On this page
What Are Empyema and Lung Abscess? Key Differences Defined
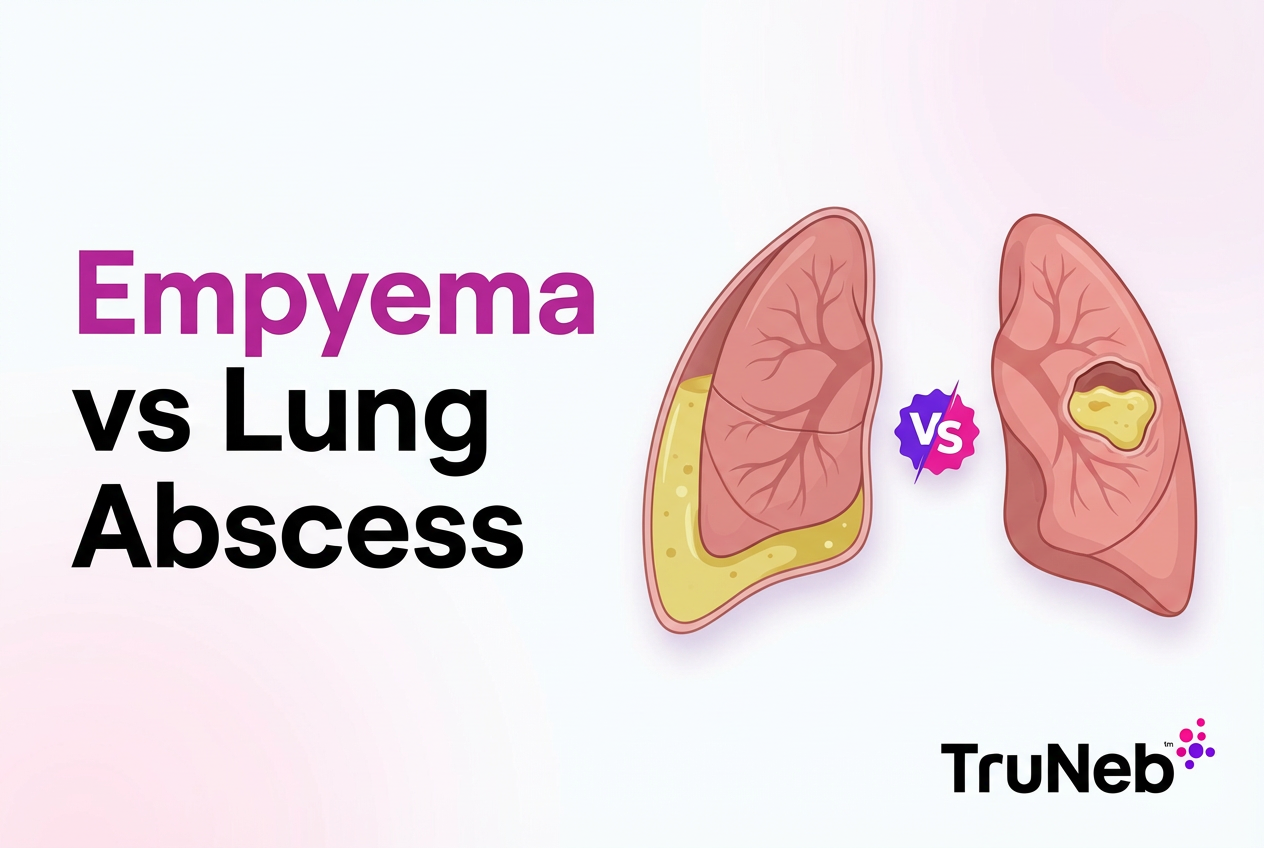
Empyema means a pocket of pus in the pleural space, the thin lining around your lung and chest wall. It’s also called pleural empyema or pyothorax.
A lung abscess is a cavity of pus inside the lung tissue (lung parenchyma).
Although the names sound similar, an empyema is not the same as a lung abscess—it forms around the lung instead of inside it. Because they sit in different places, doctors use different tests and treatments.
Key point: Empyema is pus around the lung, while a lung abscess is pus inside the lung, and that location difference drives how doctors treat them.
Empyema vs Lung Abscess: At a Glance
Empyema vs lung abscess at a glance: location drives symptoms, imaging, and treatment.
| Aspect | Empyema | Lung abscess |
|---|---|---|
| Location | Pus in pleural space (around the lung) | Pus in lung parenchyma (inside the lung) |
| Typical cause | Complicated pneumonia with infected pleural fluid (parapneumonic effusion) | Aspiration of mouth bacteria or severe necrotizing pneumonia |
| Notable symptom | Sharp chest pain with deep breaths, shortness of breath | Cough with large amounts of foul-smelling sputum |
| Imaging clue | Lenticular pleural fluid, split pleura sign on CT, obtuse angle with chest wall | Thick-walled cavity with air–fluid level, acute angle with pleura |
| Treatment | Chest tube/surgery to drain + antibiotics | Antibiotics first; procedures only if not improving |
| Usual outcome | More serious if treatment is delayed; can require procedures | Usually heals with medicine over several weeks |
Key point: Around the lung usually needs drainage; in the lung usually needs antibiotics.
Causes and Risk Factors
Lung abscess:
- Most start after aspiration. Food, stomach contents, or saliva slip into the airway during sleep, seizures, heavy alcohol use, or swallowing problems. This is often called aspiration pneumonia when the infection starts after material is inhaled into the lungs. Mouth bacteria, especially anaerobic bacteria from the gums and teeth, then infect the lung.
- Risks include poor dental hygiene, alcohol misuse, stroke, dementia, sedating medicines, and conditions that raise aspiration risk.
- Some follow severe bacterial pneumonia or happen behind a blocked airway.
Empyema:
- Most are a complication of pneumonia. Fluid collects around the lung (a parapneumonic effusion) and then becomes infected.
- Risk rises with delayed or severe pneumonia, a weakened immune system, diabetes, or after chest surgery or trauma.
In short: Abscesses follow aspiration into the lung; empyemas form when infected fluid collects around the lung.
Symptoms of Empyema vs Lung Abscess
Shared signs: fever, chills, cough, and fatigue are common in both.
Lung abscess:
- Cough with foul‑smelling, pus‑like sputum. Odor points to anaerobic mouth bacteria.
- Symptoms can build over days to weeks. Night sweats and weight loss can happen.
- Chest pain is usually mild unless the cavity sits near the pleura.
Empyema:
- Sharp chest pain with breathing (pleuritic pain) and shortness of breath.
- Patients usually look sicker and breathe fast and shallow.
- On exam, one side can have reduced breath sounds and dullness from fluid.
- People with empyema often get suddenly worse a few days into pneumonia, with new sharp chest pain and breathlessness.
Rule of thumb: Foul‑smelling sputum points toward a lung abscess, while sharp chest pain with breathing and shortness of breath point toward an empyema.
⚠️ Seek emergency care right away if you or someone you’re caring for has severe chest pain, trouble breathing, confusion, or blue lips or face.
Diagnosis: How Doctors Tell Them Apart
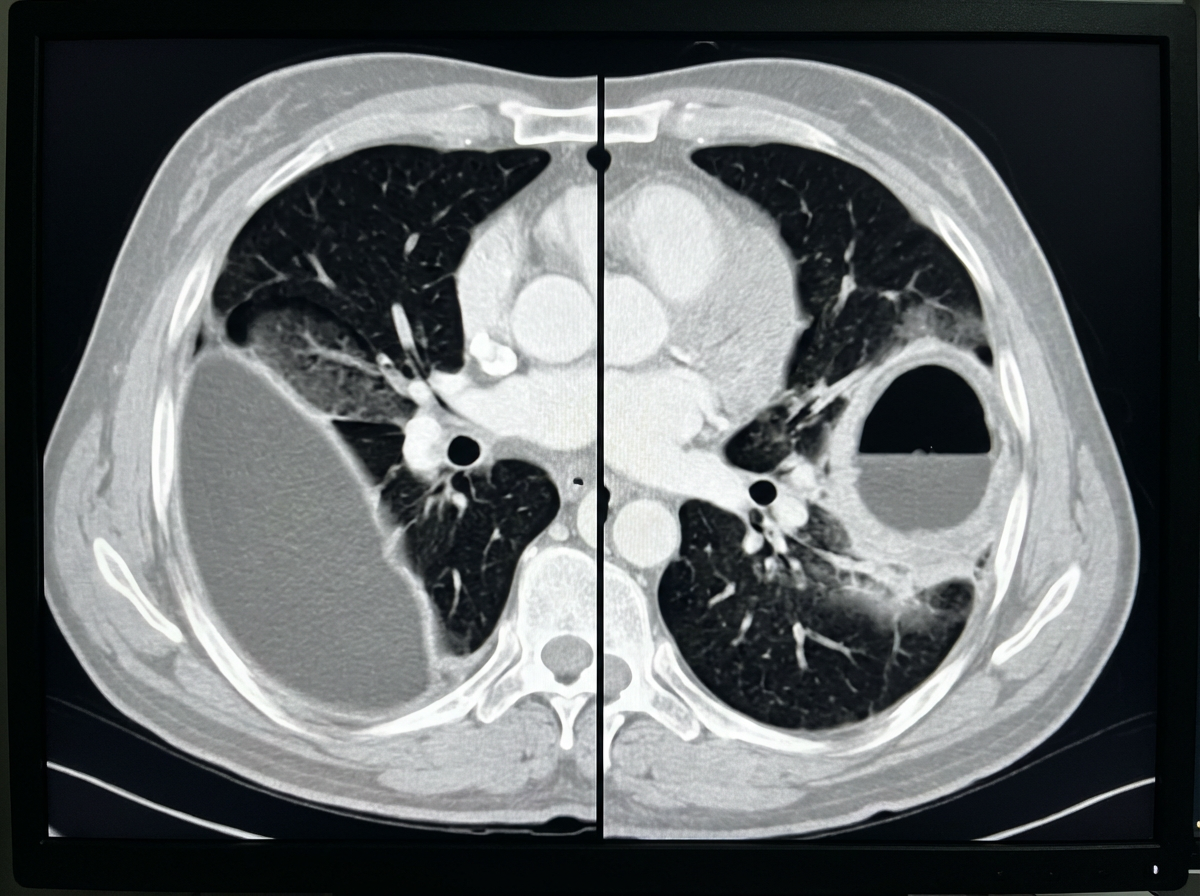
Doctors usually start with a chest X‑ray and ultrasound, which can also show whether the pleural fluid is simple or has pockets and strands that suggest empyema. An abscess can show a cavity with an air–fluid level. An empyema looks like pleural fluid that layers with a curved top (meniscus).
Chest CT is the clearest test. On CT, an empyema is a lens‑shaped pleural collection that compresses the lung. The split pleura sign (both pleural layers enhancing around the fluid) supports empyema. A lung abscess is a thick‑walled cavity inside lung tissue, typically with a visible air–fluid level and sharp angles where it meets the pleura.
If empyema is suspected, thoracentesis (drawing out fluid) can confirm pus and guide antibiotics. For abscess, sputum cultures or bronchoscopy help identify germs and check for a blockage.
Key point: CT shows whether pus is around the lung or inside the lung, and that difference guides treatment.
Treatment and Management
Empyema: pus in the pleural space almost always needs to be drained by a doctor. Doctors place a chest tube to remove infected fluid and give IV antibiotics. If the pus is thick or stuck in pockets, they sometimes use intrapleural medicines (fibrinolytics) through the tube to help thin and break up the fluid, or do minimally invasive surgery (VATS) to clean the space and help the lung re‑expand. Doctors also repeat imaging to confirm the pleural space is clear and the lung has re‑expanded.
Lung abscess: most heal with several weeks of antibiotics that cover the likely germs. The cavity usually drains into the airway on its own as you cough. Procedures are uncommon and reserved for very large cavities, poor response to medicine, or a blocked airway.
Why this matters: antibiotics alone usually can’t clear a large pocket of pus around the lung, but they can clear a pocket inside the lung.
Safety note: This information is general. Talk to your doctor before starting, stopping, or changing any medication.
Key point: Empyema almost always needs drainage plus antibiotics; a lung abscess usually improves with antibiotics alone.
Prognosis and Complications
Lung abscess: with the right antibiotics and follow‑up, most people recover. Reported mortality is very low. Possible problems include coughing up blood, a connection from lung to pleural space (bronchopleural fistula), or chronic infection if not treated.
Empyema: more serious overall, especially if drainage is delayed. Studies show empyema has a noticeably higher in‑hospital death rate than a simple lung abscess, even with modern care. Complications include a thick pleural peel that traps the lung (fibrothorax), infection tracking to the chest wall (empyema necessitans), and sepsis.
Both improve fastest with early, appropriate care and follow‑up imaging to confirm resolution.
Key point: Empyema carries higher short‑term risk; most lung abscesses heal with medicine and time.
Recovery and Prevention: Aftercare for Your Lungs
- Complete your treatment plan and show up for check‑ins. Your team can order a follow‑up chest X‑ray or CT to confirm healing.
- Breathing exercises, such as using an incentive spirometer and doing deep‑breathing practice, are commonly used to help re‑expand lung areas after illness or drainage. Your doctor can show you how to do these safely.
- Clear mucus. If you have lots of phlegm or chronic lung disease, your doctor can recommend airway clearance like chest physiotherapy, positions that help drain mucus, or inhaled therapies to thin secretions.
- Nebulized options. When prescribed, inhaling sterile hypertonic saline (3% or 7%) through a quality device can help loosen mucus so it’s easier to cough out. A portable mesh nebulizer like the TruNeb™ device can make at‑home treatments convenient and quiet when your doctor prescribes nebulized medicine or saline. Use any nebulized medicine only under medical guidance.
- Prevent the next infection. Don’t smoke. Keep good oral hygiene to lower aspiration risk. Avoid lying flat right after eating if swallowing is hard. Stay current on pneumococcal and flu vaccines. Manage conditions like diabetes and COPD.
Talk to your doctor before trying a new medication or starting any nebulized treatment.
⚠️ Contact your doctor promptly if your fever returns, your breathing worsens, or your cough and sputum suddenly get worse instead of better.
Key point: Finish care, clear mucus under guidance, and prevent aspiration to lower the chance of repeat problems.
Frequently Asked Questions
Tap or click a question below to see the answer:
Yes. If an abscess ruptures into the pleural space, pus can spill around the lung and create an empyema. This needs prompt care.
Empyema is usually more urgent because it compresses the lung and typically needs drainage with a chest tube. A lung abscess is serious too, but most improve with antibiotics alone.
Imaging, especially CT, shows where the pus is. Fluid testing (thoracentesis) confirms empyema. Clinical clues help: foul sputum leans toward abscess; sharp chest pain with breathing and a pleural collection lean toward empyema.
Usually no. Procedures are for very large cavities, lack of improvement, or a blocked airway. Most abscesses resolve with medicine and time.
Treat pneumonia early, avoid aspiration, keep good oral care, don’t smoke, and stay up to date on vaccines. Manage any chronic lung or swallowing problems with your care team.
Key point: An abscess can rupture and cause an empyema; CT and fluid testing confirm the difference and guide treatment.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always talk with your doctor about your symptoms, questions, and treatment options.