On this page

ALS Breathing Problems: What Actually Changes First
ALS affects breathing by weakening the muscles that move air in and out, not by damaging the lungs. Early changes can be subtle, and your care team has tools to help. This guide walks through early signs, how doctors check breathing, airway clearance tools (including nebulizers), NIV/BiPAP, tracheostomy choices, and daily tips.
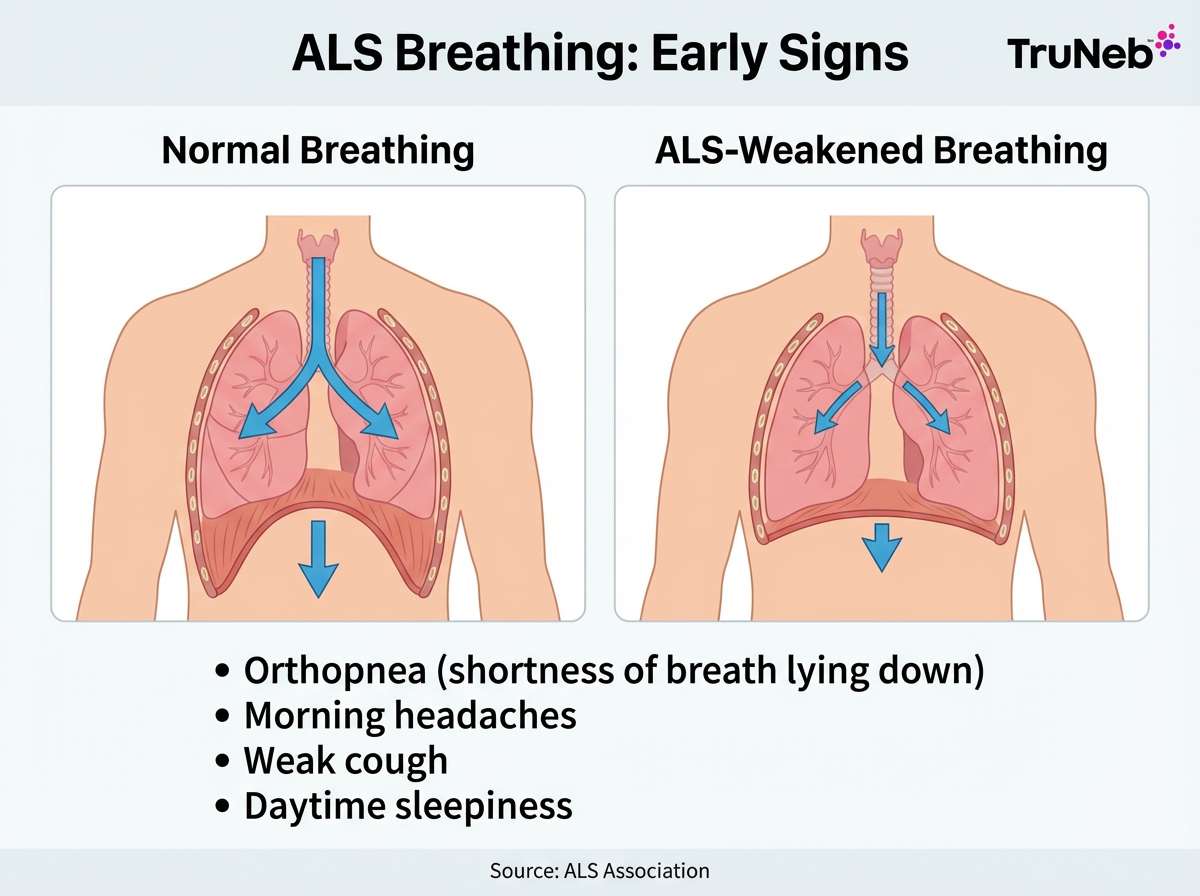
Your lungs are usually healthy at first, but breaths get smaller and coughing gets weaker.
Here are early changes to watch:
- Shortness of breath when lying flat (orthopnea)
- Waking at night feeling air-hungry or with a dry mouth
- Morning headaches or daytime sleepiness (carbon dioxide (CO₂) can build up overnight; this is called hypercapnia, or CO₂ retention)
- A weaker cough and more throat mucus
- A softer, breathy voice or needing more pauses between sentences to catch your breath
- Faster breathing during simple tasks like dressing
Tell your doctor if you notice these changes, especially if they're new or getting worse.
Key idea: ALS weakens breathing muscles, not the lungs.
How Doctors Check Your Breathing in ALS
Your ALS clinic team and pulmonologist use a few simple tests to spot changes early and match the right support.
- Spirometry: how much air you can blow out (forced vital capacity, FVC) and how fast
- MIP/MEP or sniff nasal pressure (SNIP): breathing muscle strength
- Night checks: oximetry or capnography to see oxygen and CO₂ while you sleep
- Symptom checklists: morning headaches, naps, or waking short of breath
You don't have to remember these names; your team uses them to track how strong your breathing muscles are and how well you clear carbon dioxide.
Key idea: Simple lung tests and nighttime checks can spot breathing problems before you feel short of breath in the daytime.
Airway Clearance That Works When Muscles Weaken
Mucus can sit deeper when muscles get tired. Clearing it regularly keeps you comfortable and helps prevent infections.
Your care team can show you how to:
- Use strong cough technique and huff coughing
- Try a manual assisted cough (a helper presses your belly as you cough)
- Use a cough assist device to boost cough strength
- Use gentle suction for saliva or secretions you can't clear
- Add moisture with humidified air and regular sips of water
Your respiratory therapist will show you which techniques are right for you and how to do them safely.
Key idea: Clearing mucus early and regularly keeps you more comfortable and helps prevent infections.
Nebulizers and Saline: Loosen Mucus, Make Coughs Count
Adding moisture can thin sticky mucus so each cough moves more. Clinics commonly use isotonic or hypertonic saline for this purpose. Hypertonic saline is a stronger salt solution that can pull water into mucus to loosen it. Hypertonic saline is prescription-only; only use it if your doctor recommends it.
If you see boxes labeled "steam inhaler," don't use those for breathing medications—those are different from nebulizers.
A portable mesh nebulizer is small and quiet, so you can fit a quick saline treatment into a morning or bedtime routine. Clean and dry your device as directed to lower infection risk. To explore portable options, including TruNeb, talk with your respiratory therapist.
Image prompt: Product shot of the TruNeb™ portable mesh nebulizer next to a small bottle of saline. Alt text: TruNeb™ portable mesh nebulizer on a table with saline vial.
Key idea: moist air and saline can make hard-to-move mucus easier to clear.
Noninvasive Ventilation (BiPAP): Sleep Better, Save Energy
Noninvasive ventilation, commonly called BiPAP, uses a mask to gently push air in when your muscles need help. A lot of people start at night and wake clearer, with fewer headaches and more energy.
Research summarized by the ALS Association shows that starting NIV when symptoms and tests first change can improve sleep and daytime comfort, and it's linked to longer survival in ALS. Your doctor will usually bring up NIV before breathing feels very hard, based on your tests and symptoms. Your team will fit the mask, set the machine, and check in regularly.
Image prompt: Close-up of a person resting with a BiPAP mask at night. Alt text: Person using a BiPAP mask while sleeping.
Key idea: Starting BiPAP at night can improve sleep, energy, and comfort as ALS breathing muscles weaken.
Breath Stacking and Cough Assist: Step by Step
Breath stacking helps you take a bigger breath so the cough is stronger. Learn it with your respiratory therapist.
Only practice breath stacking after your care team has shown you how; this guide is just to help you remember the steps.
Steps (general guide, not a medical order):
- Sit upright and relax your shoulders.
- Seal your lips around a mouthpiece or use your mask.
- Take a small breath in and hold it without letting air out.
- Add 2–3 more small breaths, stacking them.
- When your chest feels full, cough.
A cough assist device can push air in, then pull it out fast to copy a strong cough. Your clinic will teach the right settings and timing.
Key idea: a bigger breath makes a stronger cough.
ALS Breathing Support Timeline
Here’s how these tools usually show up over time.
ALS breathing support typically progresses from simple comfort steps to assisted ventilation, based on your symptoms, tests, and goals.
| Stage | Common signs | What usually helps |
|---|---|---|
| Early/mild | Breathlessness only with exertion; lungs are structurally normal but breathing muscles are weaker | Positioning, pacing activity, humidifier, airway hygiene |
| Night symptoms | Orthopnea, morning headaches, daytime sleepiness | NIV (BiPAP) is typically started at night. Teams can add cough assist and use saline via nebulizer to thin mucus |
| Daytime breathlessness | Winded with light activity, weaker cough | More frequent airway clearance, consider daytime NIV sessions, close follow-up |
| Severe weakness | CO₂ retention (hypercapnia), little speech, frequent infections | Full-time NIV or discuss tracheostomy ventilation based on goals |
Note: Plans are individualized with your ALS clinic. Tests and your goals guide each step.
Key idea: Breathing support usually builds up step by step—from simple positioning and humidifiers to NIV and, for some, tracheostomy—based on your symptoms, tests, and goals.
Tracheostomy and Invasive Ventilation: Big Decision, Plan Early
If breathing muscles get very weak, some people choose a tracheostomy and a ventilator that breathes through a neck tube. Only a small share choose this long-term path in the U.S. (about 5–10%), according to the ALS Association. It can extend life and usually needs 24/7 caregiver support, suction, and careful planning.
Talk with your care team early about your goals, comfort, and support at home so you can make the choice that fits you.
Key idea: plan ahead so the decision is yours, not made in a crisis.
Safety and Care Notes
- This guide is educational. Talk to your doctor before trying a new medication, changing oxygen, or starting devices like NIV, cough assist, or hypertonic saline.
- Keep vaccinations up to date (flu, COVID-19, pneumonia) to lower infection risk.
- Clean and dry masks, tubing, and nebulizers as directed.
- Watch for warning signs of CO₂ buildup: morning headaches, confusion, or rising sleepiness. Call your care team.
- Tell your doctor if breathing symptoms don't improve, suddenly worsen, or if you're thinking about changing any part of your breathing support plan.
- Have a written plan for chest colds: who to call, which treatments to use, and when to seek urgent care.
- ⚠️ If you have severe trouble breathing, chest pain, blue lips or face, or can't speak in full sentences, call emergency services right away.
Key idea: Keep your equipment clean, stay up to date on vaccines, and have a clear plan with your doctor for when breathing changes or infections hit.
Daily Tips to Breathe Easier
Small habits can make breathing more comfortable.
- Try sleeping with the head of the bed raised or on your side.
- Take breaks between tasks; sitting for showering and dressing can save energy.
- Smaller, more frequent meals can feel more comfortable because a full stomach can press on your diaphragm.
- Sip water through the day, and add humidity if your air is dry.
- Aim for a smoke-free space and avoid strong fumes.
- When traveling, pack masks, tubing, filters, power cords, and a backup battery, and check power and battery rules in advance.
Key idea: Simple changes in posture, pacing, and moisture can make day-to-day breathing more comfortable.
Frequently Asked Questions
Key idea: These quick answers cover common questions about BiPAP, oxygen, nebulizers, cough assist, tracheostomy, and travel with breathing equipment.
Tap or click a question below to see the answer:
Your doctor usually suggests BiPAP when your tests change (for example, a drop in forced vital capacity, FVC) or when night symptoms like orthopnea, morning headaches, or daytime sleepiness show up. It's a shared decision, not a fixed date.
Oxygen doesn't fix weak breathing muscles. Your team sometimes uses oxygen in certain situations, but the main help is ventilation support (like BiPAP) and airway clearance. Don't change your oxygen on your own; any changes should be made with your doctor.
Nebulized saline is commonly used to thin mucus. The type (isotonic vs hypertonic) and the schedule are decided by your doctor—this isn't medical advice. Always clean the device well.
Your therapist will set a plan based on your symptoms. A lot of people use it during colds and at set times each day to prevent mucus buildup.
No. In the U.S., only about 5–10% choose long-term tracheostomy ventilation, according to the ALS Association. It's a personal decision based on your goals and support.
Yes, with planning. Bring your equipment and extra filters, and a letter from your doctor if needed. Check power needs and battery rules with the airline before you go.
If you have questions about nebulizers, BiPAP, or other breathing support tools, reach out to our respiratory care team.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always talk to your doctor about your symptoms and before starting, changing, or stopping any treatment.