On this page

ALS and Breathing:
When Life Support Comes Into Play
This guide is for people living with ALS and families. It outlines noninvasive vs invasive ventilation, what a tracheostomy is, daily life on a ventilator, pros and cons, and choosing or declining a trach.
ALS affects the nerves that control muscles, including the muscles that help you breathe. ALS weakens the muscles that move air in and out of your lungs. The diaphragm and chest muscles tire over time, so breathing slowly becomes harder. This slow weakening can lead to respiratory failure.
Early clues include shortness of breath when lying flat, morning headaches, poor sleep, and daytime fatigue. These can mean carbon dioxide is building up because breaths are too shallow.
⚠️ If you or someone with ALS has sudden severe shortness of breath, chest pain, confusion, or trouble staying awake, call 911 or seek emergency medical care right away.
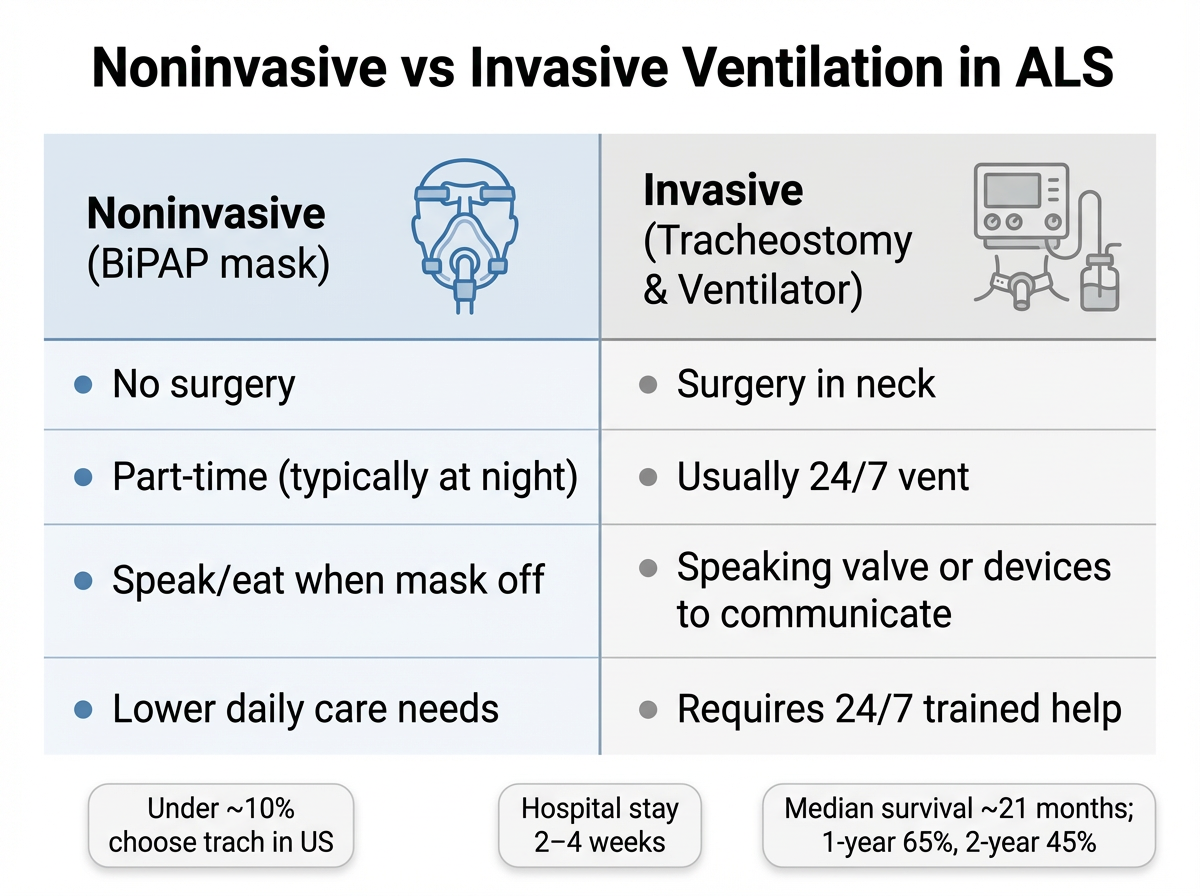
Most people start with noninvasive ventilation (NIV) like a BiPAP mask. It helps at night and sometimes during the day. NIV can improve comfort and buy time.
If NIV can’t keep oxygen and carbon dioxide at safe levels, your team might discuss invasive ventilation. That means a tracheostomy (a breathing tube in the neck) connected to a ventilator.
Bottom line: NIV is tried first; a tracheostomy is considered when the mask is no longer enough.
When to Consider a Tracheostomy in ALS
Timing matters. Some people plan the trach ahead with their clinic team. Others face the choice in a hospital if breathing fails and they can’t safely come off a breathing tube.
Your team might raise the option when NIV no longer keeps oxygen and carbon dioxide (blood gases) in a safe range, when infections keep coming, or when secretions make mask use unreliable.
Candidacy is about more than numbers. Age, overall health, how fast ALS is changing, caregiver support, and your goals all matter.
Only a small minority of people with ALS choose long‑term tracheostomy ventilation (under 10% in the U.S.).
Write your wishes down. Add them to your advance directive so emergency teams know what to do if you can’t speak for yourself. Share the plan with your family and clinic.
Bottom line: Plan early and document your wishes so the right decision is honored in an emergency.
ALS Tracheostomy Pros and Cons
Key takeaway: A tracheostomy can add time for some people with ALS, but it also brings 24/7 caregiving, higher costs, and major lifestyle changes.
| Pros | Cons |
|---|---|
| Extends survival by months to years for a number of people with ALS. | Requires 24/7 trained caregiving; emergencies can be fatal if no one is present. |
| Relieves the feeling of air hunger when breathing muscles fail. | Speech and natural eating are frequently lost; a large share of patients need a feeding tube. |
| Modern tech (eye‑tracking speech devices, portable vents) supports connection. | Does not stop ALS; paralysis and care needs continue to increase. |
| Can create time for milestones with family. | Higher infection risk and complex daily care (suctioning, supplies, maintenance). |
| Round‑the‑clock care can be physically and emotionally demanding; hiring skilled caregivers is expensive and usually not fully covered by insurance. |
Bottom line: A tracheostomy can add time, but it also adds 24/7 care and major lifestyle changes.
Tracheostomy in ALS:
Procedure and Hospital Stay
In surgery, a small opening is made in the windpipe (trachea). A trach tube goes through that opening and connects to a ventilator. You’re asleep during the procedure. Pain and discomfort are managed with anesthesia and medicines.
Afterward, teams set ventilator settings and teach caregivers how to manage the trach and equipment. Caregivers receive hands‑on teaching from the hospital team. People typically stay in the hospital two to four weeks while everything is tuned and training is complete.
If a feeding tube isn’t already in place, doctors typically place a PEG during the same hospitalization. It’s easier to do both while you’re under anesthesia and already recovering.
Bottom line: Expect about 2–4 weeks in the hospital to set up the ventilator and learn safe home care.
Life with a Ventilator After Tracheostomy
Daily life changes, but a steady routine helps. Most people are on the ventilator all day. Portable ventilators can mount on a wheelchair for outings.
A trained caregiver needs to be nearby at all times. Suctioning, tube checks, and troubleshooting alarms can’t wait. Families usually share shifts; some hire nursing help for parts of the day. Caregivers can get exhausted; build in breaks and outside help when possible.
For example, a typical morning might include checking settings, cleaning the trach site, suctioning, doing range‑of‑motion exercises, and setting up communication devices.
With planning, plenty of people still enjoy time with loved ones, shows, music, and computer use with eye‑tracking. It’s a team effort, but life continues.
Bottom line: Home life on a ventilator is possible, but it requires constant, trained caregiving.
Communication After an ALS Tracheostomy
Natural speech is usually not possible when the cuff is inflated because air bypasses the vocal cords. Some people can use a speaking valve at times if the cuff can be deflated and airflow allows it.
Most people lean on augmentative and alternative communication. Eye‑tracking computers, text‑to‑speech apps, and letter boards help you stay connected. Starting these tools early makes the transition easier. A speech‑language pathologist can help choose and set up the right tools.
Caregivers can also learn to read mouth movements and use simple yes/no signals to speed up daily conversations.
Bottom line: Plan for eye‑tracking or text‑to‑speech tools; they keep conversations going when voice is lost.
Nutrition and Care Routines
Most people get nutrition and hydration through a PEG feeding tube after a tracheostomy. It lowers the risk of aspiration and keeps calories steady.
Daily care includes suctioning as needed, cleaning the trach site, changing dressings, managing humidification for the ventilator, and watching for infection. A simple checklist posted at home helps keep tasks consistent and safe.
Physical therapy and gentle range‑of‑motion exercises, planned with your doctor or therapist, can help with comfort and circulation.
Bottom line: After a trach, most people with ALS use a PEG tube for safe, reliable nutrition.
Equipment, Costs, and Home Adjustments
A typical setup includes a portable ventilator (ideally with a backup), trach supplies, a suction machine, batteries, and a manual resuscitation bag for emergencies. A lot of homes add a hospital bed and reliable backup power.
Insurance (like Medicare) usually covers equipment rental and supplies. Most plans do not cover 24/7 caregiving. Families blend paid hours, family shifts, and respite options to make coverage work.
Ramps, doorway changes, and a wheelchair van can make daily life and appointments easier. Plan for charging schedules and power‑outage drills. Keep emergency numbers and a printed plan by the bedside.
⚠️ If the tracheostomy tube comes out or the ventilator stops and you can’t fix it quickly using your training, call emergency services immediately.
Bottom line: Insurance usually covers equipment, but not round‑the‑clock caregivers—plan support early.
Managing Secretions in ALS with a Tracheostomy
Weak cough and saliva control make mucus a daily challenge. Good airway clearance keeps you safer and more comfortable.
Key tools
- Suctioning through the trach removes pooled mucus.
- Cough assist devices push air in and pull it out to simulate a cough.
- Humidification and nebulized saline keep secretions thin.
Portable mesh nebulizers can deliver normal or hypertonic saline (3% or 7%) to help loosen thick mucus so it’s easier to suction. They’re quiet and battery powered, which makes daily care simpler.
Safety note: Always talk to your doctor before starting nebulized saline or any new medication, and follow their specific instructions.
⚠️ Products labeled "steam inhaler" are not the same as nebulizers and are not used to deliver ALS medications or saline through a trach.
Bottom line: Many care teams thin mucus and then clear it using a mix of saline nebulizers, cough assist, and suction.
ALS Tracheostomy Life Expectancy and Quality of Life
Research shows tracheostomy with invasive ventilation can extend life. One study reported a median survival of about 21 months after trach, with roughly 65% alive at one year and 45% at two years. Some live much longer; outcomes vary by age, health, and disease speed.
Quality of life depends on support, comfort, and communication. A lot of people who choose a vent and adapt report acceptable quality of life and would make the same choice again. Others find the limits too great. Honest planning helps avoid regret.
If someone later decides to stop ventilator support, medical teams can provide comfort medications and hospice care to help ensure they stay comfortable and their passing is as peaceful as possible.
Bottom line: Median survival after tracheostomy in ALS is about 21 months, but results vary widely.
If You Don’t Choose a Tracheostomy in ALS
Choosing comfort is a valid path. When NIV is no longer enough and a trach isn’t desired, hospice and palliative care focus on relief from air hunger and anxiety.
Medications like opioids and anxiolytics ease the sensation of breathlessness. These medicines are prescribed and adjusted by hospice or palliative care doctors. Teams also support the family and help you stay at home if that’s your wish.
Share your preferences early with your family and care team. Put them in writing so your wishes are honored.
Bottom line: Hospice teams focus on easing air hunger so the end of life is as comfortable and peaceful as possible.
Frequently Asked Questions
Tap or click a question below to see the answer:
Most people can’t speak with the cuff inflated. Some use a speaking valve at times if the cuff can be deflated and airflow allows it. Most people switch to eye‑tracking or text‑to‑speech devices.
Yes. ALS causes permanent respiratory muscle weakness. Once someone is fully ventilator‑dependent, they typically stay on the vent unless they choose to stop support with their medical team.
Plan on about two to four weeks for setup and training before going home.
Use battery backups and have a manual resuscitation bag ready, as trained by your care team. Keep an emergency plan posted and reviewed by all caregivers, and call emergency services if you can’t restore ventilation quickly.
In most Western countries, only a small percentage—usually under 10%—choose long‑term tracheostomy ventilation.
Insurance usually covers equipment and supplies, not 24/7 caregiving. Families blend paid help and family support.
Bottom line: A tracheostomy doesn’t stop ALS, but it can extend life when BiPAP isn’t enough. In short: Tracheostomy is a personal choice. Talk with your doctor and care team about what matters most to you, update your advance directives, and lean on palliative care and support resources as you plan next steps. Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always talk with your doctor about your symptoms, test results, and treatment options.