On this page

How Fast Can You Really Get Over Bronchitis?
Disclaimer: This article is for informational purposes only and is not a substitute for medical advice, diagnosis, or treatment. Talk to your doctor about symptoms, medications, and treatment decisions.
⚠️ Seek emergency care right away if you have severe trouble breathing, bluish lips or face, severe chest pain, confusion, or you cannot speak in full sentences.
Bronchitis can feel miserable when you are in the middle of it. The deep cough, the burning chest, the nonstop mucus all make you want a cure right now.
Here is the honest answer: there is no instant cure for acute bronchitis. This article focuses on acute bronchitis, which is a short-term infection and inflammation of the airways, not chronic bronchitis. Most cases are caused by viruses from a cold, flu, COVID-19, or another respiratory infection, so your immune system has to clear the infection on its own. Antibiotics do not kill viruses and usually do not help recovery in acute viral bronchitis.
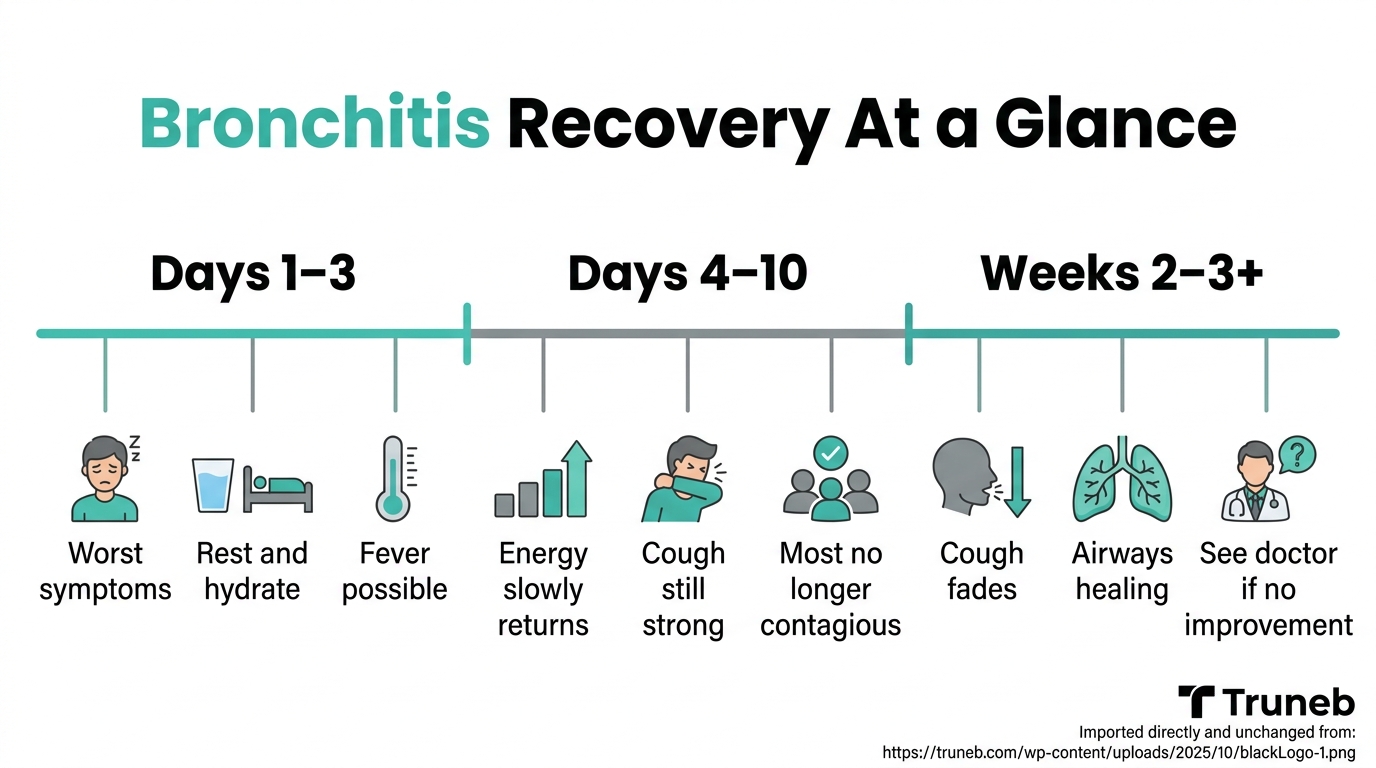
Key point: Acute bronchitis usually gets better on its own in 2 to 3 weeks, but the cough can last longer while the airways heal.
During the first few days, bronchitis often feels like a bad chest cold. You may have a low-grade fever, body aches, fatigue, and a cough that keeps getting worse. Around day 4 to 7, other symptoms usually start to ease, but the cough and tiredness can still be strong. By week 2, many people feel much better, even if they still cough.
Bronchitis itself is not contagious, but the virus that triggered it is. You can usually spread that virus for a few days up to about a week, similar to a cold or flu. That is why staying home and resting early on protects both you and the people around you.
Bronchitis and pneumonia can share some symptoms, but they are not the same. Pneumonia is a deeper lung infection that more often causes high fever, chills, and trouble breathing, and it needs prompt medical attention. For a closer comparison, see our guide on bronchitis versus pneumonia differences.
So you cannot flip a switch and erase bronchitis overnight. But you can do a lot to feel better faster, breathe easier, and avoid making it worse. This guide explains how to cure bronchitis fast in a realistic way, meaning how to recover as quickly and safely as possible.
Talk to your doctor before trying a new medication or if your symptoms are getting worse instead of better.
Day 1 and Day 2: The Fast Relief Game Plan
The first 48 hours can influence how you feel over the next couple of weeks. Pushing through work or ignoring symptoms can make bronchitis feel worse. Giving your body what it needs early can help you feel better and support recovery.
Rest comes first. Your immune system does its best work when you slow down. If you can, take it easy for a day or two, rest more than usual, and hold off on strenuous exercise or heavy chores. Even one or two true rest days can help you feel better and may support recovery.
Next, start drinking more fluids right away. Aim for frequent sips through the whole day rather than chugging a big glass once in a while. Water, warm herbal tea, broth, and diluted juice all count. Staying well hydrated can make thick mucus easier to cough up, which helps your airways stay clearer.
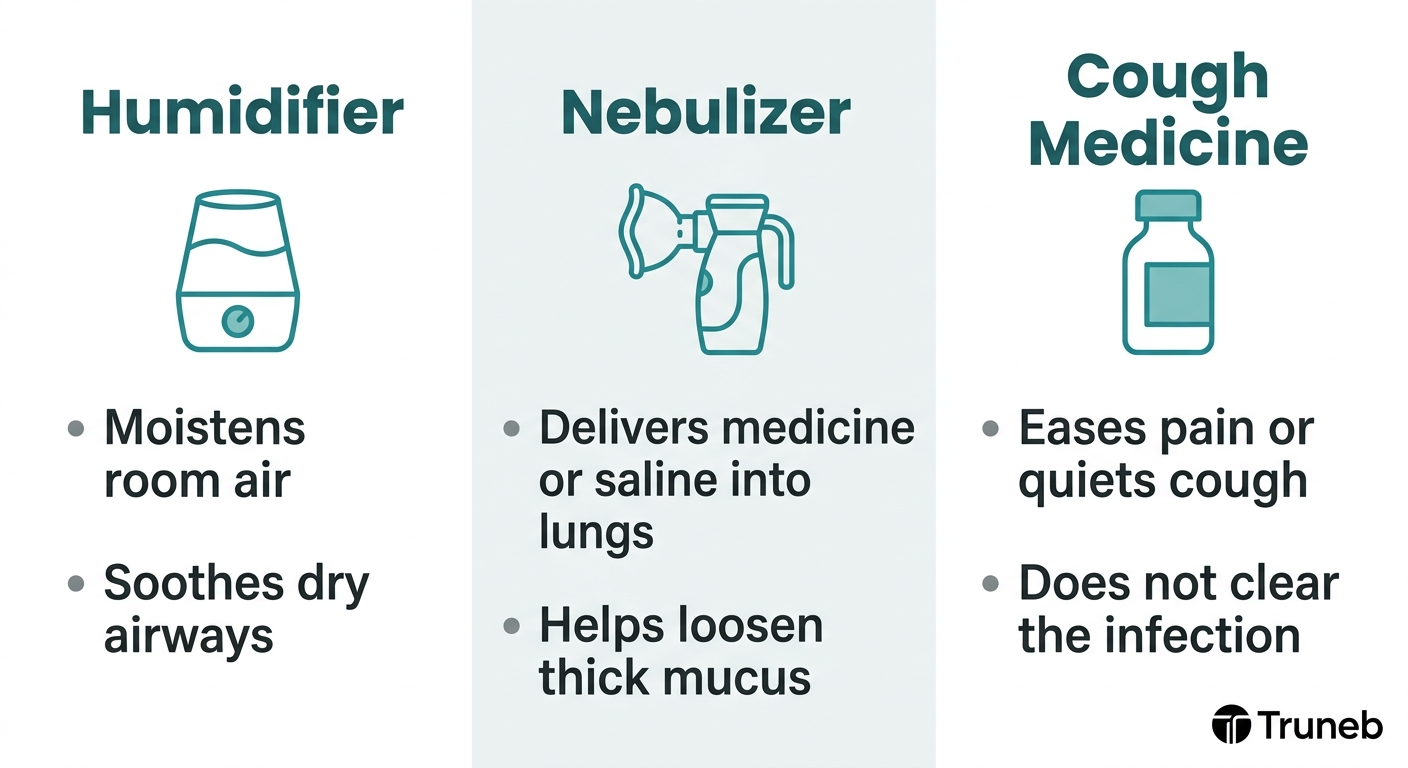
Moist air can also make breathing more comfortable. Set up a cool-mist humidifier where you sleep or rest and keep it running, making sure it is clean. If you do not have one, you can try steam. Sit in a steamy bathroom with the shower running or sit near a bowl of warm (not boiling) water and breathe the mist for a few minutes at a time. Be careful around hot water and steam so you do not get burned.
At the same time, protect your lungs from anything that makes them work harder. Do not smoke. Stay away from secondhand smoke, strong cleaning fumes, and dusty rooms. If you must go out in cold air, wrap a scarf loosely over your nose and mouth to warm the air before it hits your chest.
If you have a mild fever or body aches, over-the-counter pain relievers like acetaminophen or ibuprofen can take the edge off so you can rest. Follow the label directions and avoid taking more than one product with the same ingredient.
Early bronchitis care focuses on rest, fluids, moist air, and avoiding smoke or other lung irritants. If you are comparing devices, our article on nebulizer versus humidifier differences can help clarify which tool does what.
Daytime Home Remedies That Actually Help
During the day, your main goals are to keep mucus moving, calm irritation, and stay as comfortable as possible while your body fights the infection.
Let your cough do its job. A bronchitis cough feels miserable, but coughing is how your lungs clear out mucus. In general, you want a loose, productive cough during the day, not a completely silent chest. Sit upright rather than flat when you can, and take a few deeper breaths now and then to help bring mucus up. If it is safe and comfortable, gentle walking around the house can also help keep secretions from settling.
Soothing your throat makes coughing less rough. Simple tools work well here:
Use honey to coat and calm your throat. A spoonful of plain honey or honey stirred into warm herbal tea can reduce coughing and ease soreness, especially in older kids and adults. Do not give honey to children under 1 year old.
Warm saltwater gargles can soothe an irritated throat. Dissolve a small amount of salt in a glass of warm water, gargle, and spit it out. You can repeat this a few times a day if it feels helpful.
Sip warm liquids through the day. Ginger, chamomile, or peppermint tea with lemon and a little honey gives you fluids, warmth, and a soothing coating all at once. Ginger and turmeric are natural spices that many people use in teas or soups for comfort and general anti-inflammatory support, but they are not proven treatments for bronchitis itself.
Lozenges or cough drops with menthol or eucalyptus can briefly numb an irritated throat and quiet mild coughing fits. Let them melt slowly rather than chewing them. For kids, check the age recommendations and avoid hard lozenges in very young children because of choking risk.
Keeping your nose clear also matters. Saline nasal sprays or drops help wash out mucus in your nose, which can reduce postnasal drip that triggers more coughing.
Some people also use steam or warm mist during the day, similar to the first 48-hour plan, to feel more comfortable. Steam inhalers are not the same as nebulizers and are not for breathing in medications. If you want a detailed comparison, read our guide on nebulizer versus steam inhaler.
Key point: The best home remedies for bronchitis help loosen mucus and calm irritation rather than stop every cough.
Which Medicines Help Bronchitis - And Which Do Not
Over-the-counter medicines can make bronchitis more bearable, but they do not cure the infection itself. Choosing the right ones for your symptoms matters.
Expectorants such as guaifenesin (found in products like Mucinex) are used to thin and loosen mucus so it is easier to cough up. They do not stop the cough. That is usually a good thing during the day, because you want to clear your lungs. Staying well hydrated overall can also help mucus stay thinner.
Cough suppressants with dextromethorphan (often labeled DM) can quiet a harsh, dry cough for a few hours. These are most useful at night when you need to sleep. If you use them in the daytime, keep it limited so you are not completely blocking a productive cough. Always follow the dosing instructions and avoid using adult cough medicines in young children.
Pain and fever reducers like acetaminophen or ibuprofen help with chest soreness from coughing, headaches, and low-grade fevers. Bringing a fever down and easing aches can help you rest, eat, and drink, which supports your immune system. Check labels so you do not double up on the same ingredient in more than one product.
If you feel wheezy or tight in the chest, doctors sometimes prescribe a bronchodilator such as an albuterol inhaler. These medicines relax the muscles around your airways so air can move more freely. They are usually prescribed if you have asthma, COPD, or if your bronchitis is causing clear wheezing. If you have questions about side effects, our article on common albuterol side effects may be helpful.
Steroid medicines are not routinely used for simple acute bronchitis, but doctors may prescribe them for people with asthma, COPD, or significant airway inflammation to help calm swelling in the airways.
Antibiotics are the most common thing people ask for and the least likely to help. Acute bronchitis is almost always caused by viruses, so antibiotics like amoxicillin or azithromycin usually do not help recovery in acute viral bronchitis and can cause side effects. Doctors reserve antibiotics for the rare cases where a bacterial infection is suspected, such as whooping cough (pertussis), or for people at higher risk of complications.
In short, use expectorants to help your cough work better, pain relievers to stay comfortable, and cough suppressants only when the cough is stopping you from sleeping. Skip antibiotics unless your doctor clearly explains why you need them.
Over-the-counter medicines can ease bronchitis symptoms, but they do not cure the infection itself.
Talk to your doctor or pharmacist before combining medicines, and do not change any prescription treatments without medical advice.
Nighttime Bronchitis Cough: How to Sleep Better
Night can be the hardest part of bronchitis. Lying down lets mucus pool, your throat dries out, and every tickle can turn into another coughing fit. Better nights usually mean you feel stronger during the day, so it is worth building a bedtime routine that calms your chest.
Start by changing your sleep position. Instead of lying flat, prop yourself up with extra pillows or a wedge so your upper body is raised. Some people find it easier to sleep in a recliner chair for a few nights. Elevation helps mucus drain and reduces that feeling of choking or needing to cough the second you lie back.
Run a cool-mist humidifier in your bedroom at night. Clean, moist air keeps your airways from drying out, which can trigger coughing. If you do not own a humidifier, a warm, steamy shower before bed and breathing the warm mist can loosen mucus just before you lie down.
About 30 minutes before bedtime, combine a soothing drink and any cough medicine you and your doctor have decided is right for you. A warm, caffeine-free tea with a spoonful of honey can coat your throat and reduce irritation. If your cough is so strong that you cannot fall asleep, this is also the time to use a cough suppressant with dextromethorphan, as directed on the label or by your doctor. Using it mainly at night lets your cough stay productive during the day while giving you a break to rest.
Mentholated vapor rubs on your chest or throat can help some people breathe more easily at night. The cooling feeling and vapors may ease coughing enough to drift off. Do not apply thick layers or use adult-strength vapor rubs on very young children.
Keeping your room slightly cool, dark, and quiet, or using gentle white noise, can also make it easier to relax. A calm mind often means fewer tight muscles and less coughing.
Good sleep supports recovery when you have bronchitis by helping your body fight the infection and repair your airways.
Sleeping slightly upright, keeping the air moist, and using soothing remedies before bed can help reduce nighttime coughing.

How Nebulizers Can Help You Breathe Easier
Most people think of nebulizers only for asthma, but they can also play a role in bronchitis care in the right situation.
A nebulizer is a small device that turns liquid medicine or saline into a fine mist you breathe in through a mouthpiece or mask. Because the mist goes straight into your airways, it can be helpful if you are wheezing, very tight in the chest, or struggling with thick mucus.
Doctors sometimes prescribe bronchodilator medicines like albuterol to use in a nebulizer when bronchitis causes bronchospasm, which means the muscles around the airways tighten and narrow. This medicine relaxes those muscles so air can move more freely. It is often used if you already have asthma or COPD and a chest infection has made your breathing worse.
Some clinicians also recommend nebulized saline, including hypertonic saline (a saltier solution), to help thin very sticky mucus. Breathing in this salty mist is sometimes used to help loosen mucus and may increase coughing during the treatment as mucus moves. That extra coughing is part of how your body clears mucus from the airways.
Portable mesh nebulizers have made these treatments easier to do at home. A device like the TruNeb portable mesh nebulizer is quiet, battery-powered, and small enough to carry in a bag. Portable mesh nebulizers can be more convenient for home use or travel than larger tabletop machines.
Only use medications or saline solutions that were made for nebulizer use and approved by your doctor. Do not try to nebulize essential oils, homemade mixtures, or anything not designed for inhalation. Always follow the instructions on how to clean and dry your nebulizer so each treatment stays safe. For added safety, see our guide on how to clean a nebulizer.
A nebulizer does not cure bronchitis, but in selected cases it can help deliver saline or prescribed medicine directly into the airways to ease breathing.
If you feel very congested, have known lung disease, or have been given an inhaler but still feel tight, ask your doctor whether nebulized treatments could help in your specific case. For some people, they become a useful tool to breathe easier while bronchitis runs its course.
Bronchitis Red Flags: When To Call a Doctor or Go to the ER
Most cases of acute bronchitis can be managed at home, but some symptoms mean you need medical help.
Call your doctor or go to urgent care if:
- You have a fever higher than about 100.4°F (38°C) that lasts more than a couple of days, or a new fever appears after you first started to improve.
- Your cough is not improving at all after 2 to 3 weeks, or it suddenly gets much worse after seeming better.
- You feel short of breath with everyday activities, or you hear yourself wheezing even when you are resting.
- You have a history of asthma, COPD, heart disease, or a weak immune system and bronchitis symptoms are hitting harder than usual.
Go to the emergency room or call emergency services right away if:
- You are struggling to breathe, cannot speak in full sentences, or feel like you cannot catch your breath.
- Your lips, face, or fingertips look bluish or gray.
- You have chest pain that is severe, crushing, or gets worse when you take a deep breath.
- You are coughing up more than just small streaks of blood.
- You feel confused, very dizzy, or your heart is racing while you are just sitting still.
These signs can point to pneumonia, a serious asthma or COPD flare, a blood clot, or another urgent problem that needs fast treatment. Symptoms that get worse again after first improving can also be a warning sign of pneumonia or another infection.
If you get bronchitis over and over, or you cough for more than 8 weeks, schedule an appointment even if you feel okay otherwise. Your doctor may want to check for chronic bronchitis, asthma, or other lung issues.
Bronchitis symptoms that get worse instead of better, especially trouble breathing or chest pain, need medical attention.
When you are not sure, it is always safer to get checked than to wait and hope a serious problem goes away on its own.
How To Avoid Future Bronchitis Flares
Once you start feeling better, it is worth thinking about how to make bronchitis less likely next time. You cannot dodge every cold or virus, but you can lower your risk of a chest infection turning into another long, miserable cough.
If you smoke, quitting is the single most powerful step you can take. Cigarette smoke irritates and damages the lining of your bronchial tubes, making them more likely to get inflamed and infected. Even cutting back heavily is a start, but full quitting gives your lungs the best chance to stay clear.
Staying up to date with vaccines also helps. A yearly flu shot lowers your chance of getting influenza, which is a common trigger for bronchitis. Talk with your doctor about whether you should have the COVID-19 vaccine or booster, the pertussis (whooping cough) booster, or pneumonia vaccines based on your age and health.
Good everyday habits protect your lungs too. Wash your hands often, especially during cold and flu season. Try not to be very close to people who are actively coughing or obviously sick. If you work around dust, smoke, or chemical fumes, wear proper protective gear and take breaks in cleaner air.
Keeping your overall health strong makes you more resilient. Aim for regular movement like walking, gentle cardio, or light strength work once you are recovered. Eat a balanced diet rich in fruits, vegetables, and lean proteins. Try to get enough sleep most nights, since chronic sleep loss can weaken your immune response.
If you have asthma, COPD, or another lung condition, follow your action plan and use prescribed inhalers or nebulizer treatments as directed. Well-controlled baseline lung disease often means milder and shorter bronchitis episodes when viruses do strike. If bronchitis keeps coming back, your doctor may want to check for chronic bronchitis or COPD. You can also browse respiratory education and support resources on the TruNeb homepage.
You cannot completely guarantee you will never get bronchitis again. But by protecting your lungs and immune system, you can often make infections less frequent, less severe, and easier to shake.
Avoiding smoke, staying up to date on vaccines, and protecting your lungs can lower the risk of future bronchitis episodes.
Bronchitis FAQs
Frequently Asked Questions
Tap or click a question below to see the answer:
The inflammation in your lungs is not contagious, but the virus that caused it is. You can generally spread those germs for a few days up to about a week, similar to a cold or flu. Staying home, washing your hands, and covering coughs in that period helps protect others.
Not automatically. Green or yellow mucus can happen with viral bronchitis as white blood cells fight the infection. Antibiotics usually do not help unless your doctor finds clear signs of a bacterial infection.
Sometimes. If the infection moves deeper into the lungs or your body has trouble fighting it off, pneumonia can develop. Watch for high fever, worsening shortness of breath, chest pain, or feeling much sicker instead of slowly better — those are reasons to see a doctor quickly.
Many people feel ready to return once their fever has been gone for at least 24 hours and their energy is starting to come back. You may still have a cough, and that is okay, but if you are still very short of breath or feeling awful, an extra rest day can help.
These quick answers cover the most common bronchitis questions readers ask after the main guide.
Talk to your doctor before starting or changing any medications, and get urgent help if your breathing suddenly gets worse or you notice any of the red-flag symptoms above.