On this page

A non-rebreather mask (NRB) is an emergency oxygen mask used for people who are breathing on their own but have very low oxygen levels.
It’s usually set between 10 and 15 liters per minute (L/min) and can deliver about 60–90% oxygen (FiO₂) depending on the fit and the person’s breathing pattern. This non rebreather mask flow rate is much higher than standard home oxygen.
Key point: A non-rebreather mask is among the highest-oxygen standard face masks used for someone who is still breathing on their own, before moving to more advanced support like a bag-valve-mask or a ventilator.
FiO₂ stands for "fraction of inspired oxygen" and simply means the percentage of oxygen in the air someone breathes. Room air is about 21% oxygen. With a well-set NRB mask, you can more than triple that.
This guide walks you through how NRB masks work, the right flow rate to use, when they’re used in emergencies, how they’re set up in medical settings, and how they compare with other oxygen delivery devices.
Talk to your doctor before changing any oxygen settings or starting new respiratory treatments, especially if you have a chronic lung condition like asthma or COPD differences.
⚠️ Seek emergency care right away for severe shortness of breath, blue lips or face, confusion, chest pain, or if someone is struggling to breathe.
Disclaimer: This article is for informational purposes only and is not a substitute for medical advice. Always talk to your doctor about oxygen therapy, breathing treatments, and any changes to your care.
How Does a Non-Rebreather Mask Work?
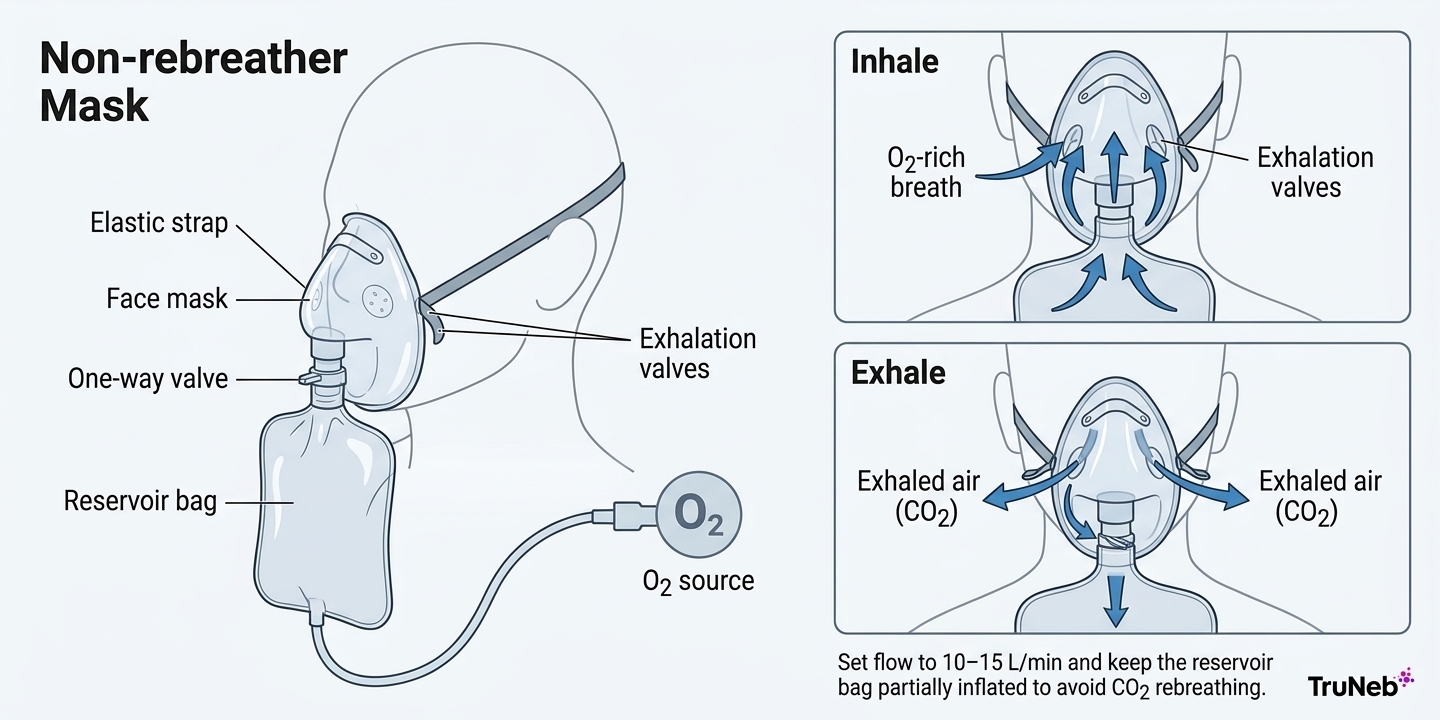
A non-rebreather mask looks simple, but its parts are carefully designed to push oxygen up and keep exhaled air out.
Here’s what you’re seeing when you look at an NRB:
- A clear plastic face mask that covers the nose and mouth
- Soft elastic strap and nose clip to help seal the mask
- A large soft reservoir bag hanging under the mask
- One-way valve between the mask and the bag
- One or two flutter valves over the side ports of the mask
- Oxygen tubing connected to a wall outlet or tank
When the oxygen is turned on, it flows into the reservoir bag and fills it with nearly 100% oxygen. The goal is to keep that bag at least two-thirds full.
On inhalation, the one-way valve between the bag and the mask opens. The person breathes in oxygen from the reservoir bag. At the same time, the flutter valves over the side ports close so room air does not rush in.
On exhalation, the valve to the bag closes. Exhaled air leaves through the side ports, lifting the flutter valves briefly and then closing again. That exhaled air does not go back into the reservoir bag.
Because of this system, the person "non-rebreathes" their own CO₂-rich exhaled air and instead gets a high concentration of fresh oxygen with each breath.
In practice, you rarely reach a perfect 100% oxygen level at the mouth. Some room air can leak in around the mask, and breathing patterns vary, so most sources list the NRB mask FiO₂ range as about 60–90%.
One-line takeaway: A non-rebreather mask uses a reservoir bag plus one-way valves to give much higher oxygen levels than a simple mask, while trying to keep exhaled air from being breathed in again.
Recommended Flow Rate and Oxygen Concentration (FiO₂) for Non-Rebreather Masks
For non-rebreather masks, the flow setting is what makes the mask safe and effective.
Standard NRB flow rate:
- Set between 10 and 15 L/min
- In many emergency settings, the flow is set to 15 L/min to help keep the reservoir bag full
If the flow is set too low, two problems show up:
- The reservoir bag collapses with each breath and may stay flat
- Exhaled carbon dioxide (CO₂) is not flushed out well, so the person can start to rebreathe it
Guidelines warn against using an NRB mask below about 10 L/min. You want to see the reservoir bag remain partially inflated at all times. It should fall a bit when the person breathes in, then refill between breaths.
Typical NRB FiO₂ (oxygen percentage):
- About 60–90% FiO₂ at 10–15 L/min
- Real-world FiO₂ depends on the mask seal, the person’s breathing rate and depth, and whether any valves are removed
For comparison:
- Room air: ~21% oxygen
- Nasal cannula: ~24–44% oxygen (up to 6 L/min)
- Simple mask: ~40–60% oxygen (5–10 L/min)
- Non-rebreather mask: highest FiO₂ of the standard face masks
Key point: A non-rebreather mask should run at high flow (ideally 15 L/min) with a bag that never fully collapses, because that’s how you safely reach the 60–90% oxygen range without causing CO₂ buildup, and the exact oxygen percentage still depends on the fit and breathing pattern.

When and Why is a Non-Rebreather Mask Used?
Non-rebreather masks are reserved for situations where someone is breathing but their oxygen level is very low. They are a short-term rescue tool, not a long-term solution, and they do not treat the root cause of low oxygen by themselves.
Common reasons to use an NRB mask include:
- Severe hypoxemia from lung disease: Very low oxygen levels that may be seen in bad pneumonia, ARDS, or pulmonary edema when simpler devices are not enough.
- Major trauma or shock: After serious injury or blood loss, emergency teams can use an NRB during transport to keep oxygen delivery as high as possible.
- Carbon monoxide poisoning or smoke inhalation: High-flow oxygen via NRB helps clear carbon monoxide from hemoglobin faster and supports damaged lungs.
- Severe asthma or COPD flare: While more advanced treatment might be noninvasive ventilation or intubation, an NRB mask can be used briefly while the team supports the person and treats the flare.
- Cluster headache attacks: In some emergency and neurology settings, doctors use high-flow oxygen through an NRB as one option to help shorten cluster headache attacks.
In most hospitals and EMS systems, the pattern is similar:
- The person is conscious or at least breathing on their own.
- Oxygen saturation is very low or dropping fast.
- The team wants the highest oxygen they can get without immediately using a bag-valve-mask or intubation.
If the person is not breathing adequately, an NRB mask is not enough. In those cases, the care team may move to assisted ventilation with a bag-valve-mask or a ventilator.
One-line takeaway: Think of the non-rebreather mask as a high-oxygen bridge used in ambulances, emergency rooms, and critical care units while the team treats the cause of low oxygen or decides on the next step.
How to Use a Non-Rebreather Mask (Step-by-Step)
Here is a general, step-by-step look at how trained staff set up and monitor a non-rebreather mask in medical settings. This is for education only and does not replace local protocols or professional training.
- Check the oxygen source and equipment
- Confirm the wall outlet or tank is working and has enough oxygen.
- Inspect the NRB mask: tubing connected, reservoir bag intact, one-way valves in place.
- Attach the mask to the oxygen source
- Connect the tubing firmly to the outlet or tank regulator.
- Set the flow to 10–15 L/min. In many clinical settings, staff use 15 L/min to keep the bag well-inflated.
- Pre-inflate the reservoir bag
- Hold a hand lightly over the mask port so air does not escape.
- Let the oxygen fill the reservoir bag until it is at least two-thirds full.
- This helps make sure the first breaths through the mask are oxygen-rich.
- Fit the mask on the patient
- Place the mask over the nose and mouth.
- Use the elastic strap to secure it, then adjust the nose clip so the top edge seals without digging into the skin.
- Check that the reservoir bag hangs freely and is not twisted or trapped.
- Watch the bag and the patient
- With each breath in, the reservoir bag should shrink slightly, then refill.
- If the bag collapses completely, trained staff would increase the flow and check that the oxygen source is working.
- They also monitor comfort, breathing pattern, and oxygen saturation if a pulse oximeter is available.
- Reassess often and be ready to change support
- NRB masks are for short-term use. If oxygen levels do not improve, or the person becomes drowsy or stops breathing well, the care team may move to more advanced breathing support.
- If the person stabilizes, they may be stepped down to a simple mask or nasal cannula for comfort.
Because NRB masks can limit room air if oxygen stops flowing, they should only be used where trained staff can watch the person continuously.
Talk to your doctor about the devices they use and what each one does. Never try to set up or change oxygen equipment at home without direct instructions from a professional.
One-line takeaway: A non-rebreather mask works safely only when trained staff set the oxygen high enough to keep the reservoir bag partially inflated the whole time.
Non-Rebreather vs Other Oxygen Masks
The main difference between oxygen masks is how much oxygen they can deliver and how precisely they control it.
Non-Rebreather vs Simple Face Mask
Non-rebreather mask
- Has a reservoir bag plus one-way valves.
- Flow: 10–15 L/min.
- Approximate FiO₂: ~60–90%.
- Exhaled air leaves through side ports and does not refill the bag.
- Used when the goal is the highest possible oxygen concentration in a breathing patient.
Simple face mask
- Plastic mask without a reservoir bag.
- Side holes stay open to let room air mix in and to vent exhaled gas.
- Flow: 5–10 L/min (kept at least 5 L/min to reduce CO₂ buildup in the mask).
- Approximate FiO₂: ~40–60%.
- Safer if oxygen is interrupted, because room air can still enter freely.
- Used for moderate oxygen needs or during short procedures.
Non-Rebreather vs Partial Rebreather Mask
Partial rebreather mask
- Looks like an NRB but without the one-way valve between mask and bag.
- Some exhaled air flows back into the bag, so the person "partially" rebreathes that gas.
- Flow: typically 6–10 L/min.
- Approximate FiO₂: ~50–70%.
- Less commonly used today; many facilities go directly from simple mask to NRB when they need larger jumps in FiO₂.
In short, simple masks and partial rebreathers sit in the middle range for oxygen delivery. Non-rebreathers sit at the top, but they require high flow and close monitoring because of the one-way design.
Non-Rebreather vs Venturi Mask
Venturi mask (air-entrainment mask)
- Uses a special adapter with small openings that mix oxygen with room air in fixed ratios.
- Each adapter color corresponds to a set FiO₂ (for example 24%, 28%, 35%, 40%, 50%).
- Flow at the wall may be high, but the delivered oxygen percentage stays precise and stable.
- Used when careful oxygen control is more important than very high FiO₂.
Non-rebreather mask
- Uses a reservoir bag filled with near 100% oxygen and one-way valves.
- Flow: 10–15 L/min, FiO₂ around 60–90%, but not exact.
- Best when the priority is the highest possible oxygen, such as major trauma, severe pneumonia, or carbon monoxide exposure.
A simple way to remember it:
- Venturi mask = controlled oxygen for fine-tuning.
- Non-rebreather mask = maximum oxygen for emergencies.
Clinicians choose between these masks based on the person’s condition, blood gases, and how tightly they want to control oxygen levels. If you want context on lower-range home therapy, see this guide to oxygen use in COPD.
Why Non-Rebreather Masks Are Not for Home Use
It might seem logical to think, "If this mask gives such high oxygen, why not use it at home?" But non-rebreather masks are not designed or approved for unsupervised home oxygen.
Here’s why:
1. They need very high oxygen flow
Most home oxygen concentrators top out at about 5–10 L/min. A non-rebreather needs 10–15 L/min just to work safely. If the flow is too low, the reservoir bag flattens and CO₂ can build up.
2. The one-way valves can limit room air
If the oxygen source suddenly stops while someone is wearing an NRB mask with tight straps, the one-way design may slow or block room air from getting in. In a hospital, staff are watching and can respond. At home, that could become dangerous quickly.
3. Home oxygen has different goals
At home, oxygen therapy is usually about gently keeping levels in a safe range over hours, days, and months. This is done with nasal cannulas or simple masks at lower flow rates, not emergency-level oxygen bursts.
For people who need oxygen at home, doctors will prescribe a specific device and flow setting. That might include:
- A nasal cannula connected to a concentrator
- A simple mask for short periods
If you use home oxygen now and feel more short of breath, do not try to "upgrade" your own equipment. Call your doctor or oxygen provider. Changes in breathing can signal an infection, a flare-up of COPD or asthma, or another issue that needs medical care. If you monitor at home, understanding pulse oximeter reading ranges may help you know when to seek care.
Talk to your doctor before trying any new oxygen device or changing your flow rate. Using the wrong setup at home can cause harm, even if it looks similar to hospital equipment.
One-line takeaway: Non-rebreather masks are not designed for home use because they need high oxygen flow and close monitoring to stay safe.
Oxygen Masks vs Nebulizers – Different Roles in Respiratory Care
Oxygen masks and nebulizers often sit side by side in emergency rooms and clinics, but they do two very different jobs.
What oxygen masks do
- Deliver extra oxygen gas to the lungs
- Raise blood oxygen levels when they drop too low
- Examples: nasal cannula, simple mask, non-rebreather mask, Venturi mask
These devices do not contain medicine by themselves. They simply change how much oxygen you breathe in, and they support low oxygen levels without fixing the underlying cause.
What nebulizers do
- Turn liquid medication or saline into a fine mist you inhale
- Help open narrowed airways, thin mucus, and reduce swelling in the lungs
- Commonly used for conditions like asthma, COPD, and cystic fibrosis
Nebulizers do not usually boost oxygen levels directly. Instead, they make it easier to move air in and out, which can improve how you feel and how well your lungs work over time.
For many people with chronic lung disease, the pattern looks like this:
- In a flare or emergency, hospital teams may use high-flow oxygen devices (like a non-rebreather mask) to support low oxygen levels.
- For daily control at home, they use inhalers or nebulizers to deliver medicines that keep airways as open and clear as possible.
A portable mesh nebulizer can be especially helpful for people who need treatments on the go, at work, or during travel. The TruNeb portable mesh nebulizer is one example of this type of device that can deliver prescribed medications or saline without a large tabletop machine.
Oxygen therapy and nebulizer therapy often work together: oxygen for low levels in a crisis, nebulizers for long-term airway care between flare-ups. To compare delivery options, you can also review nebulizer vs inhaler differences and learn using a nebulizer with oxygen.
Always follow your doctor’s exact instructions on which medications to nebulize, how often to use them, and when to seek urgent care instead of treating at home. Do not start, stop, or mix nebulized medicines or oxygen equipment on your own without medical guidance. For maintenance and safety, see nebulizer cleaning instructions and how to use a nebulizer.
One-line takeaway: Oxygen masks raise oxygen levels, while nebulizers deliver medicine or saline to the lungs.
| Device | Typical flow (L/min) | Approx. FiO₂ | Best for |
|---|---|---|---|
| Non-rebreather mask | 10–15 | ~60–90% | Short-term emergencies when very low oxygen needs rapid support |
| Partial rebreather mask | 6–10 | ~50–70% | Medium-to-high oxygen needs when NRB is not required |
| Simple face mask | 5–10 | ~40–60% | Moderate oxygen needs or short procedures |
| Venturi mask | 2–15 (set by adapter) | 24–50% (precise) | Situations where oxygen must be tightly controlled, such as some COPD cases |
Frequently Asked Questions
Tap or click a question below to see the answer:
A non-rebreather mask is usually run between 10 and 15 L/min of oxygen. In many emergency settings, staff use 15 L/min so the reservoir bag stays partially inflated and the person gets a high FiO₂ without rebreathing CO₂.
When used correctly at 10–15 L/min with a decent seal, a non-rebreather mask typically delivers about 60–90% oxygen. The exact FiO₂ varies with mask design, fit, and how the person is breathing.
If the oxygen flow is too low, the reservoir bag can flatten and exhaled CO₂ is not washed out. The person can then rebreathe that exhaled air instead of getting fresh oxygen, which reduces the benefit of the mask and may be unsafe.
Non-rebreather masks are not meant for unsupervised home use. Most home concentrators cannot provide the high flow they need, and the one-way valves can limit room air if oxygen stops. Follow your doctor's prescription, which usually involves a nasal cannula or simple mask at home.
Both masks have reservoir bags, but a partial rebreather does not have a one-way valve between the bag and the mask. Some exhaled air goes back into the bag, so its FiO₂ is lower (around 50–70%), while a non-rebreather can reach roughly 60–90% because it keeps most exhaled air out of the reservoir.
The gas inside the reservoir bag is close to 100% oxygen, but a small amount of room air usually leaks in around the mask edges. In real use, this is why most sources quote about 60–90% as the realistic FiO₂ range.
Your doctor and hospital team choose oxygen devices based on your vital signs, blood tests, diagnosis, and how stable you are. If you are unsure why a certain mask or flow rate is being used, it is always okay to ask them to explain.
No. Do not start, stop, or adjust oxygen devices or nebulized medications without talking to your doctor. They can tell you which tools and doses are safe for your lungs and when you need urgent in-person care instead of home treatment.