important.
Consider these comparisons:
- A rate of 30 breaths per minute is normal in a calm toddler but high in a healthy adult at rest.
- A rate of 18 is normal in a school-age child or adult but can be too slow for a newborn.
Clinicians look at the combination of age, respiratory rate, and symptoms to decide if someone has tachypnea, bradypnea, or a normal variation. They also examine the pattern of breathing. Deep, labored Kussmaul respirations, stridor (high-pitched noise on breathing in), severe wheezing, or episodes of apnea (pauses in breathing) can each point to different urgent conditions. For related breathing sound differences, see stridor vs wheeze guide.
If you see an out-of-range number and the person also looks distressed, gets tired while breathing, has blue lips or fingers, or can’t speak in full sentences, seek emergency care.
Talk to your doctor before changing any prescribed medications, especially opioids, sedatives, or inhaled treatments, based on home breathing counts.
Key takeaway: Tachypnea is fast breathing and bradypnea is slow breathing, but what counts as fast or slow depends on the person’s age and overall symptoms.
What Can Make Respiratory Rate Go Up or Down
Lots of everyday things can change your breathing rate. Here’s what usually speeds it up and what can slow it down.
Respiratory rate is a sensitive vital sign. It often changes before blood pressure or heart rate when someone is getting sick or more stressed.
Common Reasons Breathing Gets Faster
A higher breathing rate (tachypnea) doesn’t always mean an emergency. Some common causes include:
- Fever: American Lung Association and Cleveland Clinic reports show that fever commonly speeds up breathing, especially in children.
- Exercise or play: Muscles demand more oxygen during movement, so breathing rate increases.
- Anxiety or panic attack: Fast, shallow breathing can show up with chest tightness, tingling, and a feeling of doom, along with dyspnea (shortness of breath).
- Asthma or COPD: Narrowed airways and trapped air make breathing harder, so rate and work of breathing can rise.
- Pneumonia or bronchiolitis: Infections in the lungs make it harder to move air and oxygen.
- Heart failure: Fluid in the lungs limits gas exchange, so the body compensates by breathing faster.
- Dehydration: With less circulating volume, the body can increase rate to move oxygen.
In chronic lung diseases like asthma and COPD, your doctor may give you an action plan that pairs respiratory rate with wheezing, cough, and pulse oximetry readings to guide when to use inhalers or nebulized medications.
A portable mesh nebulizer such as the TruNeb portable mesh nebulizer can help some people follow their prescribed inhaled medication plan more easily at home or while traveling. TruNeb doesn’t replace medical care, but it can support the routine your doctor recommends.
Common Reasons Breathing Gets Slower
Respiratory rate can also drop:
- Sleep: Mild slowing is normal during sleep across all ages.
- Opioids: Pain medicines like morphine or oxycodone can suppress the drive to breathe, especially in high doses or when combined with other sedatives.
- Sedatives and certain psychiatric medicines: Some can slow breathing and make it shallow.
- Brain or neurologic problems: Stroke, head injury, or brain infections can affect the breathing center in the brainstem.
- Severe fatigue or worsening illness: As someone tires out, rate may slow even while breathing effort stays high, which is very dangerous.
Very slow or shallow breathing, especially with confusion, snoring with long pauses, blue lips, or hard-to-wake behavior, needs emergency care.
Normal During Sleep vs Abnormal During Sleep
During healthy sleep, breathing slows slightly and can become a bit more regular. Healthline and MedlinePlus note that adults may drop toward the lower end of the 12 to 20 range, and children may move toward the lower end of their normal range. This still counts as a normal respiratory rate during sleep for that age if there are no other warning signs.
Sleep apnea is different. It involves repeated episodes of apnea (no breathing) or very shallow breaths during sleep, often with loud snoring, gasping, or witnessed pauses. Oxygen saturation can drop repeatedly. Over time, this can strain the heart and brain. If you want more context on nighttime oxygen concerns, see normal oxygen levels during sleep.
In adults using opioids or sedatives, it can be hard to tell normal sleep from dangerous respiratory depression. Warning signs include:
- Very slow or irregular breathing
- Long pauses between breaths
- Blue or gray lips (cyanosis)
- Failure to wake up with loud voice or firm shaking
If you suspect an overdose or see these signs, call emergency services right away.
Talk to your doctor before starting or stopping opioids, sedatives, or sleep apnea treatments. Never change doses on your own.
Key takeaway: Many things can shift respiratory rate up or down, but dangerous changes usually come with other warning signs like hard breathing, color change, confusion, or extreme sleepiness.
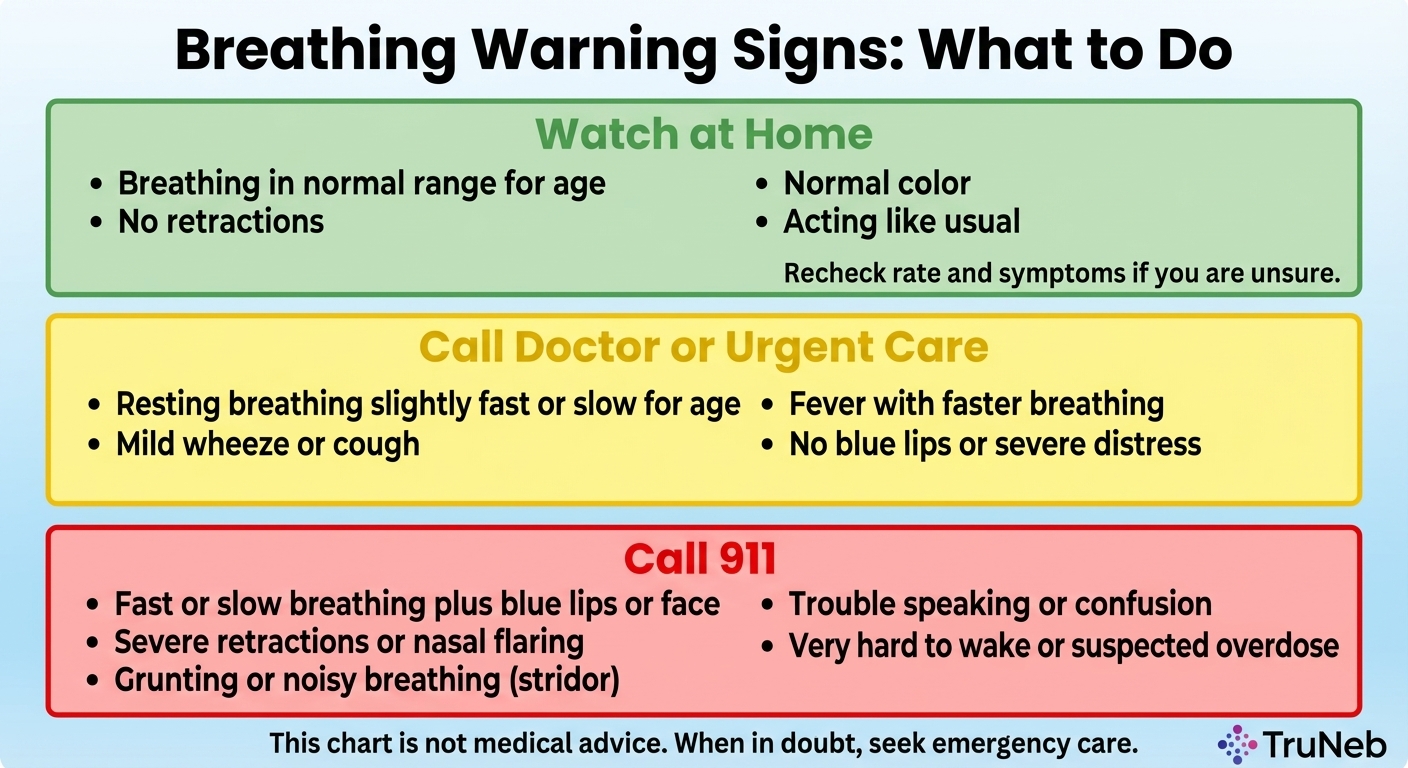
When an Abnormal Breathing Rate Needs Urgent or Emergency Care
Respiratory rate alarm thresholds are most useful when you look at the number and the symptoms together. A slightly high or low rate in a comfortable person can be less urgent than a normal rate in someone who looks very sick.
If someone has fast or slow breathing plus blue lips, severe trouble breathing, confusion, or is hard to wake, call emergency services right away.
Signs That Mean Call a Doctor Soon
Contact your doctor the same day or within a few hours if you notice:
- A resting respiratory rate that stays outside the normal range for age, but the person is still alert and breathing without hard effort
- Fever plus a higher breathing rate in a child, without blue lips or severe distress
- New wheezing or a persistent cough with a slightly higher rate
- A change from baseline in someone with asthma or COPD, such as breathing faster than usual even while using prescribed inhalers or a nebulizer
MedlinePlus and the CDC note that these patterns can be early signs of pneumonia, bronchiolitis, asthma flare, or other illnesses that benefit from prompt evaluation.
Signs That Mean Go to Urgent Care or the ER
Head to urgent care or an emergency department if you see:
- Fast breathing at rest with chest discomfort or pain
- Worsening shortness of breath (dyspnea) when walking across a room or speaking
- Oxygen saturation readings that are low for that person (for example, below about 92 percent if your doctor has given you a target)
- A child who is breathing fast even while calm, especially with retractions or nasal flaring
These signs can point to pneumonia, COPD or asthma exacerbation, heart failure, or another serious problem that needs urgent testing and treatment.
Signs That Mean Call 911 Now
American Lung Association, CDC, and MedlinePlus emergency guidance all emphasize calling emergency services right away if any of these are present:
- Blue, gray, or very pale lips, face, or fingernails (cyanosis)
- Severe retractions (skin pulling in between ribs or at the neck) or belly moving in opposite direction to the chest
- Grunting with each breath or high-pitched noisy breathing (stridor)
- Inability to speak in full sentences or a child who can’t cry due to shortness of breath
- Sudden confusion, agitation, or unresponsiveness
- Suspected overdose from opioids or sedatives, especially with very slow or shallow breathing
- Fast or slow breathing that seems to be getting worse over minutes
These are emergency red flags for respiratory failure. Don’t drive yourself if breathing is very difficult; call for help.
Talk to your doctor about an action plan if you or your child has asthma, COPD, or another chronic lung disease so you know in advance when to call the office, urgent care, or 911. It may also help to review when urgent care makes sense for asthma and the basics of signs of COPD getting worse.
Key takeaway: Fast or slow breathing paired with blue lips, severe effort, trouble speaking, or confusion is a medical emergency and needs 911.
Respiratory Rate in People With Asthma, COPD, and Other Chronic Lung Conditions
For asthma, COPD, and other chronic lung diseases, respiratory rate is one more number to track alongside symptoms and oxygen levels when you’re monitoring at home.
What Baseline Changes Can Happen in Chronic Disease
In asthma, COPD, bronchiectasis, and similar conditions, the airways can be narrower or inflamed even on good days. The American Lung Association and Cleveland Clinic note that some adults with chronic lung disease have a resting rate near the upper end of normal, such as 18 to 22 breaths per minute.
During a flare, the rate can climb higher as breathing gets harder. In COPD, for example, a person who normally rests at 18 can run at 24 to 26 during a mild exacerbation.
Trends matter more than a single number. A steady rise in respiratory rate over several hours or days, especially with more wheezing, cough, or fatigue, can be more meaningful than one isolated reading.
How to Monitor Safely at Home
If you live with asthma, COPD, or another chronic lung condition, your doctor may give you an action plan that includes:
- Checking respiratory rate at rest
- Watching for wheezing, chest tightness, or retractions
- Tracking oxygen saturation with pulse oximetry if prescribed
- Noting triggers such as infections, smoke, or weather changes
Write down your baseline values when you’re well. Then note any changes during flares.
Don’t change steroid doses, inhalers, or other prescription medicines without medical advice. Bring your home records to clinic visits so your doctor can adjust your care safely.
Where Nebulizer Therapy Fits
Many people with asthma or COPD are prescribed inhaled medications, such as bronchodilators or inhaled steroids, to help open airways and reduce inflammation. These can be delivered by metered-dose inhaler, dry powder inhaler, or nebulizer, depending on your care plan. If you are comparing devices, this overview of nebulizer vs inhaler differences may help.
A portable mesh nebulizer like the TruNeb™ portable mesh nebulizer can make it easier to take prescribed nebulized treatments when you’re away from home or when holding and timing a standard inhaler is difficult. TruNeb turns liquid medication prescribed by your doctor into a fine mist you breathe in through a mask or mouthpiece.
Nebulizer therapy can help ease breathing and lower work of breathing during a flare for some people, but only as part of a broader action plan set by your doctor. It’s not a substitute for emergency care or in-person evaluation.
Talk to your doctor before starting nebulized medications, hypertonic saline, or changing doses of any inhaled therapy. They can tell you how and when to use each treatment and what respiratory rate or symptoms should send you to urgent care or the ER. For device-specific setup and technique, see portable mesh nebulizer how to use.
Key takeaway: In chronic lung disease, small day-to-day changes in respiratory rate matter less than clear trends, symptoms, and a plan you build with your doctor.
Frequently Asked Questions
Tap or click a question below to see the answer:
Most healthy adults at rest breathe about 12 to 20 times per minute, according to major medical sources. Some fit adults can rest slightly below 12 without symptoms, but rates under about 10 or over about 24 with distress should be checked by a doctor as they can fall outside the usual adult respiratory rate normal range.
During sleep, an adult’s breathing usually slows toward the lower end of the normal range. A calm sleeping adult might breathe around 10 to 16 times per minute. Very slow, shallow, or irregular breathing with snoring pauses, blue lips, or trouble waking can be a sign of sleep apnea or respiratory depression and needs medical attention.
Fever usually raises respiratory rate in children. A mildly higher rate that stays close to the normal breathing rate for a child’s age and improves as fever drops is common. If a child with fever is breathing much faster than their usual baseline at rest, especially with retractions, nasal flaring, or blue lips, seek urgent care.
Experts recommend counting for a full 60 seconds when you’re concerned. This is especially important in infants, young children, and anyone with irregular breathing, because shorter measurements can miss pauses or bursts and give a misleading respiratory rate.
It depends on age and context. For a calm toddler, 30 breaths per minute can be normal. For a school-age child, it’s at the top of the normal range. For a resting healthy adult, 30 is higher than normal and can signal tachypnea. Use a normal respiratory rate by age chart and always match the number with symptoms.
Both matter, but effort often matters more. A slightly high rate in a comfortable person with normal color can be less urgent than a normal rate in someone with retractions, nasal flaring, grunting, or confusion. Guidelines stress that respiratory distress signs and changes in color or alertness should always be taken seriously.
Yes. Anxiety and panic attacks can cause fast, shallow breathing, chest tightness, tingling lips or fingers, and a feeling of not getting enough air. While anxiety-related tachypnea can ease with calming and slow breathing, it’s safest to rule out lung, heart, or metabolic causes with your doctor.
Worry about a baby breathing fast when the rate is higher than about 60 breaths per minute at rest and is paired with signs of distress such as retractions, nasal flaring, grunting, poor feeding, or blue lips. These can signal bronchiolitis, RSV, pneumonia, or other serious conditions that need urgent care.
Key takeaway: Use age-based ranges as a guide, but always match the number with how hard someone is working to breathe, their color, and how alert they are.
Disclaimer: This article is for informational purposes only and isn’t a substitute for professional medical advice, diagnosis, or treatment. Always talk with your doctor about any questions you have about your symptoms or medications.